You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In recent years, clear aligner therapy has been enjoying increasing popularity, largely driven by patient demand for dental esthetics. Today, patients seeking orthodontic care expect treatment that not only addresses their desire for ideal smile esthetics, but also satisfies their expectations of convenience, affordability, and high quality in terms of delivery of care.1 Understanding these patient incentives that have helped spur the popularity of clear aligner therapy and focusing on addressing patients' primary concerns can provide the dentist with an additional skill set that can be incorporated into patient care. Most importantly, by acknowledging the patient's personal perception of their orthodontic problems-and by attending to their concerns and "wants" before advocating other recommendations- the clinician will be poised to "manage expectations" for the patient and to help the patient recognize the full scope of their dental needs. In this way, the clinician can amalgamate the patient's esthetic requests with the standard of care, using clear aligner therapy.
UNDERSTANDING THE PATIENT MINDSET
Providing optimal aligner treatment at your dental practice begins with understanding the patient's mindset about and perception of their dental wants and needs. Generally speaking, the patient mindset can be divided into three different types: positive, neutral, and critical.
The Positive Mindset: The patient with the "positive" mindset has overall good feelings toward the dentist and the practice, agrees to most of the treatments the dentist prescribes without argument, and, in general, trusts and respects the clini- cian. Communication with this patient starts with an already established trust and confidence in the dentist, and usually is less intensive in terms of effort and time. These patients need continued communication and demonstration of care to keep trust in place and support a continued positive practice.
The Neutral Mindset: For the patient with the "neutral" mindset, treatment decisions may be largely insurance- or cost-driven. These patients often are indecisive regarding the necessity of a recommended treatment, and in many cases, their dental care decisions may be swayed or driven by other people in their life, such as their spouse, family members, or friends. Clinicians will find that they need to spend slightly more time explaining treatment to these "neutral" patients, and may need to provide some more clinical education, as well. Unlike patients with the positive mindset, they tend to look for demonstrable outcomes and require assurances with regard to upcoming treatments.
The Critical Mindset: Finally, and not surprisingly, the most challenging patients are those with the "critical" mindset. These patients will find fault with much what the clinician does and demand more from the practice than is sometimes reasonable or feasible; they may expect a cost discount or a "guarantee" about the quality of the treatment. In many practices, the dentist and the dental team may find that they spend most of their time and energy attempting to satisfy the requests of the patient with the "critical" mindset. The best approach with these patients is to create a team-driven strategy to prioritize and allocate time, and to create communications that can address their needs.
CHANGING PATIENT PERCEPTIONS AND MANAGING EXPECTATIONS
Many patients are accustomed to, or at least expect, immediate satisfaction of their needs. They may wonder why they cannot simply have their teeth whitened and/or why they need to have their teeth cleaned before teeth whitening or other esthetic procedures, despite the fact that they may present with dentition for which prophylactic cleaning prior to treatment is essential. Patients often simply want the results or the service that they requested, and they want it quickly. For example, the perception of the patient in Figure 1 about her dentition may be only that she has a large gap between her upper front teeth, which she wants fixed to be esthetically pleasing. Meanwhile, the dentist, looking at the same smile, also sees occlusion, occlusal plane, vermilion border of lips, the interpupillary line with its relation to the midline of the face, and what the arrangement of teeth should be after the space or overlapping of teeth is corrected.
Here is where an understanding of the patient's mindset, as mentioned earlier, helps the clinician customize communications with the patient. The patient with the positive mindset is open to the clinician's suggestions, and educating this patient with regard to a demonstrable outcome-for example, long-term health outcomes in the case of the above-mentioned patient-will shift his or her perceptions.
For the patient with the neutral mindset, the patient's perceptions about his or her dental needs can be changed when the demonstrable outcome is also accompanied by a secondary resource or additional qualifying resource. For example, the clinician could show "before and after" images of patients with similar cases, both those that were successful and those that were ignored and untreated. Delving deeper into patients' hesitation with open-ended questions about what they define as their short- and long-term oral health outcomes and how they would like to achieve them are other approaches that can help these patients shift to a positive mindset.
