You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Many patients seek dental care when they are recovering from serious illnesses; others have chronic conditions and take many medications. The dental healthcare provider should use four basic concepts before providing dental care: Will the patient be able to endure the physiologic stress of the procedure? Will the patient have adequate hemostasis? Is there any increased susceptibility to infection? Will drug actions and interactions cause any complications?
Some of these questions can be answered by reviewing clinical laboratory test results. As with many other areas of healthcare, the use of laboratory testing has expanded greatly in the past decade, mostly due to the development of automated testing devices and computerized reporting. These results about a patient’s condition can provide valuable information for diagnosis and management of orofacial conditions, guidance on assessing the patient’s ability to tolerate the proposed dental treatment, and a prognosis based on a particular treatment. The use of clinical laboratory tests (blood and other bodily specimens) in the general practice of dentistry is often limited because of insufficient education and training. These articles, presented in a two-part series, describe the common laboratory tests and provide general guidelines for a patient evaluation. The information should not be used in lieu of appropriate medical consultations and referrals.
Some important points about acquiring laboratory results can be summarized as follows. A patient with complex medical problems will probably receive routine tests ordered by the physician to monitor disease status, organ function, or metabolic reactions to medications. The most recent results should be readily available through the physician’s office. When these are not accessible or if the dentist observes a sign of poor disease control, the physician should be consulted so that the physician can order the appropriate test(s). Occasionally, the dentist can specifically order a laboratory test. However, this implies a previous relationship with a testing laboratory and the understanding of medical diagnosis and procedure codes, which are necessary to include with the laboratory test in order to bill the patient’s medical insurance company.
The typical laboratory report will include the patient’s demographic data; date and time that the specimen was collected; and the ordering physician’s name. The specific results will be accompanied by the normal test range, which may vary between laboratories. Abnormal results are often indicated with H (high) or L (low) or may be printed in bold or color. Some reports will also include historical data, eg, the viral load results for a few years in a patient with human immunodeficiency virus (HIV), with comments regarding the degrees of change. While these indicators help, treatment decisions should never be made solely on these results.
HIV/AIDS Laboratory Evaluation
Dental treatment is a necessary component of managing the patient with HIV or acquired immunodeficiency syndrome (AIDS). Oral manifestations are common, especially as the patient’s immune system deteriorates. The dentist may be the first healthcare provider to become suspicious of HIV infection because certain opportunistic infections appear in the orofacial region. Although state laws differ, it is likely that in the near future, dental offices will be an alternate location for employing the rapid tests that check oral fluids for antibodies to HIV-1 and HIV-2. (One caveat is that counseling a patient who has just received a diagnosis of HIV is an essential part of testing; this aspect may be a critical point when a dental clinician is deciding whether to provide these tests.)
For patients who are known to be infected with HIV, several routine laboratory tests should be reviewed regularly before invasive dental treatment is provided. These include HIV viral load, cluster of differentiation 4 (CD4) count and percentage, absolute neutrophil count (ANC), and platelet count (PC). Most well-monitored patients with HIV have blood tests every 2 to 6 months.1
Viral load is the number of HIV copies per milliliter in the plasma (#/mL); the higher the viral load, the more active the HIV infection. For some patients, the amount of virus is used to determine whether the administration of antiretroviral medications should be initiated. The optimal value is expressed as “nondetectable” because the typical test employs the polymerase chain reaction (PCR) to amplify the amount of HIV ribonucleic acid (RNA) in a volume of blood.2 Other tests report the lowest possible amount as < 48 copies/mL or similar values.
