You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Removal of sound tooth structure involves biologic compromise.1 When the mechanical requirements of a restoration align to provide greater respect for the biologic requirements of a restored tooth, there is a greater chance for long-term success for both the tooth and the restoration.
The long-term success of metal posterior restorations has been established.2-4 The minimal thickness required to achieve sufficient material strength allows conservative preparation design and, therefore, less risk of pulpal compromise. Though resistance and retention form are required in the preparation design for metal restorations, the mechanical requirements can typically be met with less tooth reduction than is required for metal-ceramic or all-ceramic cohesively retained restorations.
While metal restorations are an outstanding treatment option for posterior teeth, their use has been declining over the past decade relative to that of metal-ceramic and all-ceramic restorations. This trend is attributed to patients’ interest in tooth-colored restorations. All-ceramic restorations also benefit from technologies that automate aspects of their fabrication. Automation implies less reliance on the skill of the individual ceramist as well as greater homogeneity and lower probability of defects within the material itself. Additionally, all-ceramic, adhesively retained restorations have been shown to demonstrate superior optical properties over porcelain metal restorations.5-7
While the concept of using ceramic in posterior teeth dates back to the late 1800s, it was not considered practical until the advent of adhesive protocols.8,9 Presently, ceramic onlays warrant consideration as an effective means of restoring posterior teeth.10-15
Case Selection
Several factors must be considered when determining the appropriateness of posterior all-porcelain, adhesively retained restorations. While the patient’s desire for an esthetic restoration may be one consideration, it should not be the only consideration.1,2,13,16 Other parameters that should be considered involve functional forces, adhesive potential of the remaining tooth structure, ability to achieve adequate isolation, and inherent tooth color.17
The patient’s functional risk factors may be a contraindication to all-porcelain restorations. Patients with parafunctional activity have been shown to demonstrate forces as much as six times that of the nonbruxer.18 The forces that these patients are capable of generating far exceed the fracture strength of all-porcelain restorations. Another functional consideration is the position of the tooth within the arch; the more posterior the tooth within the arch, the higher the bite forces that the restoration will receive.19,20 For example, when there is a need for a full-coverage restoration of a second molar in a patient with large masseter muscles, cast gold still remains the most predictable solution.
Since the retention of the restoration is dependent on the bond strength which itself is closely related to the amount of remaining enamel available for bonding, it is recommended that there be equal to or greater than a 1-mm average ring of enamel available as a retentive substrate for the restoration. Certainly, the greater the amount of remaining enamel, the greater the adhesive potential of the tooth/ ceramic interface.21 For a posterior tooth with significant preoperative wear, 2 mm of additional occlusal reduction to provide adequate bulk for the restoration may result in insufficient enamel remaining for optimal retention. While the most optimal and least optimal clinical indications for adhesively retained restorations are apparent, many questions still remain regarding situations that fall in the middle. The precise clinical impact of varying degrees of available enamel versus dentin substrate, the long-term clinical effects of dentin bonding systems that exhibit significant in vitro shear bond strengths, and the influence of individual functional risks on the long-term prognosis of the final restorations are all questions that need further exploration.
The ability to achieve adequate isolation for an adhesive protocol must also be considered. Subgingival margins, areas exhibiting little to no remaining enamel around the circumference of the preparation, and situations that do not allow for proper isolation during the delivery phase are contraindications to the long-term success of adhesively retained restorations.
Posterior teeth that are particularly suited for adhesively retained restorations are teeth that fall within the esthetic zone, teeth that require cuspal protection but still maintain significant structural integrity in an axial dimension, and teeth with short clinical crowns. The advantages of adhesively retained restorations in these situations include improved esthetics, greater preservation of tooth structure, and less risk of biologic width violation.
Preparation Design for All-Porcelain Onlay Restorations
The guidelines for preparation design of all-porcelain posterior restorations center on providing adequate bulk of material to affect appropriate resistance to fracture, as well as providing smooth transitions that avoid concentrating stresses within the porcelain during occlusal load.
