You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In 1967, Dr. Herbert Schilder, one of the pioneers of modern endodontics, introduced the concept of filling root canals in three dimensions (3-D).1 In the ensuing 30 years, advances in technology, such as the introduction of nickel-titanium (NiTi) rotary instrumentation, digital radiography, apex locators, ultrasonics, irrigation systems, magnification, illumination, and more efficient instrumentation and obturation methods have allowed us to consider the fourth dimension: time.2 In this article, the author will define efficiency as a clinical concept and discuss its application to the practice of modern endodontics.
It is important to clarify the notion of time as a clinical factor during the rendering of care, so that efficient endodontic care is not confused with fast, sloppy care. Efficiency is defined as the ratio of useful energy delivered by a system to the total energy supplied to it. Essentially, analysis of the efficiency of a system measures the waste of effort by the system and compares how much effort will comparatively get the same results. Systems that produce less effort to produce the same output more quickly are considered more efficient. However, efficiency does not quantify the quality of work and, consequently, given the same quality output, there are more- and less-efficient means of achieving results; these involve establishing robust systems that create a smooth work flow that generates reproducible results.
It is very important to understand that efficiency analysis in endodontics also assumes a constant quality of care and, therefore, higher efficiency does not mean a lower quality of care. This quality of care is set by each practitioner for his or her particular philosophy of practice; setting the highest standard of care is the obligation of each practitioner. Given a specific standard, there are more- and less-efficient ways to achieve such results.
Similarly, astute clinicians understand that efficiency and quality of care are not mutually exclusive. For years, academic mentors warned dentists about the consequences of rushing through an endodontic procedure and failing to adhere thoroughly to the endodontic axiom of effective cleaning, shaping, and obturation of the root canal system. Any discussion of how rapidly a procedure was completed was taboo and seemingly reflected a lack of desire on the part of the practitioner to attain high ideals of care or to adhere to world-class standards. However, as mentioned earlier, efficient care does not imply fast, sloppy care with a lower standard. Instead, efficiency uses technical systems to achieve the desired standard of care faster. It simply means reducing waste in clinical practice, not compromising quality. This discussion can best be demonstrated by a clinical case.
Case Study
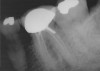
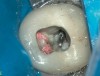
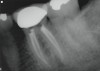
A 40-year-old man presented with a chief complaint of occasional chewing discomfort in a tooth with a history of endodontic therapy (Figure 1). The patient recounted a 1-hour visit with his dentist for the root canal therapy and subsequent visits to fabricate the crown. Eight months after the initial root canal therapy and coronal restoration, mild chewing discomfort persisted in the tooth. After discussing options and giving consent, a nonsurgical re-treatment through the new crown with intracoronal removal of the post was performed to address the patient’s chief complaint while attempting to retain the new crown (Figure 2). A 1-hour appointment was necessary to achieve these objectives (Figure 3). The patient’s symptoms disappeared and the access preparation was subsequently restored.
This case best explicates the word efficiency as it pertains to clinical endodontics. While the original root canal and the re-treatment were both performed within the same time frame, the quality, the standard of care, and, inevitably, the outcome were dissimilar in the same tooth. The first procedure was performed quickly; the second was done efficiently. This brings up the question of skill and experience as functions of efficiency in clinical procedures.
Defining Skill
Skill may be defined as the conscious interaction of knowledge, desire, and practice. Gaining any skill is a function of having the desire to gain the necessary knowledge and then further developing it through practice. In endodontics, these ideals along with effective anesthesia, patient management, proper access, and effective instrumentation and obturation lead to optimal results. If achieving quality results is the same as going from point A to B, the efficient practitioner’s course can be plotted as a straight line (Figure 4). The inefficient practitioner will waste time and while obtaining similar results, the procedure will take longer to perform.
Performing procedures efficiently is not only a matter of productivity; it is also a matter of responsible patient service. Because endodontic therapy often is not an elective procedure, given the same optimal outcome patients would clearly choose more efficient techniques to achieve their results. This is why efficiency is a priority as a matter of good service and the obligation of all conscientious clinicians to their patients. All procedures should be streamlined and efficient systems should be installed so that patients can be served effectively without wasting their time. Efficiency of care during a patient visit for root canal therapy can be broken down to two basic areas of service: those systems that improve the efficiency of the clinical procedure while maintaining quality, and those that improve the patient management as a whole (Figure 5). Efficient clinical procedures should create a smooth flow for the actual procedure (dealing with just the tooth), and efficient patient management systems should create a smooth operation of the non-clinical aspect of care (dealing with the patient as a whole). This can be anywhere from the time the phone is an-swered by front desk staff all the way to the patient’s postoperative visits and the communication of continuity of care issues.
Clinical Milestones
As far as patients are concerned, efficiency of care is a continuum that begins from the time they contact the office to schedule an appointment until the procedure is complete and optimal results are achieved. However, discussion of efficiency in the non-clinical, managerial aspects of the treatment is beyond the scope of this article and we will therefore focus on the clinical aspects of care. To discuss efficiency in clinical endodontics clinicians should evaluate its role during the important clinical milestones of any given procedure. These milestones are the clinical diagnosis, administration of anesthesia, access opening, irrigation, instrumentation, and obturation of the root canal.
Diagnosis
Although endodontic diagnosis is often a straightforward process, correctly diagnosing early irreversible pulpitis, discerning referred pain, or differentiating odontogenic vs non-odontogenic pain is often a challenging process. Because pain is a highly subjective experience, efficient diagnosis can only be made through a systematic analysis of the presenting clinical signs and a thorough review of the history of symptoms using a visual pain analogue scale (describing all symptoms on a scale of 0-10). To avoid skipping important information during the diagnostic cascade, a pain-history questionnaire should be filled out by all patients presenting with a chief complaint of pain in the orofacial region. This questionnaire helps the patient to understand and be better able to verbalize his or her pain before the chairside interview.
A thorough compilation of the medical/dental history by the nurse, hygienist, or a well-trained dental assistant before spending time with the endodontist helps focus the patient’s chief complaint to the relevant information and allows the endodontist to use his or her time more effectively to make a correct diagnosis. This way, this information can be filtered and summarized in a constructive way before the endodontist’s initial evaluation of the patient. Training the office staff to effectively understand the pathologic process, ask the right questions during the clinical interview, and to further evaluate and communicate this information to the endodontist can help expedite the diagnostic process. As a rule of thumb, whenever a definitive diagnosis cannot be reached with a high degree of confidence, referral to a specialist or monitoring the symptoms without irreversible treatment is imperative. Initiating root canal therapy in a tooth without adequate evidence should be avoided at all cost.
Anesthesia
Effective pain control is one of the most important aspects of the patient experience in the dental office and directly correlates to patients’ perception of the care rendered to them. A radiographically perfect root canal procedure that is performed under less than total anesthesia can adversely affect the patient’s confidence in the endodontist and his/her clinical skills. For utmost efficiency during the clinical procedure, effective, profound anesthesia is of paramount importance. If anesthesia is inadequate, multiple interruptions will decrease efficiency while reducing patient confidence. It is, therefore, important to ascertain pulpal anesthesia with standard vitality tests (electric pulp tester or cold/thermal tests) immediately before rubber dam isolation and access preparation.3
Should conventional anesthesia fail, intraligamental and intraosseous anesthesia should be administered at once. It is important to realize that the duration of anesthesia for these two techniques is less than the conventional methods; hence, they should not be used as the primary method of anesthesia in molar endodontic therapy, where a full pulpectomy may take longer than the effective duration of their action. Duration of pulpal anesthesia for 2% lidocaine 1:100,000 administered with a conventional nerve block is only 45 to 60 minutes vs 90 minutes of soft tissue anesthesia.4 Therefore, efficient pulpectomy is essential in avoiding the anesthesia wearing off during or toward the end of the procedure.
The most important factors for efficiency in anesthesia are effective delivery of enough anesthetic to the right anatomical location, testing the vitality before starting the procedure, and delivering more anesthetic via intraligamental and intraosseous injections if conventional anesthesia fails, testing again, and starting the procedure only when full pulpal anesthesia has been achieved. This is one area where adequate time is necessary for effective work. Intraosseous anesthesia can be used as a primary method of anesthesia in the anterior and some premolars that have conventional, uncomplicated anatomy, where the root canal therapy can be performed efficiently within the duration of action of the anesthetic, and where the patient understands the anesthetic method. Conventional techniques are adequate in terms of the quality of anesthesia as long as proper techniques are employed. Therefore, the utmost efficiency is gained by techniques that render adequate duration of anesthesia for a given procedure and also by assuring complete anesthesia has been achieved before starting a case so that multiple interruptions are not necessary.
Access
Proper access preparation is not only a key to successful endodontic therapy, it is also crucial to efficient instrumentation and obturation. A lack of understanding of proper access principles can prevent efficient flow of instrumentation by difficult visualization of the orifices or potential ledges and steps that create wasteful motions. Our understanding of endodontic access has evolved over the past 20 years. While dentists used to think of endodontic access preparation as the process of gaining access to the canal orifices, it is now understood that the purpose of access preparation is gaining straight-line access to the apical one third of each root canal.
It is important to spend adequate time preparing the correct access—one that is neither too small nor too large—with proper convenience form so that excessive time is not wasted later because of complications of instrumentation. The axial walls of the access preparation should flow smoothly into the orifices, without any ledges or steps that interrupt smooth instrumentation. The use of orifice shapers, Gates-Glidden burs, and a crown-down preparation in the coronal one half of the canal is very important as they allow straight-line access into the apical one third. The end result of correct access is that an instrument in any given canal should stand straight in the tooth and parallel to the long axis of its corresponding root trunk. If a file enters a canal orifice with sharp deviation from the root’s long axis, it will be potentially exposed to multiple bends along its journey to the apex, not only predisposing it to fracture, but also creating less efficient instrumentation.
A thorough understanding of pulpal morphology is crucial in efficient exploration and discovery of any additional canal. It is very important to understand that additional canals are present most of the time in both maxillary and mandibular molars, and to be efficient in locating and treating them. Digital radiography, a technology that has greatly helped improve endodontic efficiency, allows for taking multiple exposures before and during the access preparation to find the chamber and diagnose the potential presence of additional canals. Studying multiple-angle radiographs before the clinical procedure aids greatly in having a more realistic picture of what to expect during the access preparation and instrumentation of the root canals. Incorporating preoperative bite-wing radiographs to measure the depth of bur penetration and its angulations greatly helps to expedite the access prep-aration and helps to reduce the uncertainty with the process. In angulated or calcified canals, digital radiographs allow for taking multiple radiographs mid-operation to align the bur properly and make course adjustments.
Occlusal adjustment, flattening of the cusps, and removing the tooth from occlusion before the access preparation can potentially produce a more stable reference point and reduce postoperative discomfort resulting from high occlusion. The most common error in access preparation is underpreparing the access. This makes instrumentation more difficult and increases the chance of missed canals. While there is a balance between the endodontic needs to prepare an adequate size access—one that ensures successful management of the apex—and the restorative needs of preserving tooth structure, it is important to understand that saving tooth structure at the expense of missing canals and performing root canals that are less effective at achieving length are rationally unsupportable positions. The endodontic needs for effective cleaning and shaping of the canals while reducing the risks of missing canals, instrument separation, ledging, and other procedural errors take precedence over restorative needs because promoting a healthy, infection-free foundation is mandatory before the restoration of the tooth. If such a healthy environment is not achievable, the tooth should be removed, not restored. Too small of an access that preserves tooth structure but results in a missed or ledged canal and chronic infection does not serve the patient in any beneficial way.
Irrigation
Because irrigation is an important component of successful endodontic therapy and because it has been shown that the volume of irrigant is a significant factor in clearing debris from the canal, efficient techniques that employ high volumes of irrigant should be used liberally for the best outcome. Positive pressure irrigation through a syringe combined with suction has been the traditional canal irrigation method. A new technique using negative pressure has recently been introduced with the promise of improved quality of irrigation through the safe delivery of high volumes of irrigant deep into the canal.5 While its efficacy is yet to be demonstrated, the goal of combining irrigation and suction can potentially improve efficiency and safety for a given volume of irrigant. For all clinicians, however, the use of larger irrigation syringes (10 cc to 20 cc) instead of smaller ones can reduce the frequency of syringe reload during the procedure, thus improving efficiency (Figure 6). Multiple irrigants may be required during a procedure for disinfection and removal of the smear layer. Having these irrigants in large syringes and readily available can help improve the flow of the procedure.
Another device that helps to improve both the quality and efficiency of irrigation is the use of piezoelectric ultrasonics. Ultrasonic energy enhances irrigation by activating the irrigant through the three physical mechanisms of cavitation, agitation, and acoustic streaming. By increasing the kinetic energy of the irrigant, these three physical phenomena act like catalysts and can potentially increase irrigation efficiency.6 Anecdotal claims about an absolute length of time an irrigant should be in contact with the canal walls can best be addressed by adding ultrasonic energy to the irrigant to help expedite the cleaning of canals. The use of ultrasonics during instrumentation can help remove debris more efficiently from fins, isthmuses, and aberrant anatomies.7 Many small, powerful ultrasonic units are available on the market and should be employed during many phases of conventional and surgical endodontic therapy.
Instrumentation
One of the most significant advances in the efficiency of modern endodontic therapy has been the advent of NiTi rotary instrumentation. Engine-driven instrumen-
tation has significantly improved instrumentation efficiency and although effective hand instrumentation may still produce a sufficient quality of care, the overall efficiency rendered by engine-driven NiTi instruments has made them the standard for efficiency of care. Many systems are currently available on the market with various design features, and while engine-driven instruments are more efficient than stainless steel hand files, the efficiency of all NiTi instruments is not the same. For example, instruments that have land areas in their cross-sectional design generally remove dentin by crushing it vs cutting it and are, therefore, less efficient than files with triangular cross-sections with cutting blades. Instrumentation technique is also a factor of efficiency. Crown-down techniques help improve apical tactile feedback and help to facilitate negotiation around curves. Systems that use numerous files are also less efficient than those that use fewer files to achieve the same result. Clearly, the necessary number of files should be a balance between the need for efficiency and the need for preventing file fracture because of excessive torque on a given file. It is important that the incidence of procedural errors such as ledging, zipping, canal transportation, and instrument separation be decreased if not fully eliminated because such errors slow down progress and adversely affect case outcome.
One significant area of inefficiency during instrumentation is the required time for changing rotary files from handpieces. The use of multiple cordless handpieces, each preloaded with the required file in a given system, and the exchange of these handpieces vs changing files in one handpiece generally expedites the process of moving up or down in file size during instrumentation. The author’s pilot time-motion study of instrumentation has shown that more time is wasted outside the root canal changing files in the handpiece than is used in the canal with each file cutting dentin and shaping canals. This is particularly true with rotary files that employ higher RPM settings where the intracanal-use time of each instrument is minimal. A triangular cross-section file that rotates at 600 RPM rotates 10 revolutions every second. This means that any given area of the canal is swept by a blade 30 times every second (three blades for a triangular cross-section rotating at 10 revolutions/second) Therefore, such files are very efficient and, in the author’s experience, the intracanal time necessary with them is very limited, generally a fraction of a second. To avoid wasting time changing files in the same handpiece it is more efficient to use multiple cordless handpieces preloaded with different files and exchange them to minimize the time wasted by changing files in the same handpiece (Figure 7). This holds true no matter what system is used.
During canal instrumentation, excessive removal of tooth structure from the canal is not necessary. The minimal amount of removal that results in successful cleaning and allows for adequate obturation is all that is logically required. It is true that this cannot be ascertained clinically; however, the coexistence and popularity of both 0.04 and 0.06 constant taper files is an indication that both systems work. The author prefers the use of 0.04 taper rotary instruments vs the larger 0.06 taper files because the 0.04 taper allows for the preparation of a larger apical diameter (where dentin removal is more important) vs more coronal removal of dentin as offered by the 0.06 taper file. Larger apical 0.06 tapered files remove apical dentin at the expense of coronal dentin; therefore, their use should be limited. Larger apical sizes should only be prepared with 0.04 taper files to avoid unnecessary coronal weakening of the root. Given the adequacy of taper for obturation with a 0.04 taper in ISO sizes 30 or 35 in many molars and the effectiveness of irrigation with these file tapers, higher tapers will not necessarily improve the success rate but will unnecessarily weaken radicular tooth structure, predisposing the root to fracture. Therefore, larger tapers and root weakening for the mere advantage of a clinical “look” is unconscionable in the absence of evidence that proves a clinical improvement in outcome.
Obturation
Although cleaning and shaping the root canal system is the most significant factor in the short-term success of the case, proper obturation prevents recontamination and failure of the case in the long run. Effective obturation helps prevent apical disease caused by remaining bacteria in the canal after the cleaning and shaping process or reinfection of the canal caused by coronal leakage. Therefore, it is important to understand that sealing the root canal ends at the interface of the bacterial environment of the mouth and the canal (ie, the coronal filling or crown margins), not at the orifice of the canals. Because continual exposure of an obturated canal to bacteria results in complete canal recontamination within a short period of time, any effort to reduce coronal leakage after root canal therapy can only help to improve the long-term success of the case. Many techniques, including but not limited to lateral and vertical condensation, continuous wave, carrier-based, resin-based, and/or sealer-based (epoxy or glass ionomer) techniques, have been devised to address the various challenges of root canal obturation.
Unfortunately, to date no prospective, long-term, longitudinal study has been published demonstrating the relative efficacy or clinical success rate of the above techniques. However, because it has been established that the most important determinants of success are thorough cleaning, shaping and obturation, and an excellent coronal seal, the relative efficacy of the above techniques may not be as clinically significant a determinant of success if the core principles of cleaning, shaping, and obturation are followed. Therefore, in the absence of efficacy-related data that would unequivocally demonstrate a higher success rate between various techniques, efficient obturation methods are advantageous over inefficient ones.
Endodontic practitioners should pay particular attention to effective cleaning and shaping of canals and fill with efficient techniques that achieve consistent, reproducible results that are safe for the patient and readily re-treatable in case of failure. Instrumentation systems that allow a matching size obturation cone are particularly efficient because they reduce the need for prolonged cone fitting and often reduce the need for multiple accessory cones. If a matching gutta-percha is used with the final size shaping instrument, the gutta-percha will be a close match for the prepared canal, reducing the necessary time for excessive manipulation and fitting of the master cone. For the best cone-fitting efficiency, operators should select obturation techniques that match their corresponding instrumentation technique. For many systems today, this allows for a systematic matching of a master cone to the preparation file, which improves the efficiency of moving from an instrumented canal into obtaining a matching-size master cone and paper point. Placing paper points in all canals and blowing air over their shaft allows a wicking action that helps dry canals rapidly. Because the canals are blocked with the paper point, the incidence of air emphysema is eliminated with this technique. During obturation, much like the other steps during the treatment process, it is very important to develop and implement systems of communication with the chairside assistant to help smooth the flow of fitted master cones and additional cones/sealer into each canal.
Discussion
Several other technologic improvements have emerged recently that have improved the efficiency and quality of care. The use of the surgical operating microscope (SOM) allows for better visualization, inspection, evaluation, and, therefore, localization of additional canals. It also helps to improve the outcome of endodontic therapy.8,9 Although these devices have a high learning curve and may slow down the procedure during the learning phase, they improve efficiency of care after their operation is mastered through better visualization of the chamber and facilitating the discovery of additional canals.
The use of digital radiography and office-management software improves the efficiency of care once the learning curve of implementing and mastering the technology has been realized by the practice. Any form of digital information-management software that allows for efficient data entry of essential information through user-friendly interfaces helps to improve efficiency. Such systems will invariably help streamline the quality of information processing and allow for more thorough record keeping, financial processing, and improved patient privacy compliance. All such investments in digital technology can potentially help to reduce the number of human resources necessary to run an office, thereby reducing cost, unreliability, and the chance of human error, while maintaining productivity and improving service. The paperless, digital office is the future of all dental offices that seek to improve their efficiency and productivity.
On the clinical front, integration of instruments through the use of integrated carts and systems helps to reduce clutter in the operatory and bring all the necessary tools within reach. This reduces the burden of valuable time being taken up by the clinical assistant setting up the operatory and helps to streamline the process by having all of the necessary technology within easy reach. System integration is a fundamental part of any efficient office that strives to keep a clean, professional look while providing excellent service.
Apex locators also have helped dramatically in increasing the efficiency of endodontic procedures by allowing a more predictable canal length determination than the traditional radiograph, which is often difficult to read and interpret and may require several angles to finally view the periapex. In the author’s opinion, using a combination of radiographs and apex locators is often the most predictable method of determining the final length.
Other areas, such as the decision to perform single- vs multiple-visit treatment, are also significant factors in the efficiency of endodontic treatment. Theoretically, all procedures that can achieve the axiom of effective cleaning, shaping, and obturation of the root canal within a single visit should be performed in a single visit. However, if patient root canals cannot be fully dried after instrumentation because of the presence of blood, pus, or other exudates, obturation in a single visit may not be desirable. Placement of intracanal calcium hydroxide medication in such cases of continued drainage is necessary. Taking shortcuts—such as obturating a canal that has not been effectively cleaned—in the hope of success is unethical. Outcome assessment should always be a priority compared to expeditious treatment.
In today’s busy dental practice, it is also important to remember that the procedure is performed most efficiently with the least number of interruptions. Performing concurrent procedures on multiple patients can decrease efficiency and potentially jeopardize quality. This can further affect the patient’s overall experience negatively because of excessive, prolonged opening and vanishing effective pulpal anesthesia. Hygiene checks, phone calls, and other interruptions can also decrease efficiency and should be minimized by scheduling endodontic procedures in such way that a single sitting with the patient should begin and end the procedure without interruptions.
As a result of recent technological advances and a thorough understanding of the canal anatomy, improved instrumentation and obturation techniques have dramatically improved the efficiency of the endodontic procedures dentists perform. When required, multiple endodontic cases can be performed today in one sitting with minimal trauma to the patient while achieving optimal results (Figure 8).
The technological, psychological, and communication systems dentists choose to perform treatment effectively result in the overall efficiency of the care rendered to patients. To explain how effective systems can help maintain higher efficiency, three hypothetical systems (A, B, and C) can be compared that have been implemented to achieve the same quality results. Their relative efficiency can be illustrated on a graph (Figure 9). It can generally be assumed that an increase in the mere speed of performing a task will decrease the quality of the task performed (A). More effective systems, however, can help maintain quality at higher speeds as they are more efficient (B and C). All systems fail eventually at the point of diminishing return (PDR) where any increase in speed will adversely affect quality. The more robust a system, however, the higher speeds can be achieved before PDR is reached, as demonstrated by system C.
Conclusion
In endodontics, much like other facets of practice, dentists must choose wisely and implement robust systems and techniques so that patients receive the care they seek both effectively and efficiently. It is important that the effectiveness of any system employed that decreases the efficiency of the dentist’s care by introducing additional steps into the procedure be firmly established before implementing it into clinical procedure. In the absence of such convincing qualitative evidence, any additional steps in care will only act to decrease efficiency for the sake of a perceived, psychological improvement in treatment. Wishful thinking should at all times be balanced against the real, scientifically proven, and clinically significant results.
Oftentimes, dentists implement systems and techniques that may rationally make sense, but there is no evidence of their improvement of the quality of the care rendered or whether they provide a clinically significant benefit. In the absence of any scientific evidence in the superior quality of any given new technique, dentists can only assess its value through its efficiency. If the method is as good as the old one but is more efficient, then it is an improvement and worth the investment. If the system claims to be a qualitatively superior method but is less efficient, then the burden of proof lies with the system to demonstrate scientifically whether the decrease in efficiency is worth the investment. Astute clinicians will put the needs of their patients for the effective, efficient, and humane care they seek before their own personal needs.
References
1. Schilder H. Filling root canals in three dimensions. Dent Clin North Am. 1967:723-744.
2. Buchanan LS. Into the fourth dimension: news from the front as the millennium approaches. Dent Today. 1998;17(2):56-63.
3. Nasseh AA. Considerations for ensuring complete anesthesia during endodontic care. Inside Dentistry. 2005;1(1):60-64.
4. Malamed S. Handbook of Local Anesthesia: Text with Malamed’s Local Anesthesia Administration DVD Package. 5th ed. St. Louis, Mo: Mosby; 2004.
5. Nielsen BA, Craig Baumgartner J. Comparison of the EndoVac system to needle irregation of root canals. J Endod. 2007;33(5):611-615.
6. Ahmad M, Pitt Ford TJ, Crum LA. Ultrasonic debridement of root canals: acoustic streaming and its possible role. J Endod. 1987;13(1):490-499.
7. Archer R, Reader A, Nist R, et al. An in vivo evaluation of the efficacy of ultrasound after step-back preparation in mandibular molars. J Endod. 1992;18(11):549-552.
8. Tsesis I, Rosen E, Schwartz-Arad D, et al. Retrospective evaluation of surgical endodontic treatment: traditional versus modern technique. J Endod. 2006;32(5):412-416.
9. Rubinstein RA, Kim S. Long-term follow-up of cases considered healed one year after apical microsurgery. J Endod. 2002;28(5):378-383.
About the Author
Ali Allen Nasseh, DDS, MMSC, PC
Clinical Instructor
Harvard School of Dental Medicine
Assistant Professor
Tufts University School of Dental Medicine
Private Practice
Boston, Massachusetts