When test findings show that the HIV viral load has increased, these findings may indicate that the immune system is deteriorating and/or medications are failing. Changes that are less than approximately 0.5 log 10 copies/mL, which is a 3-fold change, usually are not clinically significant.3
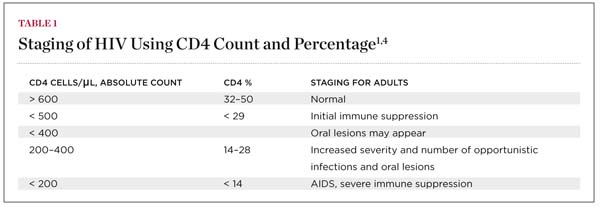
CD4 cells are a subset of lymphocytes, or T-cells, and are particularly susceptible to destruction by HIV. The number of CD4 cells is reported as part of a list of several types of lymphocytes and used in HIV staging (Table 1).4 The value is usually reported as an absolute count, as well as a percentage of total lymphocytes. The absolute CD4 count per microliter (µL) is most often the index used in clinical practice, while the percentage is employed to assess immune function. Cluster of deviation 8 (CD8) cells, also called cytotoxic T cells, are no longer used to predict clinical outcomes, although they are still reported in many tests.1,3
 |
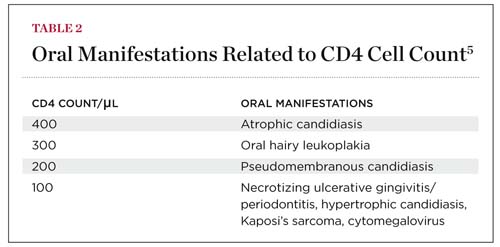
The CD4 count also helps to determine the need for and response to antiretroviral therapy. Oral manifestations have been correlated to CD4 counts (Table 2). If the dental healthcare provider observes certain oral lesions, the physician should be notified that the HIV may be progressing and a change in medications may be indicated.5
 |
Before any elective invasive dental treatment is performed for a patient with HIV, the complete blood count (CBC) with differential, specifically the ANC and PC, also should be evaluated. As HIV progresses, patients experience anemia, leukopenia, and thrombocytopenia.2 When the ANC is < 500 cells/mL, antibiotics should be added perioperatively.6 For example, penicillin VK 500 mg should be provided starting 1 hour before the invasive dental procedure and continued with 500 mg every 6 hours for 5 days.7 If PCs fall below 50,000/mL, elective dental treatment should be deferred in order to avoid the risk of postoperative bleeding.
The ideal situation for the dentist who is treating a patient with HIV is the opportunity to evaluate a series of test results taken over time, eg, 12 months. The goal of medical management is to have a normal CD4 count that stays high and an undetectable or low HIV viral load that stays low. Emergency dental care must be provided at any time; however, knowing ANC and PC values at the time of treatment allows the dental healthcare provider to manage any infections or bleeding problems.1
Hemostasis
Hemostasis is a complex process that includes the coagulation factor cascade and platelet activation. The effect of therapeutic medications, such as warfarin and heparin, are measured with specific laboratory tests that will be described in this section. See the section below regarding the use of platelet inhibitor medications and treatment modifications during dental treatment.
Warfarin is a commonly used medication in the United States with more than 22 million prescriptions filled in 2008.8 This is an anticoagulant used to reduce the risk of myocardial infarction (MI) or stroke. Patients with atrial fibrillation, prosthetic heart valves, a history of MI or cerebrovascular accident, or deep venous thrombosis are given this medication. It interferes with the vitamin K-dependent coagulation factors, and the function of these factors is measured with the prothrombin time (PT) test. The normal range of PT is 11 to 15 secs, and therapeutic range is expressed as a ratio of the medicated time to normal, eg, PTR 1.5 (PT ratio one-and-a-half times normal).
The international normalized ratio (INR) is the standard test used to measure the therapeutic level of anticoagulation with warfarin therapy. It was endorsed by the World Health Organization in the 1980s9 to facilitate comparisons of PTRs from one region of the world to another. This allowed physicians to collaborate on the best therapy for specific conditions. Recommendations have been published that give guidance based on the condition being managed10 (Table 3).
 |
Many factors can alter the level of anticoagulation that is caused by the use of warfarin. These include genetics, age, drugs, diet, and conditions such as hepatic dysfunction, malabsorption syndrome, or hyperthyroidism.11 In one study, as many as two thirds of patients using warfarin were also taking prescription or over-the-counter medications that altered the anticoagulant effect both positively and negatively.12 Some medications increase the metabolism of warfarin, while others potentiate its effects adversely. Events such as intracranial hemorrhage, occult gastrointestinal hemorrhage, and anemia have been well documented.10-12 For patients taking oral warfarin, INR testing is recommended every 4 weeks or less.11
Much research has been published that addresses the risks of discontinuing warfarin for a period prior to invasive dental treatment.13-15 A critical appraisal of the existing guidelines related to the management of these patients’ conditions16 supports the concept that the risk of a significant thromboembolic event outweighs the bleeding risk associated with a limited invasive dental procedure. Specifically, if the INR is less than or equal to 3.5 within 24 to 72 hours before minor dental surgical procedures, no adjustment of warfarin is needed. These minor dental procedures include simple extraction of fewer than three teeth, gingival surgery, crown-and-bridge work, scaling, and surgical removal of teeth.16
The partial thromboplastin time (PTT) test is used for patients who are taking heparin, or for identification of other bleeding disorders (eg, hemophilia) or decreased liver function. A normal value for PTT is 25 to 35 seconds. The activated partial thromboplastin time (aPTT) is a modified, more sensitive test, which is used for the monitoring of heparin therapy.17
Antiplatelet Medicationsand Dental Treatment
Thrombocytopathy refers to altered platelet function and can be related to diseases and conditions, such as von Willebrand disease, or acquired by taking certain medications. Clinical signs include prolonged bleeding after injury or surgery, spontaneous nosebleeds, or easy bruising. The bleeding test and platelet function analysis are used to evaluate platelet function. Both are largely qualitative and not widely used. The platelet count may be normal; however, the platelets do not work properly.