As for patients with the critical mindset, while they are the toughest to change in terms of their perceptions, the clinician's role is to evaluate and address patients' oral health and to allocate resources to help these patients identify their pain points, hear their concerns and address them, and provide whatever educational resources and logistic support are necessary. Sometimes, however, even these efforts may not be successful. At this point, the practition- er may decide to try to achieve this particular patient's oral health outcomes in smaller "sprints" of treatment or to allow the patient to come back when he or she is ready.
By recognizing patient perceptions, the dental clinician can pave the way toward fostering the patient's acceptance or willingness to consider treatment recommendations that may extend beyond those that the patient expects or wants. This process of "changing expectations" begins with addressing the patient's chief concern or "wants" first, before making additional treatment recommendations to address the patient's other "needs."
Uniting Standard of Care With Patients' Esthetic Needs
It may sometimes seem to the clinician that providing standard of care treatment may be at odds with patients' requests for improving specific aspects of the esthetic appearance of their teeth. Yet standard of care treatment can indeed be symbiotic with fulfilling a patient's esthetic needs. This process begins by identifying the patient's chief concern, and by acknowledging the patient's perception of their needs. For example, a patient such as the young woman in Figure 1 may, after seeing some TV ads on aligner therapy and perhaps doing some cursory online research, decide that clear aligner therapy is appropriate for her. She may also believe that it should be relatively simple to correct the "spacing problem in her anterior upper teeth." For the prudent practitioner, addressing this chief complaint of the patient with regard to esthetics is the first step in standard of care treatment, followed by clinical diagnosis and a treatment plan.
Addressing the patient's primary complaint begins by having an honest conversation with the patient about their concerns, as well as educating them on the condition of their teeth and the extent of the treatment that would be needed to address the chief problem. This conversation should include the notion of esthetics versus function, and the future consequence of delaying a particular dental treatment. Therefore, when it comes to clear aligner treatment options, the conversation with patients who have either the positive or the neutral mindset should begin with a discussion about whether the patient is a suitable candidate for clear aligner therapy as an esthetic solution, rather than for treatment with traditional fixed orthodontic appliances. While many patients would prefer clear aligners because they are more esthetically attractive and comfortable than traditional orthodontics, and because the aligners are removable,2,3 clear aligner therapy is not the optimum treatment for some cases requiring more complex tooth movements, such as extrusion or correction of severe rotations.4 Clear aligner therapy is, however, ideal for mild to moderate cases of malocclusion.2 Indeed, some studies have demonstrated the effectiveness of aligner therapy for selected mild to moderate cases to be similar to that of fixed appliance orthodontic treatment.5,6 The literature has shown that with advances in clear aligner therapy, software progress along with customized composite attachments mostly likely can increase the effectiveness of orthodontic treatment with clear aligners, improving anterior root torque, rotation, and mesial-distal (M-D) movement; clear aligners can also increase posterior anchorage. Clear aligner techniques are continually evolving owing to the development in materials, auxiliaries, and computer programming, resulting in greater effectiveness of and more advanced clear aligner treatments.7,8
For the patient in Figure 1 (left panel), understanding her perception of "wants" versus "needs" is key. For example, the patient's perception is that the gap between her upper incisors "needs" to be closed and she "wants" to close the diastema using clear aligners. The clini- cian's thoughts on the treatment process, on the other hand, may include evaluation of the upper and lower arch form; making sure the patient will have a stable bite at the end of treatment; ensuring there is no unwanted collision with the lower anterior arch as the diastema on the upper arch is closing; determining whether there will be a need for lingual tipping of upper incisors; and, most importantly, avoiding a potential posterior open bite, which can create a greater malocclusion. Therefore, an ideal process would be to evaluate the patient's candidacy for aligner treatment (and quickly educate the patient concerning this), addressing both esthetics and function and creating a proper balance between the "wants" and the "needs" of the patient. The clinician can discuss what would be involved in the treatment plan to address the patient's chief complaint and how quickly treatment is expected to be completed. The conversation about the overall plan should also include information on which companies offer the particular aligner treatment, as well as on the hybrid partner networks that help facilitate the clear aligner treatment. The clinician should explain that such partner networks assist patients in locating an in-network dentist to perform their oral evaluation before aligner treatment, after which teledentistry with the clear aligner company's treating clinician and team members help ensure proper aligner tracking and adjust the aligner treatment as needed. The affordability of the treatment plan should also be reviewed with patients, as having the option of a low-cost treatment alternative that addresses their anterior or cosmetic concerns is often a primary incentive for their choosing aligner therapy1-and may therefore be a determinant in their decision-making. Once the clinician has engaged the patient in this honest conversation, in the context of addressing the patient's chief concern or "wants" first, the patient will be more comfortable listening to the clinician's assessment of any additional dental problems that he or she might have, as well as be more receptive to any further recommendations. Thus, the patient will be fully informed of all treatment options that address both their "wants" and their "needs." The right panel of Figure 1 shows the treatment outcomes after the patient's chief concern has been addressed.