Occlusal Requirements
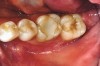
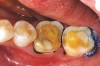
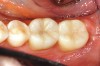
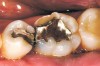
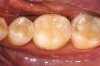
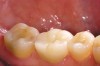
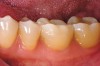
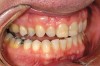
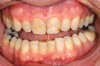
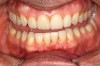
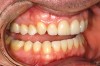
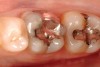
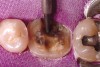
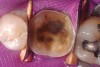
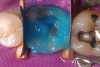
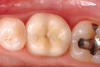
While in vitro studies do not definitively demonstrate a correlation between fracture resistance and cuspal coverage, cuspal coverage is still considered important in instances where the remaining tooth structure is less than one third to one half of the intercuspal distance.22,23 Other factors that support cuspal coverage of posterior teeth are the position of the tooth within the arch, with molars subject to greater bite forces and, therefore, exhibiting a greater need for cuspal coverage.24,25 Cracked teeth also warrant cuspal coverage (Figure 1A through Figure 1C).26,27
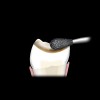
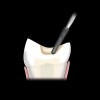
All-porcelain restorations in posterior teeth require a minimum of 2 mm of occlusal clearance in the stress-bearing areas to provide adequate strength for the materials (Figure 2).28 While varying degrees of strength exist between feldspathic, leucite-reinforced, and lithium disilicate restorations, all have been shown to be successful with adequate occlusal thickness and proper management of occlusal forces.29 Higher strength porcelains, such as lithium disilicate, present opportunities for one-phase fabrication and may offer adequate strength at thicknesses less than 2 mm.30 More studies are needed to verify this hypothesis.
Additive techniques, such as that required when increasing the vertical dimension of occlusion as part of a comprehensive treatment solution, are particularly suited to adhesively retained restorations. The minimal degree of tooth preparation that is required in these instances leaves a larger enamel ring and higher bond strengths at the tooth/adhesive interface.21
The tooth itself is critical in supporting the restoration. When there has been a loss of tooth structure in a pulpal direction beyond that which is considered sufficient to meet the mechanical requirements of the restoration, the tooth must be reinforced and the preparation shaped to ideal contour.31 Resin hybrid core materials provide strength as well as etchability and are well-suited to this purpose.
Interproximal Axial Requirements
The axial requirements of preparation design are dependent on the individual requirements of the tooth in need of restoration. All-porcelain restorations make use of adhesive principles for retention and their preparations do not require extension to create resistance and retention form. However, the biomechanical or esthetic requirements of a tooth may demand that the preparation extend beyond the degree required to satisfy the occlusal requirements of the restoration.
Many, though not all, restorations which need cuspal protection also require extension to the interproximal contact zone. Indications to extend the preparation cervically in the interproximal zone include fracture, crack lines, existing restorations, caries, or the need to alter proximal shape. The degree of cervical extension is directly related to the biomechanical compromise of the tooth. If the interproximal margin extends cervically to such a degree that no enamel remains, the practitioner must reevaluate the appropriateness of an adhesively retained restoration. Other potential contraindications to adhesively retained restorations involve situations that prevent adequate separation or isolation during cementation protocols. Challenges can also arise from the geometric relationship of one tooth to another within the arch form or the relationship of the interproximal tissue to the cervical margin. If potential compromises arise, the clinician must evaluate the situation and combine scientific knowledge with sound clinical judgment to determine the best long-term solution for the patient.
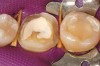
Unlike traditional preparations that involve cuspal protection, adhesively retained restorations need not break the interproximal contact zone unless there is a biomechanical indication for doing so. Interproximal finish lines that fall within the contact zone can be managed in the laboratory as well as clinically. However, if there is no need to break contact with the adjacent teeth, the preparation will require an orientation strategy to aid in the fabrication and seating of the restoration. A slight depression, mirroring the shape of a Class I cavity preparation and prepared within the central fossa of the tooth, will provide a keyway for proper orientation and seating of the restoration at the time of insertion. Transitions from platforms created by the occlusal reduction and interproximal shoulders should follow a smooth slope that avoids steep angles to the long axis of the tooth (Figure 3).
Facial or Lingual Axial Requirements
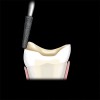
Facial or lingual axial reduction may be used to accommodate previous restorations, loss of tooth structure resulting from fracture, or esthetic considerations. In areas where a loss of tooth structure in a facial or lingual dimension dictates that the restoration extend more cervically than the extent provided by the occlusal reduction, a well-defined, 1-mm shoulder that is 90° to the cavosurface should be established to provide adequate bulk of porcelain (Figure 4).32 The internal aspects of the shoulder should be rounded to prevent stress concentration.33
A chamfer finish line provides for the most esthetic blending of porcelain and tooth structure and is commonly added as the final detail to the facial aspect of the preparation (Figure 5). The occluso-cervical position of the facial chamfer is largely dependent on the need to alter tooth color. If the inherent color of the tooth is acceptable, a 2-mm chamfer is all that is required to blend the porcelain/tooth interface (Figure 6A through Figure 6E). A need to effect a color change dictates a facial finish line carried to the free gingival margin.
Additional indications for carrying the facial aspect of the preparation to the free gingival margin include the intent to alter the buccal contour of the tooth with the final restoration or the desire to eliminate the need for pre-existing Class V restorations (Figure 7A through Figure 7D). Ideally, the depth of the chamfer should be maintained within enamel to maximize bond strengths.34,35 Knife-edge margins should be avoided as they are not well-suited to all-porcelain restorations. To increase marginal fit, it is recommended that all sharp edges are eliminated and finishing burs are used to minimize surface roughness (Figure 8).36 Transitions from platforms created by the occlusal reduction and axial shoulders should likewise follow a smooth slope that avoids steep angles to the long axis of the tooth. To increase resistance to fracture under occlusal load, all transitions should be smooth and gradual.37 Sharp angles in the preparation are to be avoided, as they generate areas of high stress within porcelain. Smooth-butt margins, 90° to the cavosurface, are considered ideal.
Provisionalization
Without the advantages of resistance and retention form, fabrication and retention of provisional restorations for restorations that will ultimately be adhesively retained presents special challenges. In addition, the color of the luting agent can have a significant impact on the esthetics of the provisional restorations because of the typically thin nature of these restorations on the facial aspects of the teeth.
A straightforward approach to fabricating provisional restorations for posterior adhesively retained restorations involves the use of a silicone matrix developed from the diagnostic mock-up or the pretreatment tooth contours in instances where there are no plans for significant alterations of anatomy or contours.38,39 In an isolated field, the prepared teeth are micro-abraded, rinsed, and dried. The preparations are coated with unfilled resin. The silicone matrix, filled with a self-curing bisacryl provisional material, is seated intraorally over the prepared teeth. When the bisacryl material reaches full set, the matrix is removed. The provisional restorations, retained on the preparations, are trimmed of excess material intraorally, with hand instruments and fine diamonds.
Alternately, an extraoral trimming of the provisionals can be accomplished by seating the silicone matrix filled with bisacryl material over slightly moist preparations that have not been micro-abraded. In this case, the provisional restorations will not adhere to the preparations and will be removed along with the silicone matrix. The provisional restorations can then be trimmed, shaped, and polished before cementation. Fine diamonds, diamond-impregnated discs, and acrylic burs that are specifically designed for trimming bisacryl materials are helpful in contouring the restorations. A water-soluble lubricant is placed on the external surfaces to aid in removal of excess cement after cementation. Translucent resin cements used without adhesive protocols are well-suited for luting provisional restorations that have little mechanical retention. Without etching or priming of the prepared tooth surfaces, the resin cement functions as a weak cohesive link between the tooth and the provisional restoration. It is recommended that adjacent units of the provisional restoration remain fused to one another as an additional retentive aid.