The use of antiplatelet medications, such as clopidogrel and aspirin, has become extremely common in the last few years. Typically, these patients have cardiovascular disease; they may have had MIs and/or placements of coronary artery stents. Many dentists are confronted with the decision of discontinuing these medications in such patients prior to surgical treatment.
In 2007, the American Heart Association, American College of Cardiology, Society for Cardiovascular Angiography and Interventions, American College of Surgeons, and American Dental Association published a joint statement that advised against the discontinuation of antiplatelet medications for patients with drug-eluting coronary artery stents.18
Napenas and colleagues recently published a retrospective study showing no episodes of prolonged postoperative bleeding in patients using single and dual antiplatelet therapy. The dental procedures included extractions, periodontal surgery, and subgingival scaling and root planing.19 Dental healthcare providers should be prepared with local hemostatic measures, such as hemostatic dressings, sutures, and pressure appliances. The use of non-steroidal anti-inflammatory drugs (NSAIDs) employed for postoperative pain should be avoided because they may increase the risk of a bleeding episode.16
Liver Disease
The liver has many functions: the production of proteins, the storage of sugar and bile, and the inactivation of chemicals and waste products. A large variety of diseases affect the liver; among these are viral hepatitis and alcohol-related liver disease. Signs and symptoms vary, and the presence of jaundice, easy bruising, ascites, fatigue, abdominal tenderness, and confusion do not consistently occur and are not quantitative for the degree of impaired function.
Perhaps the most important liver functions to dental healthcare providers are drug metabolization and production of clotting factors. The evaluation of overall liver function is accomplished using a group of tests related to its functions (Table 4). Abnormal test results may indicate significantly impaired hemostasis (due to the lack of sufficient coagulation factors) and/or impaired detoxification or activation of medications that may be prescribed during dental treatment.
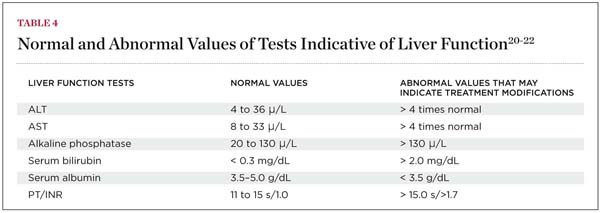 |
Unlike renal disease, in which estimates of renal function based on creatinine clearance correlate with parameters of drug elimination such as clearance and half-life, routine liver function tests do not reflect actual liver function. Instead, they are markers of liver cellular damage. Serum levels of the liver enzymes alanine aminotransferase (ALT), aspartate aminotransferase (AST), and alkaline phosphatase will rise when the hepatocytes are damaged by toxins or viral replication. Although elevated levels of these enzymes indicate liver damage, they do not always reflect the functional capacity of the liver or the extent of dysfunction.20 Further data analyses include the ratio of these values to each other and the magnitude of increase of the above-normal value. For example, an AST/ALT greater than 2 (the normal ratio is 1) is indicative of alcoholic hepatitis, cirrhosis, or chronic viral hepatitis.21 ALT or AST four times more than normal is indicative of significant hepatic dysfunction, and medication doses may need alteration.20,21
Serum bilirubin will rise when the liver is unable to conjugate this breakdown product of red blood cells and excrete it. Serum albumin levels fall when the liver cannot produce it. PT will rise when the liver cannot make clotting factors (see section on hemostasis).
Recommendations for Dental Treatment Modifications of Patients with Liver Disease
When one or more of the following exists:21-24
- AST/ALT levels four times more than normal
- Serum bilirubin > 2 mg/dL
- Serum albumin < 3.5 g/dL
- INR greater than 1.7 attributable to hepatic failure
- Presence of ascites attributable to hepatic failure or hepatic encephalopathy
Surgical procedures. Consider local hemostatic measures, blood product transfusion, and/or hospitalization for complex procedures.