In this way, by identifying and attending to the patient's perceived foremost needs, the clinician can better facilitate providing standard of care treatment with clear aligners. For the prudent practitioner, addressing a patient's "chief" concern and providing standard of care treatment ultimately will go hand-in-hand, whether the treatment is provided by the practitioner or made through a referral to an orthodontic specialist.
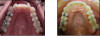
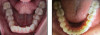
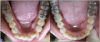
For example, a 28-year-old female patient presented with malocclusion, for which she had previously been offered multiple treatments. Treatments for malocclusion ranged from fixed orthodontic appliances to the extraction of bicuspids. The patient was concerned about the treatment timeline and the cost of the fixed orthodontic treatment, and wanted to avoid the extraction of healthy bicuspid. The patient's perception of her problem was that she required orthodontic treatment that would provide a better smile line, at an affordable cost (Figure 2, left panel). From the clinician's perspective, the patient exhibited overbite, open bite, and overjet of lateral incisors of 4 mm, along with an edge to edge posterior occlusion with a unilateral crossbite (Figure 2, right panel). The clinician reassured the patient that bicuspid extractions would not be necessary, and presented her with a clear aligner esthetic treatment plan. Understanding the clear aligner parameters can aid the treating clinician in better explaining the treatment plan. The clinician reviewed with the patient the need for the expansion of the upper posterior arch on both sides by 2 mm and the anterior proclination by up to 4 mm-all of which are within the aligner capacity, regardless of which aligner plastic is utilized-and that there would be some sensation of pressure during active aligner treatment. The clinician also reviewed patient aligner wear and compliance. The patient's aligner journey began with her shifting from a "neutral" mindset to a "positive" mindset by the start of her treatment. During the 6-month progress of her tooth movements, the patient reported that she was pleased with her smile line (Figure 3, left panel), but from the clinician's perspective, the teeth alignment was not yet ideal (Figure 3, right panel). At this point, it was easy for the clinician to explain to the patient the clinical need to continue with treatment, as the patient now trusted the practitioner and the process. The clinician shared with the patient the advantages and disadvantages of interproximal reduction (IPR) along with intruding the lower anterior teeth to achieve an improved occlusal plane. At this point, the patient was receptive to the clinician's recommendations and was willing to pursue further treatment to achieve the ideal results that the clinician envisioned. Since that time, the patient has become a champion of patient referrals to the office, as she is happy with the results of aligner treatment.
TOOTH MOVEMENT CONCEPTS
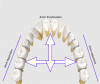
As explained earlier, clear aligner therapy is ideal for mild to moderate cases of malocclusion.9In the author's experience, the 2,4,6 rule, developed by the author, provides exact guidance in determining case complexity. According to the 2,4,6 rule, a moderate malocclusion is defined as 2 mm or less of correction needed for the midline, intrusion, extrusion, and crossbite; 4 mm or less of correction needed for the open bite and overjet; and 6 mm or less of crowding or spacing in the anterior arch cuspid to cuspid. Bicuspid and anterior rotations of 25 degrees or less would also yield a moderate clear aligner treatment (parameters are shown in Figure 4). This chairside case evaluation system enables the clinician to quickly identify whether the patient is a candidate for clear aligner treatment, and provides a starting point for the conversation with the patient about their orthodontic needs.
When discussing tooth movement concepts with the patient who opts for aligner therapy, it is always best to convey the esthetic and functional goals of the treatment based on clear aligner capacities. Orthodontic tooth movement results from resorption and formation of the alveolar bone in response to the application of load.10 Typically, each aligner is preloaded to achieve approximately 0.25 to 0.30 mm of load. With clear aligner therapy, teeth can be moved forward and tucked back lingually if necessary, keeping the root apices within the bone but tipping in multidirectional movements to gain better esthetic alignment. In some cases, teeth can be moved linearly, but this will be considered a translation movement and exceed the mild to moderate teeth movements. Cases of anterior crowding of 4 mm or less can be treated without attachments and without interproximal tooth reduction (IPR), and instead by adding posterior expansion of 2 mm, yielding better anterior esthetics without the proclination of the lower anterior arch beyond 4 mm (Figure 5). The root apex position remains the same, with only the crown portion of teeth being proclined buccally or lingually. In some cases, anterior overlapping/crowding may need IPR when sufficient space cannot be created for teeth movement alone by posterior expansion and anterior proclination.
Case Studies
Moderate Malocclusion of the Maxillary Arch and Mandibular Arch Treated With Clear Aligners Without Interproximal Reduction
A 58-year-old male patient presented with a chief concern of overlapping maxillary and mandibular lateral incisors (Figure 6 and Figure 7, left panels). The patient's treatment options were reviewed, and clear aligner therapy was chosen. Given the 2,4,6 rule of the aligner parameters set by the clinician, posterior arch expansion of 4 mm with the added anterior proclination of 2.5 mm in the upper arch was implemented. Because the lateral incisors were rotated less than 25 degrees (Figure 6, left panel), additional attachments were not needed. By uprighting and expanding the upper arch from premolar to molar regions, which can be expressed as posterior arch expansion, rotation of the lateral incisors into better anterior arch position was allowed. As the upper lateral incisors rotated into better position, a visible incipient decay was noted mid-treatment on the mesiolingual surface of tooth No. 10. This incipient caries, which was not clear on the 2D radiographs nor visible during the examination, was restored while the overlapping of the lateral incisor over the adjacent central incisor No. 9 was corrected, and the patient was spared potential further degradation of the tooth structure. Thus, clear aligner treatment was able to provide the patient with good results without the need for IPR treatment and helped achieve better oral health (Figure 6, right panel).
A similar strategy was followed for the same patient's lower anterior malocclusion requiring posterior arch expansion, creating room for the lower anterior arch alignment (Figure 7, left panel). Using clear aligner therapy, the same parameters as in the upper arch were followed by bicuspid to molar teeth uprighting, creating an expansion of 1.5 to 2 mm in each posterior quadrant, along with an approximate anterior proclination of 2 mm. After less than 1 year of treatment, the patient was moved into bite stabilization with no active tooth movement for 6 to 8 weeks, finishing the upper and lower arch in 1 mm overjet and overbite on the anterior arch coupling (Figure 7, right panel). A final retention option of lingual lower wire and clear upper aligners was used for 24 months, prior to moving into all-removable retention and night-time wear. The patient has been pleased with the treatment of his chief concern and has been in a "positive" mindset, becoming an advocate of the clinician, the practice, and the process.
Advanced Malocclusion of the Mandibular Arch Treated With Clear Aligners and Interproximal Reduction
In some cases, anterior overcrowding cannot be treated with posterior expansion and anterior proclination alone, and additional space for alignment may thus need to be provided by means of IPR. For the 44-year-old female patient shown in Figure 8 (left panel), IPR was needed to fit the crowded incisor into the mandibular arch. Lower anterior crowding was presented in excess of 4 mm of overlapping with lingual inclined incisors and cuspid No. 22. Posterior expansion up to 4 mm from molar to bicuspid will create room for better alignment on the mandibular ridge, helping resolve some of the lower anterior crowding up to 4 mm; however, an additional 2 mm of IPR will be needed, as the patient's lower arch malocclusion is presented with 6 mm of anterior crowding. Thus, an approximate 0.3 to 0.4 mm IPR will be required on the lower anterior arch cuspid to cuspid in order for the additional space to align the lower anterior arch. The patient's mandibular overcrowding was treated with posterior expansion of 2 mm per quad from molar to bicuspid, yielding 4 mm of expansion, anterior proclination of 3 mm, along with 0.3 mm of IPR between teeth Nos. 22 through 27. After 8 months of treatment with a once-weekly aligner change, the patient was pleased with the results and bite stabilization, and retention was initiated (Figure 8, right panel). In a study evaluating 376 patients who had received interproximal enamel reduction treatment, risk of tooth decay was not increased and no significant increase in sensitivity was observed.11
BENEFITS OF CLEAR ALIGNER THERAPY
Both clear aligners and fixed orthodontic braces have several advantages as well as disadvantages in treating different types of malocclusion. Clear aligners have the advantages of segmented movement of teeth and shortened treatment duration, but they are not as effective as traditional fixed orthodontics in producing bodily movements, providing adequate occlusal contacts, and controlling teeth torque.8 For example, with clear aligners, posterior dental arch expansion beyond 4 mm and translative tooth movements are difficult to achieve, and it may be preferable to use traditional fixed orthodontics for such cases. On the other hand, clear aligners are ideal for addressing crossbite of 2 mm or anterior crowding or spacing of up to 4 to 6 mm via clear aligner tipping movements.
Overcrowding and overlapping of anterior teeth are conditions that need to be treated not only to achieve good esthetic results but also to maintain a healthy periodontium. According to one clinical study of the relationship between irregularity of teeth and periodontal disease, overlapping of incisor teeth has been found to be directly related to gingivitis, a relationship that was believed by the researchers to not be explained simply by matters of oral hygiene.12 This is in part because straight teeth are easier for patients to clean and are associated with better maintenance of periodontal health.12 Clear aligner therapy is also useful for treating traumatic occlusion that has resulted in abfraction, can help provide functional and stable occlusion that is in harmony with the temporomandibular joint, and can offer an alternative to aggressive restorative solutions for certain orthodontic problems.13
A recent study found a maxillary and mandibular irregularity index of 4 to 6 mm for 84.6% and 81.1% of patients, respectively.14 Such cases, as well as other mild to moderate cases of malocclusion, are ideal for treatment with clear aligner therapy.
Although veneers can be used for esthetic treatment, they have a finite life expectancy, and when replacement of veneers is needed, tooth structure is removed, leading to pulp damage.15 Orthodontic treatment, by contrast, preserves tooth structure and tooth anatomy, while its results often last for a lifetime.15
In addition to its other many benefits, clear aligner therapy can, depending on the aligner company, be delivered via partner networks that combine teledentistry with in-person office visits. Teledentistry and monitoring tools for the patient have thus played an important role in clear aligner therapy, allowing patients to receive orthodontic care in real-time via period- ic alignment check-in visits with the treating clinician and qualified treating team members. Teledentistry has been found to be effective for monitoring ongoing clear aligner treatment progress,16 adding to the convenience and overall improved patient experience that aligner therapy affords.
Conclusion
Clear aligner therapy not only corrects the esthetic issues associated with irregularities, overcrowding, and overlapping of the teeth, but also addresses the functional and periodontal health problems that may likewise result from malocclusion. Patients who request clear aligner therapy to address a specific esthetic problem present the clinician with an opportunity to educate them on additional dental problems that they may have, and on how clear aligner therapy options can help. By addressing the patient's chief concern and "wants" first, the clinician will enable the patient to see visible proof of the benefits of aligner therapy, thereby spurring the patient's interest in and commitment to further treatment recommendations. In doing this, clinicians should strongly consider collaborating with the right partner network for clear aligner therapy, as such networks will ensure a quality process and materials, as well as cutting-edge technology-which in turn will help provide patients with the standard of care they require for their "needs."
About the Author
Payam C. Ataii, DMD, MBA
Senior Vice President Orthodontic Support
Aspen Dental Management
Laguna Hills, California
DISCLOSURE: Dr. Ataii is a clinical advisor for the National Academy of Dental Professionals and a clear aligner advocate for multiple aligner companies, both traditional and hybrid teledentistry models. Dr. Ataii has been a paid consultant for SmileDirectClub™.
Dr. Ataii received an honorarium from SmileDirectClub™ for writing this article.
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com
References
1. Okuda BC, Tabbaa S, Edomonds M, Toubouti Y, Saltaji H. Direct to consumer orthodontics: exploring patient demographic trends and preferences. Am J Orthod Dentofacial Orthodped. 2021;159(2):210-216.
2. Azaripour A, Weusmann J, Mahmoodi B, et al. Braces versus Invisalign®: gingival parameters and patients' satisfaction during treatment: a cross-sectional study. BMC Oral Health. 2015;15:69.
3. White DW, Julien KC, Jacob H, Campbell PM, Buschang PH. Discomfort associated with Invisalign and traditional brackets: a randomized prospective trial. Angle Orthod. 2017;87(6):801-808.
4. Rossini G, Parrini S, Castroflorio T, Deregibus A, Debernardi CL. Efficacy of clear aligners in controlling orthodontic tooth movement: a systematic review. Angle Orthod. 2015;85(5):881-889.
5. Ke Y, Zhu Y, Zhu M. A comparison of treatment effectiveness between clear aligner and fixed appliance therapies. BMC Oral Health. 2019;19(1):24.
6.Yassir YA, Nabbat SA, McIntyre GT, Bearn DR. Clinical effectiveness of clear aligner treatment compared to fixed appliance treatment: an overview of systematic reviews [published online ahead of print January 6, 2022]. Clin Oral Investig. doi: 10.1007/s00784-021-04361-1.
7. Nucera R, Dolci C, Bellocchio AM, Costa S. Effects of composite attachments on orthodontic clear aligners therapy: a systematic review. Materials (Basel). 2022;15(2):533.
8. Ke Y, Zhu Y, Zhu M. A comparison of treatment effectiveness between clear aligner and fixed appliance therapies. BMC Oral Health. 2019;19(1):24.
9. Weir T. Clear aligners in orthodontic treatment. Aust Dent J. 2017;62(Suppl 1):58-62.
10. McCormack SW, Witzel U, Watson PJ, Fagan MJ, Groning F. The biomechanical function of periodontal ligament fibres in orthodontic tooth movement. PLoS One. 2014;9(7):e102387.
11. Jarjoura K, Gagnon G, Nieberg L. Caries risk after interproximal enamel reduction. Am J Orthod Dentofacial Orthop. 2006;130(1):26-30.
12. Ashley FP, Usiskin LA, Wilson RF, Wagaiyu E. The relationship between irregularity of the incisor teeth, plaque, and gingivitis >3mm. Eur J Orthod. 1998;20(1):65-72.
13. Svitlana K. T-Scan occlusal analysis after adult orthodontic treatment. J Clin Orthod. 2016;50(8):466-457.
14. Asiri SN, Tadlock LP, Buschang PH. The prevalence of clinically meaningful malocclusion among US adults. Orthod Craniofac Res. 2019;22(4):321-328.
15. Christensen GJ. Are veneers conservative treatment? J Am Dent Assoc. 2006;137(12):1721-1723.
16. Park JH, Kim JH, Rogowski L, Al Shami S, Howell SEI. Implementation of teledentistry for orthodontic practices. J World Fed Orthod. 2021;10(1):9-13.