You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
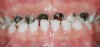
Oral diseases are the most common of the chronic diseases and cause major public health problems worldwide because of their prevalence, impact on individuals and society, and cost of treatment.1 In children, dental caries represents the most common chronic disease despite national public health efforts. Children’s quality of life can be seriously affected by severe caries because of pain and discomfort which could lead to disfigurement, acute and chronic infections, and eating and sleep disruption as well as risk of hospitalization, high treatment costs, and loss of school days with the consequently diminished ability to learn.2 Dental caries also affects the proper development of a child because of its interference with nutrition, growth, and weight gain. Children 3 years of age with early childhood caries have been found to weigh about 1 kg less than treated children; toothaches and infections alter eating and sleeping habits, dietary intake, and metabolic processes (Figure 1).3
Children with dental problems lose approximately 52 million school hours annually;4 low-income children experience nearly 12 times as many restricted activity days from dental disease as children from higher-income families.5 In the United States, dental services are a required coverage for all children under 21 years of age; however, only one third of the eligible population receives services.6 Medicaid covers dental services for children in all 50 states and each state decides what is considered “reasonable standards of dental practice” in consultation with experts.6 Low-income families find the system to be overbearing, the dentists unavailable (particularly those who accept Medicaid), the paperwork burdensome, the attending hours inconvenient, the waiting times long, and appointments difficult to get.7
However, the patterns of dental caries have significantly changed in the last century mainly due to changes in diet and the use of fluorides. High consumption of refined carbohydrates and other processed foods incrementally raises the risk of developing dental caries by providing an adequate source of energy to cariogenic bacteria. The impact of cariogenic diets in the presence of dental caries has been documented by ecological studies.8 In the United States, this decline in prevalence and severity of dental caries was analyzed by the results from the National Dental Caries Prevalence Survey in schoolchildren. From 1988–1994 and 1999–2002, this study observed a reduction in the prevalence of caries in permanent teeth of up to 10% among children aged 6 to 19 years and up to 6% among dentate adults aged > 20 years.9 It also recorded an increase of 13% in dental sealants among children aged 6 to 19 years. Unfortunately, no change in the prevalence of dental caries in primary teeth among children aged 2 to 11 years was found.
Who Has Dental Caries?
The Third National Health and Nutrition Examination Survey reported that about one third of preschoolers from families with incomes under 133% of the poverty level had cavities that could be seen on visual examination using no special instruments. By contrast, only 12% of children from higher-income families had such cavities.10 It was also reported that dental caries rates continue increasing as the child’s age increases. This survey found that not only do more low-income children have decay, but also low-income children affected by caries have more cavities than affluent children affected by caries. For every cavity in groups of children over 300% of the poverty level, there are almost five (4.8) cavities in groups of children under 100% of the poverty level. In terms of ethnicity, black children have more cavities than white children, Hispanic children have more than black children, and Native American and Pacific Islanders have the highest rates of all children.11 More significantly, white children had 1.5 times greater chance of receiving dental care than children of color; higher-income children had a 2.4 times greater chance of receiving care than low-income and working-poor children; and children whose parent(s) had at least a high school education had about twice the chance of receiving care compared to children whose parent(s) did not complete high school.12
More than 40% of children have dental caries by the time they reach kindergarten.13 Infants in a low socioeconomic status, whose mothers have a low education level, and who consume sugary foods are 32 times more likely to have caries at the age of 3 years than children without those risk factors.14 Identifying risk factors for dental caries at an early age should be strongly recommended.
Dental caries is a disease that involves more than just inadequate feeding or hygiene habits; it is a disease with a strong socio-cultural component that must be addressed in order to develop effective interventions against it. Improving access to dental care will positively impact children’s oral health.
Definition Of Caries Risk Assessment
One of the most challenging decisions for a dental professional is to estimate when a particular patient will develop dental caries or—if the patient already has the disease—when a new lesion will be observed. There has been a change in how the dental profession manages dental caries; it has progressed from a surgical model to a disease model.15 The risk-assessment tools currently available do a fairly good job identifying who will not experience a high rate of dental caries lesions, but are less adept at indicating who will be at risk, especially with accurate specificity. Most of the tools currently available are too sensitive (yielding too many false positives) and not specific enough.