Local anesthetics of the amide family should be used cautiously in patients with hepatic impairment. The elimination half-life of a lidocaine injection is typically 90 to 120 minutes, which may be twofold or more in patients with liver dysfunction. One study measured this up to 343 minutes, or nearly 6 hours.25 A dose of 40 mg to 60 mg of lidocaine injected intraorally leads to blood levels of approximately 1 µg/mL; toxic effects in a conscious patient can occur at 5 µg/mL.26 To avoid lidocaine or other local anesthetic toxicity, it is recommended that the maximum dosage for these patients with liver disease be reduced to a maximum of three cartridges of local anesthetic per visit.
As an alternative to lidocaine, articaine is suggested as a local anesthetic for patients with liver dysfunction. While classified as an amide, articaine contains an ester side chain on a thiophene ring structure. This modification allows articaine to be initially metabolized in the serum rather than in the liver, and toxicity related to liver dysfunction should be less of a potential problem.
Caution should be used in prescribing analgesic medications that are metabolized in the liver, eg, acetaminophen and NSAIDs. Lower dosages may be indicated, or the dose-interval may need to be increased.
Avoid erythromycin, metronidazole, and tetracycline. Erythromycin and metronidazole are known inhibitors of cytochrome P450 enzymes; their use can lead to decreased metabolism of other substances, especially other medications. Erythromycin may also result in hepatocellular and/or cholestatic hepatitis by directly injuring hepatocytes or cholangiocytes. Tetracycline use can cause drug-induced liver injury by altering hepatocyte mitochondrial fatty acid oxidation and hepatic steatosis; however, these events are rare when tetracycline is administered orally.27
Conclusion
The laboratory assessment of the dental patient to assess the medical stability of HIV/AIDS, hemostasis, and liver disease is a vital component of risk assessment prior to invasive dental care. The information obtained by preoperative laboratory tests allows the clinician to make informed decisions regarding the provision of dental care and facilitates treatment modifications to minimize complications.
References
1. The Monograph Series on Oral Treatment of HIV+ Patients in Private Practice. Denver, Colorado: Howard Dental Center for HIV/AIDS Oral Medicine; 2006.
2. Aberg JA, Kaplan JE, Libman H, et al. HIV Medicine Association of the Infectious Diseases Society of America. Primary care guidelines for the management of persons infected with human immunodeficiency virus: 2009 update by the HIV medicine Association of the Infectious Diseases Society of America. Clin Infect Dis. 2009;49(5):651-681.
3. Clinical manual for management of the HIV-infected adult. National AIDS Education and Training Centers National Resource Center. http://www.aidsetc.org/aetc?page=cm-00-00. Accessed November 30, 2009.
4. Clinician’s Guide to HIV-infected Patients. 3rd ed. Patton LL, ed. The American Academy of Oral Medicine, 2001.
5. Glick M. Oral diseases of HIV-associated immune suppression (ODHIS): a new classification system. Journal of Japanese Society for Oral Mucous Membrane. 2004;10(2):56.
6. Patton LL, Shugars DA, Bonito AJ. A systematic review of complication risks for HIV-positive patients undergoing invasive dental procedures. J Am Dent Assoc. 2002;133(2):195-201.
7. Shirlaw PJ, Chikte U, MacPhail L, et al. Oral and dental care and treatment protocols for the management of HIV-infected patients. Oral Dis. 2002;8(Suppl 2):136-143.
8. Lamb E. Top 200 drugs of 2008. Pharmacy Times. 2009 (May), Published online at http://www.pharmacytimes.com/issue/pharmacy/2009/2009-05/RxFocusTop200Drugs-0509. Accessed January 20, 2010.
9. Expert Committee on Biological Standardization. Requirements for thromboplastins and plasma used to control oral anticoagulant therapy. World Health Organ Tech Rep Ser. 1983;33:81-105.
10. Hirsh J, Guyatt G, Albers GW, et al. American College of Chest Physicians. Antithrombotic and thrombolytic therapy: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th edition). Chest. 2008;133(Suppl 6):110S-112S.
11. Ansell J, Hirsh J, Poller L, et al. The pharmacology and management of the vitamin K antagonists: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(Suppl 3):204S-233S.
12. Feldstein AC, Smith DH, Perrin N, et al. Reducing warfarin medication interactions: an interrupted time series evaluation. Arch Intern Med. 2006;166(9):1009-1015.
13. Blinder D, Manor Y, Martinowitz U, et al. Dental extractions in patients maintained on oral anticoagulant therapy: comparison of INR value with occurrence of postoperative bleeding. