You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Before any treatment can occur, all patients should be evaluated for overall oral health during the initial examination regardless of the number of teeth present. If the patient is a candidate for implant therapy, a systematic series of steps should be taken to assess the possible treatment options available to the patient. The stress treatment theorem for implant dentistry as described by Misch1 is a biomechanical model used to assess the patient for implant reconstruction. The evaluation criteria are listed below in descending order of importance:
- Prosthesis design
- Patient force factors
- Bone density in implant sites
- Key implant positions and number
- Implant size
- Available bone
- Implant design
By starting with prosthesis design, the prosthetic options and available space must be addressed first. The idea that implant dentistry is a prosthetically driven discipline, not a surgically driven one, is accepted in dentistry without argument. Yet more often than not, the restorative dentist either does not examine the available space or expects the specialist placing the implant to position the implant in the right place. Because this is not a predictable model under which to operate, it is certainly not in the best interest of the patient. These parameters must be addressed first.
The crown height space is a parameter that is often overlooked until after the implants have integrated and the patient is ready for restoration. If enough space is available, traditional implant prosthetics are completed in a very satisfactory way. However, if there is too little space, then the outcome is generally unacceptable for both the patient and the doctor. The patient may be displeased because he or she may have to undergo additional procedures or have to be fitted with a different type of prosthesis than originally planned. Both of these scenarios generally require more chair time and a greater cost. In this article, the vertical and horizontal parameters that must be followed to avoid these potential complications will be addressed as they pertain to prosthesis design.
Crown Height Space: The Key Vertical Parameter
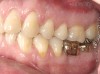
Crown height space is the distance from the occlusal plane to the crest of the alveolar ridge2 (Figure 1). The available crown height space will influence the type of prosthesis, material choices, and surgical technique that will be used. This important preoperative parameter will be discussed as it pertains to various types of restorations.
Fixed Restorations
The cement-retained implant prosthesis requires a minimum of 8 mm of crown height space.
The ideal space, however, for a cement-retained prosthesis is 9 mm to 10 mm in the posterior and 10 mm to 12 mm in a maxillary central. The crown height space for a cement-retained prosthesis has three main regions: the soft tissue, abutment, and occlusal material. The ideal vertical dimensions of each region are: 3 mm for the soft tissue;3 5 mm for the abutment height;4 and 2 mm for the occlusal metal or porcelain (Figure 2).
Taking a more detailed look at these distances, the soft tissue, also known as the peri-implant biological width, is comprised of three sections. The first is the sulcular epithelium, which has no bond to the abutment. The second, the functional epithelium, has a hemidesmosome attachment with the titanium surfaces. Together, these components comprise 2 mm of the peri-implant’s biological width. The supracrestal connective tissue, the third region of soft tissue, has a minimum vertical dimension of approximately 1 mm and is mostly collagen fibers oriented in a parallel or circumferential direction.5,6 The crown margin should be at least 2 mm above the crestal bone to allow the connective tissue zone of attachment.7
The second component of the crown height space, the abutment height, should be 5 mm in the most ideal situations. The minimum preparation height in the posterior regions of the mouth is 4 mm. While a screw-retained restoration can screw directly onto the implant body and require an even smaller crown height space, complications can arise with this type of prosthesis. A passive fit is generally harder to obtain, it exhibits weaker porcelain strength at the screw–hole interface, and presents greater incidence of screw loosening.8,9 There is also the increased laboratory fee of one and a half to twice that of a cement-retained prosthesis. While this is not a clinical complication, it, along with the former, are all complications that can possibly be avoided by looking at the crown height space preoperatively.
The third component of crown height space in a fixed restoration is the occlusal surface distance. If there is a limited amount of crown height space available, the use of a metal occlusal restoration may be required, but it may be the least esthetic option. Also, if the patient has high occlusal forces, the metal occlusal restoration may be the best option, but the use of metal should be discussed with the patient preoperatively, not pre-restoratively or, even worse, at the delivery appointment. If at least 2 mm of occlusal clearance is planned, then, just like natural teeth, there will be enough room for occlusal porcelain to be used.
Fixed Restorations: Large Segment/Full Arch
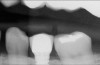
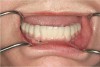
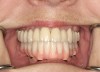
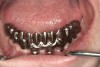
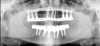
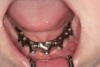
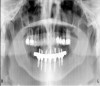
For large-segment/full-arch fixed prostheses, the critical distance is 15 mm. If the distance from the implant platform to the occlusal table is less than 15 mm, then the prosthetic material indicated is porcelain-fused-to-metal (PFM) (Figure 3). If the distance is greater than 15 mm, then a hybrid prosthesis should be used (Figure 4).
The 15-mm measurement is important because of the physical properties of the restorative materials. Acrylic requires bulk for strength. If there is less than 15 mm of distance from the implant platform to the occlusal table, there will not be sufficient space to achieve the bulk of acrylic necessary to provide strength for the prosthesis. The unfortunate result will be continual repair of fractures for the life of the prosthesis.
Likewise, PFM restorations have difficulties when too much space is available. At dimensions greater than 15 mm from the implant platform to the occlusal table, the control of surface porosity across the metal substructure becomes difficult because of variations in cooling and heating rates across the metal,10 which in turn makes it difficult to bake porcelain to the metal substructure. The result is the high possibility of future unwanted complications of porcelain fracture.11
There is also a considerable difference in the laboratory costs for these types of prostheses. A PFM restoration requires more metal to achieve a uniform 2-mm thickness and is more technique-sensitive (Figure 5 and Figure 6). A hybrid prosthesis requires less metal and uses acrylic and denture teeth for the remaining restoration (Figure 7 and Figure 8). Understanding the impact that the 15-mm height has on which type of restoration is required gives the dentist the ability to quote a more accurate fee to the patient.
Removable Prostheses
An implant-retained removable prosthesis has two options in terms of connecting the implant to the prosthesis. One option is a bar-retained prosthesis that needs at least 15 mm to 17 mm of crown height space (variance depends on the type of attachment). It is comprised of the following: 3 mm, bone to soft tissue; 1 mm, soft tissue to bar; 3 mm to 5 mm, bar plus attachment. The remaining vertical distance is made up of the denture teeth and supporting acrylic. This is a height of > 8 mm from the bar/attachment to the incisal edge (Figure 9).
The second option is a low-profile independent attachment which has a lower vertical space requirement. This space is measured from the alveolar crest to the inner aspect of the lingual denture base, and the measurement is a minimum of 7 mm.12 The current lowest vertical height of an attachment (abutment plus male) is 3.17 mm on an externally hexed implant, and 2.5 mm on a non-hexed implant.
Again, it is important to remember that acrylic restorations obtain their strength from the bulk of the material. If the preoperative option discussed with the patient is a bar overdenture and conversion to an independent attachment prosthesis is required later, the patient may be displeased, depending on his or her expectations. This is a situation that can be avoided by choosing the appropriate prosthesis based on the crown height space available.
Excessive Crown Height Space
Excessive crown height space can be problematic as well. Excessive crown height space acts as a vertical cantilever. The greater the crown height space, the greater the moment of force under lateral load. For every 1 mm in crown height increase, the force increase may be 20%. Therefore, a crown height increase of 10 mm to 20 mm may increase stress 200%.13 To prevent this, there are different surgical approaches to help diminish available crown height space, such as block onlay grafts, particulate bone grafts with mesh titanium or barrier membranes, interpositional bone grafts, and distraction osteogenesis.14-16
Diminished Crown Height Space
Diminished crown height space has several different solutions which depend on the patient’s anatomical limitations as well as his or her perceived needs. If the problem is the opposing arch, the solution may be fixed prosthodontics to level the occlusal plane (Figure 10A through Figure 10D). It may be intrusion of teeth with orthodontics or some combination of the two. If there is too little crown height space and the patient is edentulous, the solution may be to increase the vertical dimension of occlusion (VDO) with a removable prosthesis.17 If the patient has a partial dentition, it may involve traditional fixed prosthodontics to alter the VDO.18 The patient may need a surgical approach, such as an osteoplasty, before implant placement (Figure 11A and Figure 11B). However, without an initial diagnosis, there is no way of formulating a solution to an unknown problem.
Horzontal Components of Implant Placement
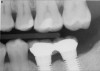
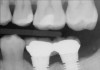
The horizontal aspect of implant spacing is critical to avoid bone loss on adjacent teeth or implants. Single-tooth implants should be placed 1.5 mm to 2 mm from the adjacent teeth,19,20 and implants should have at least 3 mm of space between them21 (Figure 12). By keeping a minimum 1.5-mm distance from the adjacent tooth and a minimum distance of 3 mm between adjacent implants, angular defects resulting from crestal bone remodeling can be kept from becoming horizontal defects19-22 (Figure 13). This distance allows the bone on the adjacent tooth to stay at its current level. Conversely, if bone loss on the adjacent tooth or implant occurs, the bone loss will not affect the adjacent tooth or implant. This is especially critical in the anterior regions of the mouth where papilla height is more important for an esthetic result.23-27
Anterior-Posterior Spread
As a general rule, when five implants are placed in the anterior mandible between the foramen, the cantilever should not exceed 2.5 times the anterior-posterior spread, with all other force factors being low.28 The anterior-posterior distance is obtained by connecting a line drawn from the distal aspect of the most posterior implants and a parallel line drawn through the center of the most anterior implant (Figure 14). The greater the anterior-posterior distance, the more favorable the situation for the posterior cantilever.29-30 There are two anatomical factors that will affect the amount of anterior-posterior spread possible: the patient’s existing arch form and the arch form of the replacement teeth. There are three types of arch forms: ovoid, tapering, and square. A square arch form provides the shortest anterior-posterior spread because all of the implants are basically in a straight line. Conversely, the tapering arch will result in the largest anterior-posterior spread, and the ovoid will result in something in between. By evaluating the arch form, the clinician will have an idea of the potential anterior-posterior spread and the amount of cantilever possible to support the prosthesis. Patient force factors will ultimately determine the amount of cantilever to be used for the definitive prosthesis.
Conclusion
This is not an exhaustive list of all the numbers a clinician needs to know to perform implant dentistry, but it comprises what the authors feel are the most preoperatively overlooked numbers. All cases are evaluated for bone width, bone height, and implant diameter preoperatively, but these other numbers are too often only looked at pre-restoratively, after the implants have integrated. As discussed, this is sometimes too late. Usually, the problems can be overcome with additional procedures, but the costs to the patient and the clinician are both monetary and emotional. Dentistry has enough complications even when things are done correctly. By paying attention to these parameters for implant dentistry preoperatively, we can minimize the complications.
References
1. Misch CE. Stress theorem for implant dentistry. In: Contemporary Implant Dentistry. 3rd ed. St. Louis MO: Mosby. 2008;68-88.
2. Jalbout Z, Tabourian G. Glossary of Implant Dentistry II. 2008. International Congress of Oral Implantologists, Upper Montclair, NJ.
3. Berglundh T, Lindhe J. Dimension of the peri-implant mucosa. Biologic width revisited. J Clin Periodontol. 1996;23:971-973.
4. Misch CE. Dental Implant Prosthetics. St. Louis, Mo: Mosby. 2005;430-430.
5. Naylor WP. Introduction to Metal Ceramic Technology. Chicago: Quintessence. 2009; Chapter 4.
6. Berglundh T, Lindhe J, Ericsson I, et al. The soft tissue barrier at implants and teeth. Clin Oral Implants Res. 1991;2:81-90.
7. Misch CE. Dental Implant Prosthetics. St. Louis, Mo: Mosby 2005;166.
8. Jemt T, Laney WR, Harris D, et al. Osseointegrated implants for single tooth replacement: a 1-year report from a multicenter prospective study. Int J Oral Maxillofac Implants. 1991;6:29-36.
9. Kline R, Hoar JE, Beck GH. A prospective multicenter clinical investigation of bone quality based dental implant systems. Implant Dent. 2002;11:224-234.
10. Bidger DV, Nicholls JI. Distortion of ceramometal fixed partial dentures during the firing cycle. J Prosthet Dent. 1981;45:507-514.
11. Bertolotti RL, Moffa JP. Creep rate of porcelain bonding alloys as a function of temperature. J Dent Res. 1980;59:2061-2065.
12. Carpentieri JR, Tarnow DP. The mandibular two-implant overdenture. Mahwah, NJ: Montage Media Corporation. 2007;26.
13. Misch CE, Bidez MW. Implant protected occlusion, a biomechanical rationale. Compend Contin Educ Dent. 1994;15:1330-1342.
14. Misch CE, Goodacre CL, Finley JM, et al. Consensus Conference Panel Report: crown-height space guidelines for implant dentistry. Part 1. Implant Dent. 2005;14:312-318.
15. Misch CE, Goodacre CL, Finley JM, et al. Consensus Conference Panel Report: crown-height space guidelines for implant dentistry. Part 2. Implant Dent. 2006;15:113-121.
16. Jensen OT, Cockrell R, Kuheke L, et al. Anterior maxillary alveolar distraction osteogenesis: a prospective 5-year clinical study. Int J Oral Maxillofac Implants. 2002;17:507-516.
17. Palla S. Occlusal Considerations in Complete Dentures. Science and Practice of Occlusion. McNeil C, ed. Chicago: Quintessence. 1997.
18. Shillingburg HT, Hobo S, Whitsett LD, et al. Fundamentals of Fixed Prosthdontics. 3rd ed. Chicago, Quintessence. 1997;85-88.
19. Van Oosterwyjck H, et al. The influence of bone mechanical properties and implant fixation upon bone loading around oral implants. Clin Oral Implants Res. 1998;9:407-418.
20. Esposito M, Ekestubbe A, Gröndahl K. Radiological evaluation of marginal bone loss at tooth surfaces facing single Brånemark implants. Clin Oral Implant Res. 1993;4:151-157.
21. Tarnow DP, Cho SC, Wallace SS. The effect of interimplant distance on the height of inter-implant bone crest. J Periodontol. 2000;71:546-549.
22. Tarnow DP, Choquet V, Hermanns M, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
23. Saadoun AP, Sullivan DY, Krischek M, Le Gall M. Single tooth implant: management for success. Pract Periodontics Aesthet Dent. 1994;6:73-80.
24. Salama H, Salama MA, Garber D, Adar P. The interproximal height of bone: A guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent. 1998;10:1131-1141.
25. Saadoun AP, LeGall M, Touati B. Selection and ideal tridimensional implant position for soft tissue aesthetics. Pract Periodontics Aesthet Dent. 1999;11:1063-1072.
26. Paul SJ, Jovanovic SA. Anterior implant-supported reconstructions: a prosthetic challenge. Pract Periodontics Aesthet Dent. 1999;11:585-590.
27. Grunder U. Stability of the mucosal topography around single-tooth implants and adjacent teeth: 10-year results. Int J Periodontics Restorative Dent. 2000;20:11-17.
28. English CE. The mandibular overdenture supported by implants in the anterior symphysis: A prescription for implant placement and bar prosthesis design. Dent Implantol Update. 1993;4:1-3.
29. Misch CE. Dental Implant Prosthetics. St. Louis, Mo: Mosby. 2005;178.
30. Brosky ME, Korioth TW, Hodges J. The anterior cantilever in the implant-supported screw-retained mandibular prosthesis. J Prosthet Dent. 2003;89(3):244-249.
Authors
Steven Kendrick, DDS
Private Practice
Midwest City, Oklahoma
Instructor
Tulsa Implant Institute
Tulsa, Oklahoma
David Wong, DDS
Private Practice
Tulsa, Oklahoma
Instructor
Tulsa Implant Institute
Tulsa, Oklahoma