Caries risk assessment is the estimation of the probability of developing a new dental caries lesion within a specific timeframe,16 and also the estimation of the probability of a change in the size or activity of existing lesions in the mouth.17 Research in oral health is focused on the early identification of high-risk children or populations to whom prevention therapies can be successfully delivered. Because of the dynamic of dental caries, even the most thoughtfully designed caries risk assessment tool can fail to identify individuals at high risk of the disease. In young children, the characteristics to be observed in order to be classified as high-risk should include but are not limited to children with special healthcare needs; caregivers with evident oral diseases; children with demonstrable dental caries lesions, plaque, or demineralization; children who sleep with their bottle or are breastfed throughout the night; later-order offspring; and children in families of low socioeconomic status.18
Risk Factors For Dental Caries
Dental caries is a multifactorial disease and, therefore, its related factors should be addressed when developing a caries risk assessment tool. These factors can be clustered in microbiologic, clinical, behavioral, environmental, and social variables.19,20
Microbiologic
Dental caries is a consequence of a shift in the ecology and metabolic activity of the biofilm (dental plaque), whereby an imbalance in the equilibrium between tooth mineral and biofilm fluid has developed.21 The biofilm is characterized by continued microbial activity resulting in continued metabolic events in the form of minute pH fluctuations. The cumulative result of the numerous pH fluctuations over months or years is a net loss of calcium and phosphate to an extent that makes the enamel sufficiently porous. Dental caries lesions are a result of imbalances in physiological equilibrium between tooth mineral and biofilm fluid.21
The colonization of normal dental microflora in infants starts with the eruption of the first primary teeth at approximately 6 months of age. The vertical colonization of cariogenic bacteria from mother to infant has been documented. In a study evaluating different mutans streptococci strains in mother-infant pairs, Li et al found identical genotypes in approximately 71% of the study pairs.22 Cariogenic bacteria are passed from mother to the child in the first 1 to 2 years of life.6,23 Recognition that mothers not only serve as the primary vehicle for transmitting the bacteria that can cause tooth decay but also have great influence on shaping the environments in which children develop has led to greater attention to oral health during pregnancy and beyond, an issue with direct relevance to Early Head Start programs and general interest in Head Start.24
Clinical
Individuals with special physical, developmental, mental, sensory, behavioral, cognitive, or emotional healthcare needs are at higher risk for developing oral diseases as a result of their limitations in performing daily self-maintenance activities or substantial limitations in a major life activity.25
Salivary and Genetic Factors
Saliva plays an important role in the development of caries lesions by buffering the pH fluctuations of dental plaque and providing the adequate minerals to remineralize a tooth surface low in structural minerals caused by an altered oral biofilm. Shifts in salivary flow may be the result of congenital or acquired conditions, surgery, radiation treatment, medication, or age-related changes in salivary function. A constantly low salivary flow rate should be included as a risk factor for new caries lesions.26
There is a strong genetic component in the presence of dental caries demonstrated by monozygotic and dizygotic reared-apart twin studies.27 The suggested genetic contribution to the disease is reported to be as high as 40%. Actual data on the genetics of caries susceptibility corroborate this finding but with variable levels of genetic contribution.28
Dental Caries History
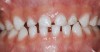
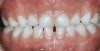
For caries prediction in primary teeth, previous caries experience was the best predictor for the presence of new lesions.29 Enamel caries lesions, also called white spots, represent the beginning of caries lesions in the early clinical stages of the infection (Figure 2). Enamel defects are defined as qualitative or quantitative disturbances in hard tissue matrices.30 The presence of enamel defects was the single best predictor of dental disease at 36 months of age.31
Dietary Factors
The presence of fermentable carbohydrates in the everyday diet is a required factor for dental caries to develop. Sucrose is not only the main source of energy for cariogenic bacteria but also a key element in the synthesis of extracellular glucans, an important microbial virulence feature.32 The increased sugar exposure may lead to an outgrowth of mutans streptococci and other aciduric species highly present in children with several caries lesions.
Based on a systematic review on sugar exposure and dental caries, a cariogenic diet is a more powerful risk factor among children who do not have adequate fluoride exposure. However, when sugar consumption with adequate fluoride exposure was present, a lower risk for dental caries was observed.33 Oral healthcare providers using caries-risk assessment should evaluate individual sugar intake.18
Oral Hygiene
Feeding practices and oral hygiene are critical components in the dental caries process.34 Good oral hygiene habits and noncariogenic feeding practices have been demonstrated to be protective factors for dental caries at very young age.35 Frequent breastfeeding, continuous bottle-feeding at night, and unlimited and constant use of a no-spill training cup are all associated with early childhood caries.36 Traditional counseling approaches targeting positive changes in oral health behaviors have been demonstrated to be ineffective.37 New approaches, such as motivational interviewing, have proved to have an effect on behavioral changes, ultimately reducing the levels of dental caries in young children.38 Understanding the importance of behavioral risk factors should be taken into consideration when designing caries risk-assessment tools.39,40
Environmental
Fluoride has been shown to be the most effective in dental caries prevention when a low level of fluoride is constantly maintained in the oral cavity. The main effect of fluoride in the prevention of dental caries is obtained by topical exposure. Using fluorides to remineralize incipient caries lesions has been suggested, attempted, and utilized in clinical practice for years, yet the detection tools to visualize lesions at this early stage and the ability to detect the effectiveness of remineralization are still unperfected.41
Social
An estimated 80% of decay is found in just 25% of children.42 The caries rate among low-income children aged 3 to 5 years may range from 16% to 65%.43 Children with incomes low enough to qualify for Medicaid had 1.4 times more dental emergency services than higher income children.44 Infants who are of low socioeconomic status, whose mothers have a low education level, and who consume sugary foods are 32 times more likely to have caries at the age of 3 years than children in whom those risk factors are not present.14 Identifying risk factors for dental caries at an early age should be strongly recommended. Urbanization, development of the food industry, and food advertisements induce mothers or caregivers to feed children snacks early and more frequently. Easy access to convenience stores and an increase in small grocery shops in the villages have also promoted sugary food consumption among small children. Having commercial sugary snacks and soft drinks at the age of 1 year has significantly increased the incidence of caries.45
Caries Risk Assessment Tools Available
American Academy of Pediatric Dentistry’s Caries-Risk Assessment Tool (CAT)
The American Academy of Pediatric Dentistry developed its CAT in 2002 based on clinical evidence and expert opinion. The structure of the initial version of the AAPD CAT included a number of risk factors organized into three general domains: clinical considerations, environmental considerations, and general health considerations.46,35 A more recent version of the AAPD CAT divides risk categories into child history (obtained via parental report), clinical evaluation, and supplemental professional assessment (Figure 3).
Caries Management by Risk Assessment (CAMBRA)
Developed in 2002, CAMBRA (0-5 years), provides separate dental and medical caries risk-assessment forms. It identifies risk and protective factors through a parent interview and clinical examination. Bacterial culturing is recommended for children who exhibit certain levels or combinations of risk factors. CAMBRA seeks to serve as a tool for developing individualized treatment and preventive care recommendations based on caries risk level and bacterial culture results.
Cariogram
The Cariogram is a computer-based tool for use by dental providers. It aims to illustrate the interaction between caries-related factors and the probability of developing new caries lesions. The Cariogram uses a pie chart to show an individual’s overall caries risk and the relative contributors to overall risk.47 Because the provider must obtain salivary secretion rates and mutans streptococcus and lactobacillus counts, it relies on assays of clinical specimens for the determination of caries risk.
Conclusion
Dental caries is the most prevalent of the oral health diseases in children affecting more than 50% of all children and 80% of adolescents. Identifying individuals and populations at high risk for dental caries should be performed using a validated caries risk assessment tool. Factors related to dental caries should include microbiologic, clinical, behavioral, environmental, and social variables.
References
1. Locker D. Concepts of Oral Health, Disease and the Quality of Life. 1997; Chapel Hill: University of North Carolina.
2. Petersen P. (2005). WHO’s action for continuous improvement in oral health. Bulletin of the World Health Organization. 2005;(83):9.
3. Acs G, Lodolini G, Kaminsky S, Cisneros GJ. Effect of nursing caries on body weight in a pediatric population. Pediatr Dent. 1992;14:302-305.
4. Gift HC, Reisine ST, Larach DC. The social impact of dental problems and visits. Am J Public Health.1992;82(12):1663-1668.
5. Newacheck P. (2000). Access to health care for children with special health care needs. Pediatrics. 2000;105:760-766.
6. AAP Fact Sheet. 2007. Children’s Health Insurance and Medicaid.
7. Siegal MD. Parent or caregiver, staff, and dentist perspectives on access to dental care issues for head start children in Ohio. Am J Public Health. 2005;95:1352-1359.
8. World Health Organization. 2002; Global Oral Health Data Bank. Geneva: World Health Organization.
9. Dye BA, Tan S, Smith V, et al. Trends in oral health status: United States, 1988-1994 and 1999-2004. Vital Health Stat 11. 2007;(248):1-92.
10. Beltrán-Aguilar ED, Barker LK, Canto MT, et al. Centers for Disease Control and Prevention (CDC). Surveillance for dental caries, dental sealants, tooth retention, edentulism, and enamel fluorosis—United States, 1988–1994 and 1999–2002. MMWR. 2005;54(3):1-43.
11. Vargas CM, Crall JJ, Schneider DA. Sociodemographic distribution of pediatric dental caries: NHANES III, 1988–1994. J Am Dent Assoc. 1998;129:1229-1238.
12. National Center for Health Statistics. Healthy People 2000 Review, 1998-99. 1999; Hyasttsville, MD: Public Health Service.
13. Eldelstein BL, Manksi RJ, Moeller JF. Pediatric dental visits in 1996: an analysis of the federal Medical Expenditure Panel Survey. Pediatr Dent. 2000;22:17-20.
14. Pierce KM, Rozier R, Vann WF. Accuracy of pediatric primary care providers’ screening and referral for early childhood caries. Pediatrics. 2002;109(5):82.
15. Nowak AJ, Warren JJ. Infant oral health and oral habits. Pediatr Clin North Am. 2000;47:1043-1066.
16. National Institutes of Health. Diagnosis and management of dental caries throughout life. 2001; Bethesda, Md: National Institutes of Health.
17. Reich E, Lussi A, Newbrun E. Caries-risk assessment. Int Dent J. 1999;49(1):15-26.
18. Fontana M, Zero DT. Assessing patients’ caries risk. J Am Dent Assoc. 2006;137(9): 1231-1239.
19. American Academy of Pediatric Dentistry. Reference Manual. 2009;31(6):29-33.
20. Beck JD, Kohout F, Hunt RJ. Identification of high caries risk adults: Attitudes, social factors and diseases. Int Dent J. 1988;38(4):231-238.
21. Shiboski CH, Gansky SA, Ramos-Gomez F, et al. The association of early childhood caries and race/ethnicity among California preschool children. J Public Health Dent. 2003;63(1):38-46.
22. Fejerskov O. Dental caries: The Disease and its Clinical Management. 2008. UK: Blackwell Publishing Ltd.
23. Li Y, Ismail AI, Ge Y, et al. Similarity of bacterial populations in saliva from African-American mother-child dyads. J Clin Microbiol. 2007;45(9):3082-3085.
24. National Institute of Dental Research. Oral Health of the United States Children: The National Survey of Dental Caries in School Children, 1986-1987. 1989; Department of Health and Human Services publication.
25. Crall JJ. Head Start’s potential for catalyzing improvements in oral health and school readiness for children, families and communities. Dialog Briefs. 2007;10:1-7.
26. American Academy of Pediatric Dentistry. Definition of persons with special health care needs. Pediatr Dent. 2005;27(Suppl):15.
27. Leone CW, Oppenheim FG. Physical and chemical aspects of saliva as indicators of risk for dental caries in humans. J Dent Educ. 2001;65(10):1054-1062.
28. Bretz WA, Corby PM, Melo MR, et al. Heritability estimates for dental caries and sucrose sweetness preference. Arch Oral Biol. 2006;51(12):1156-1160.
29. Slayton RL, Cooper ME, Marazita ML. Tuftelin, mutans streptococci, and dental caries susceptibility. J Dent Res. 2005;84(8):711-714.
30. Zero D, Fontana M, Lennon AM. Clinical applications and outcomes of using indicators of risk in caries management. J Dent Educ. 2001;65(10):1126-1132.
31. Clarkson J. Review of terminology, classifications, and indices of developmental defects of enamel. Adv Dent Res. 1989;3(1):104-109.
32. Chavez AM, Rosenblatt A, Oliveira OF. Enamel defects and its relation to life course events in primary dentition in Brazilian children: A longitudinal study. Comm Dent Health. 2007;24(1):31-36.
33. Fejerskov O. Changing paradigms in concepts on dental caries: consequences for oral health care. Caries Res. 2004;38(3):182-191.
34. Burt B, Pai S. Does low birthweight increase the risk of caries? A systematic review. J Dent Educ. 2001;65(10):1024-1027.
35. Keyes P. The infectious and transmissible nature of experimental dental caries. Arch Oral Biol. 1960;1:304-320.
36. American Academy of Pediatric Dentistry. Reference Manual. 2009;31(6):40-43.
37. Reisine S, Douglass JM. Psychosocial and behavioral issues in early childhood caries. Comm Dent Oral Epidem. 1998;26(Suppl 1):32-44.
38. Tinanoff N. Dental caries risk assessment and prevention. Dent Clin North Am. 1995;39(4):704-719.
39. Weinstein P, Harrison R, Benton T. Motivating mothers to prevent caries: confirming the beneficial effect of counseling. J Am Dent Assoc. 2006;137(6):789-793.
40. Petersen PE, Lennon MA. Effective use of fluorides for the prevention of dental caries in the 21st century: the WHO approach. Comm Dent Oral Epidemiol. 2004; 32:319-21.
41. Marinho VC, Higgins JP, Logan S, Sheiham A. Fluoride toothpastes for preventing dental caries in children and adolescents (Cochrane review). In: The Cochrane Library, Issue 1, 2004. Chichester, UK: John Wiley & Sons Ltd.
42. Donly KJ, Stookey GK. Topical Fluoride Therapy. In: Primary Preventive Dentistry. 6th ed. Harris NO, Franklin Garcia-Godoy F, eds. 2004;241-283. Upper Saddle River: Pearson Prentice Hall.
43. Kaste LM, Selwitz R, Oldakowski RJ, et al. Coronal caries in the primary and permanent dentition of children and adolescents 1-17 years of age: United States, 1988-1991. J Dent Res. 1996;75(Spec Iss):631-641.
44. Edelstein BL. Dispelling the myth that 50 percent of US schoolchildren have never had a cavity. Public Health Rep. 1995;110:522-530.
45. Amudson C. 1999. Dental Director Health Partners. Minneapolis, Minn.
46. Thitasomakul S, Piwat S, Thearmontree A, et al. Risks for early childhood caries analyzed by negative binomial models. J Dent Res. 2009;88(2):137-141.
47. American Academy of Pediatrics. The Medical Home. Pediatrics. 2002;110:184-186.
48. Bratthall D. Petersson GH. Cariogram—a multifactorial risk assessment model for a multifactorial disease. Comm Dent Oral Epidemiol. 2005;33:256-264.
About the Authors
Ana Lucia
Seminario, DDS, PhD
Acting Assistant Professor
University of Washington
Department of
Pediatric Dentistry
Seattle, Washington
Joel Berg, DDS, MS
Professor
Lloyd and Kay Chapman Chair for Oral Health University of Washington
Department of
Pediatric Dentistry
Director of Dentistry, Seattle Children’s Hospital
Seattle, Washington