Delivery and Cementation
In an isolated field, the temporary restorations are removed and the preparations thoroughly cleaned using a low-pressure, particle-abrasion cleansing protocol (Figure 9A and Figure 9B).40 The restorations are carefully tried on the prepared teeth one at a time. Proximal contacts are adjusted as needed so that each restoration seats fully to place. Accurate fit and marginal integrity are confirmed. Adjoining restorations are tried in en masse to confirm appropriate proximal contacts. Once the accuracy of the restorations themselves and the proximal contacts have been confirmed, the restorations are filled with a translucent try-in paste to provide an accurate esthetic preview of the final result. The occlusion is not evaluated until after the restorations have been luted to the preparations.
The quality of the adhesive bond has an effect on retention, microleakage, and, ultimately, the structural integrity of the restoration itself.41,42 Care must be taken to meticulously execute accepted adhesive protocols in the surface management of the tooth as well as the intaglio surface of the restoration.43,44
Ceramic Interface Management
Etching the porcelain surface is best suited to the laboratory. Manufacturer recommendations regarding appropriate etching times with hydrofluoric acid should be followed closely. Times vary between 180, 60, and 20 seconds for feldspathic, leucite-reinforced, and lithium disilicate ceramics, respectively. A lack of adherence to recommended times (either inadequate or excessive) can result in reduced bond strengths at the ceramic/ resin interface.45-50
The try-in phase exposes the etched restorations to contamination; therefore, it is recommended that they be cleaned with a 30% to 40% phosphoric acid for 60 seconds, rinsed, and dried.51 A silane coupling agent, which positively affects the resin bond to feldspathic, leucite-reinforced, and lithium disilicate ceramics, is applied to the etched and decontaminated ceramic surfaces for 60 seconds and air-dried thoroughly with a moisture-free and oil-free air source.47,52-56
Tooth Surface Management
If the teeth have not been already isolated and cleaned, rubber dam isolation and air-abrasion micromechanical debridement are completed at this time. Hemostasis must be confirmed and areas of concern addressed. Achieving a clean, dry field in which to cement all-porcelain, adhesively retained restorations is essential to prevent insufficient bond strengths and microleakage.33 The teeth, one at a time, anterior to posterior, are wedged to slightly separate the contact points and thus alleviate any resistance to full seating of the restorations at the cementation phase (Figure 9C). If need be, the occluso-cervical dimension of the wedges should be trimmed to prevent any potential interference to full seating of the restorations.
A 30% to 40% phosphoric acid is agitated on the preparation and slightly beyond the prepared margins for 15 seconds (Figure 9D). The tooth is rinsed for 5 seconds. Excess moisture is removed, yet the prepared surfaces are allowed to stay slightly moist. Desiccation of the tooth should be distinctly avoided. A fourth- or fifth-generation adhesive protocol can be used per manufacturer instructions (Figure 9E). The restoration, appropriately lined with either dual-cure or light-cure resin cement, is seated to place. Excess cement is removed and the restoration light-cured (Figure 9F).
Various parameters affect the decision to use light-cure or dual-cure resin cements. For highly translucent ceramics, a light-cure resin can be used to lute restorations that are 2 mm or less in thickness. For restorations greater than 2 mm in thickness, a dual-cure resin is recom-mended.57-59 There are indications that dual-cure cements should be used as the opacity of the restoration increases. Also, the density of lithium disilicate restorations call for greater curing times and a move toward dual-cure cements.60 Clinicians should be mindful that some dual-cure adhesive systems are less effective in situations where the cement cannot be light-cured.61
Following appropriate curing times, excess resin cement is removed from all surfaces with hand instrumentation. The occlusion is checked and adjusted as required. The adjusted areas are polished with a series of diamond-impregnated polishing points and finalized with a diamond paste on a flexible brush wheel (Figure 9G).
Conclusion
All-porcelain, adhesively retained restorations are a viable option for posterior teeth. The advantages of such restorations center on the ability to provide cuspal coverage and improved esthetics with minimal or no axial reduction of the restored teeth.
Proper case selection is of utmost importance. Patients must be informed of the limits and liabilities of the various available material choices. While no indirect material has the proven long-term success of metal restorations, all-porcelain, adhesively retained restorations show promise when used appropriately. Proper case selection, execution of a preparation design which serves to minimize stress within the final restoration, management of occlusal forces, and careful attention to adhesive protocols all serve to increase long-term prognosis and success.
Key Design Elements
- Preparation should allow for a minimum of 2 mm of occlusal clearance
- Inherent biomechanical compromises dictate the extent of axial preparation
- Preparation does not need to break the interproximal contact zone
- Facial chamfers facilitate optical blending of the tooth/ceramic interface
- Circumferential border of enamel, averaging 1 mm width
- Occlusal keyway for preparations without axial walls
References
1. Jackson CR, Skidmore AE, Rice RT. Pulpal evaluation of teeth restored with fixed prostheses. J Prosthet Dent. 1992;67(3):323-325.
2. Donovan T, Simonsen RJ, Guertin G, Tucker RV. Retrospective clinical evaluation of 1,314 cast gold restoration in service from 1 to 52 years. J Esthet Restor Dent. 2004; 16(3):194-204.
3. Studer SP, Wettstein F, Lehner C, et al. Long term survival estimates of cast gold inlays and onlays with their analysis of failures. J Oral Rehabil. 2000;27(6):461-472.
4. Stoll R, Sieweke M, Pieper K, et al. Longevity of cast gold inlays and partial crowns—a retrospective study at a dental school clinic. Clin Oral Investig. 1999;3(2): 100-104.
5. Raptis NV, Michalakis KX, Hirayama H. Optical behavior of current ceramic systems. Int J Perio Rest Dent. 2006;26(1): 31-41.
6. Holand W, Schweiger M, Watzke R, et al. Ceramics as biomaterials for dental restoration. Expert Rev Med Devices. 2008; 5(6):729-745.
7. Donovan TE. Factors essential for successful all-ceramic restorations. J Am Dent Assoc. 2008;139:14S-18S.
8. Calamia JR, Simonsen RJ. Effect of coupling agents of bond strength of etched porcelain. J Dent Res. 1984;63:179 (Abstract no 79).
9. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2): 399-417.
10. Frankenberger R, Taschner M, Garcia-Godoy F, et al. Leucite-reinforced glass ceramic inlays and onlays after 12 years. J Adhes Dent. 2008;10(5):393-398.
11. Federlin M, Wagner J, Manner T, et al. Three-year clinical performance of cast gold vs ceramic partial crowns. Clin Oral Investig. 2007;11(4):345-352.
12. Magne P, Belser UC. Porcelain versus composite inlays/onlays: Effects of mechanical loads on stress distribution, adhesion and crown flexure. Int J Perio Rest Dent. 2003; 23:543-555.
13. Felden A, Schmalz G, Hiller KA. Retrospective clinical study and survival analysis on partial ceramic crowns: results up to 7 years. Clin Oral Investig. 2000;4(4): 199-205.
14. Ritter AV, Baratieri LN. Ceramic restorations for posterior teeth; guidelines for the clinician. J Esthet Dent. 1999;11(2):72-86.
15. Naeselius K, Arnelund CF, Molin MK. Clinical evaluation of all-ceramic onlays: A 4-year retrospective study. Int J Prosthodont. 2008; 21(1):40-44.
16. Hickel R, Manhart J. Longevity of restorations in posterior teeth and reasons for failure. J Adhes Dent. 2001;3(1):45-64.
17. Trushkowsky RD, Burgess JO. Complex single-tooth restorations. Dent Clin North Am. 2002;46(2):341-365.
18. Gibbs CH, Mahan PE, Mauderli A, et al. J Prosthet Dent. 2006;56:226-229.
19. Mansour RM, Reynik JF. In vivo occlusal forces and moments: I. Forces measured in terminal hinge position and associated moments. J Dent Res. 1975;54(1):114-120.
20. Otto T, Schneider D. Long-term clinical results of chairside CEREC CAD/CAM inlays and onlays: A case series. Int J Prosthodont. 2008;21(1):53-59.
21. Dumfahrt H, Schaffer H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service: Part II- clinical results. Int J Prosthodont. 2000;13:9-18.
22. Soares CJ, Martins LRM, Foneseca RB, et al. Influence of cavity preparation design on fracture resistance of posterior Leucite-reinforced ceramic restorations. J Prosthet Dent. 2006;95(6):421-429.
23. Krifka S, Stangl M, Wiesbauer S, et al. Influence of different cusp coverage methods for the extension of ceramic inlays on marginal integrity and enamel crack formation in vitro. Clin Oral Investig. 2009; in press.
24. Dejak B, Mlotkowski A. Three-dimensional finite element analysis of strength and adhesion of composite resin versus ceramic inlays in molars. J Prosthet Dent. 2008; 99(2):131-140.
25. Fennis WMM, Kuijs RH, Kreulen CM, et al. A survey of cusp fractures in a population of general dental practices. Int J Prosthodont. 2002;15:559-563.
26. Geurtsen W, Schwarze T, Gunay H. Diagnosis, therapy, and prevention of the cracked tooth syndrome. Quintessence Int. 2003; 34:409-417.
27. Signore A, Benedicenti S, Covani U, Giambattista R. A 4- to 6-year retrospective clinical study of cracked teeth restored with bonded indirect resin composite onlays. Int J Prosthodont. 2007;20(6):609-616.
28. Federlin M, Krifka S, Herpich M, et al. Partial ceramic crowns: Influence of ceramic thickness, preparation design and luting material on fracture resistance and marginal integrity in vitro. Oper Dent. 2007;32(3): 251-260.
29. Conrad HJ, Seong WJ, Pesun IJ. Current ceramic materials and systems with clinical recommendations: a systematic review. J Prosthet Dent. 2007;98(5):389-404.
30. Rekow D, Zhang Y, Thompson V. Can material properties predict survival of all-ceramic posterior crowns? Compend Contin Educ Dent. 2007;28:362-368.
31. Banditmahakun S, Kuphausuk W, Kanchanavasita W, Kuphasuk C. The effect of base materials with different elastic moduli on the fracture loads of machinable ceramic inlays. Oper Dent. 2006;31(2): 180-187.
32. El-Ebrashi MK, Craig RG, Peyton FA. Experimental stress analysis of dental restorations. Part III. The concept of the geometry of proximal margins. J Prosthet Dent. 1969; 22:333.
33. Derand T. Analysis of stresses in the porcelain crowns. Odontol Rev. 1974;25:(suppl 27).
34. Tjan AH, Dunn JR, Sanderson IR. Microleakage patterns of porcelain and castable ceramic laminate veneers. J Prosthet Dent. 1989;61:276-282.
35. Troedson M, Derand T. Effect of margin design, cement polymerization, and angle of loading on stress in porcelain veneers. J Prosthet Dent. 1999;82:518-525.
36. Ayad MF. Effects of tooth preparation burs and luting cement types on the marginal fit of extracoronal restorations. J Prosthodont. 2009;18(2):145-151.
37. Derand T. The importance of an even shoulder preparation in porcelain crowns. Odontol Rev. 1972;23:305.
38. Lee E, Jun S. Achieving aesthetic excellence through an outcome-based restorative treatment rationale. Pract Periodont Aesthet Dent. 2000;12(7):641-648.
39. Magne P, Magne M, Belser U. The diagnostic template: A key element to the comprehensive esthetic treatment concept. Int J Periodontics Restorative Dent. 1996;16: 560-569.
40. Chaiyabutr Y, Kois JC. The effects of tooth preparation cleansing protocols on the bond strength of self-adhesive resin luting cement to contaminated dentin. Oper Dent. 2008;33(5):556-563.
41. Della Bona A, Anusavice KJ, Mecholsky JJ Jr. Failure analysis of resin composite bonded to ceramic. Dent Mater. 2003; 19(8):693-699.
42. Della Bona A, Anusavice KJ, Shen C. Microtensile strength of composite bonded to hot-pressed ceramic. J Adhes Dent. 2000; 2(4):305-313.
43. Blatz, MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent. 2003;89(4):381-387.
44. Alex G. Preparing porcelain surfaces for optimal bonding. Compend Contin Educ Dent. 2008;29(6):324-335.
45. Ayad MF, Fahmy NZ, Rosenstiel SF. Effect of surface treatment of roughness and bond strength of a heat-pressed ceramic. J Prosthet Dent. 2008;99(2):123-130.
46. Kamada K, Yoshida K, Taira Y, et al. Shear bond strength of four resin bonding systems to two silica-based machinable ceramic materials. Dent Mater J. 2006;25(3): 621-625.
47. Estafan D, Dussetschleger F, Estafan A, Jia W. Effect of prebonding procedures on shear bond strength of resin composite to pressable ceramic. Gen Dent. 2000;48(4): 412-416.
48. Chen JH, Matsumura H, Atsuta M. Effect of different etching periods on the bond strength of a composite resin to a machinable porcelain. J Dent. 1998;26(1):53-58.
49. Kupiec A, Wuertz KM, Barkmeier WW, Wilwerding TM. Evaluation of porcelain surface treatments and agents for composite-to-porcelain repair. J Prosthet Dent. 1996; 76(2):199-124.
50. Sorensen JA, Engelman JF, Torres TJ, Avera SP. Shear bond strength of composite resin to porcelain. Int J Prosthodont. 1991;4(1): 17-23.
51. Aboush YE. Removing saliva contamination from porcelain veneers before bonding. J Prosthet Dent. 1998;80(6):649-653.
52. Pisani-Proenca J, Erhardt MCG, Valandro LF, et al. Influence of ceramic surface conditioning and resin cements on microtensile bond strength to a glass ceramic. J Prosthet Dent. 2006;96(6):412-417.
53. Yoshida K, Meng X, Kamada K, Atsuta M. Influence of surface characteristics of four silica-based machinable ceramics on flexural strength and bond strength of a dual-curing resin luting agent. J Adhes Dent. 2007;9(4):407-413.
54. Yoshida K, Kamada K, Atsuta M. Effects of two silane coupling agents, a bonding agent, and thermal cycling on the bond strength of a CAD/CAM composite material cemented with two resin luting agents. J Prosthet Dent. 2001;85(2):184-189.
55. Barghi N. To silanate or not to silanate: making a clinical decision. Compend Contin Educ Dent. 2000;21(8):659-662.
56. Chen JH, Matsumura H, Atsuta M. Effect of etchant, etching period, and silane priming on bond strength to porcelain of composite resin. Oper Dent. 1998;23(5):250-257.
57. Pazin MC, Moraes RR, Goncalves LS, et al. Effects of ceramic thickness and curing unit on light transmission through leucite-reinforced material and polymerization of dual-cured luting agent. J Oral Sci. 2008; 40(2):131-136.
58. Koch A, Kroeger M, Hartung M, et al. Influence of ceramic translucency on curing efficacy of different light-curing units. J Adhes Dent. 2007;9(5):449-462.
59. Kamada K, Yoshida K, Atsuta M. Early bond strength and durability of bond between a ceramic material and chemically-cured or dual-cured resin luting agent. Am J Dent. 2001;14(2):85-88.
60. Ilie N, Hickel R. Correlation between ceramics translucency and polymerization efficiency through ceramics. Dent Mater. 2008; 24(7):908-914.
61. Asmussen E, Peutzfeldt A. Bonding of dual-curing resin cements to dentin. J Adhes Dent. 2006;8(5):299-304.
About the Authors
Elizabeth M. Bakeman, DDS
Private Practice
Grand Rapids, Michigan
Clinical Instructor,
Kois Center for Advanced Dental Education
Seattle, Washington
John C. Kois, DMD, MSD
Director
Kois Center for Advanced Dental Education
Seattle, Washington
Private Practice
Seattle/Tacoma, Washington
Affiliate Professor
University of Washington
Seattle, Washington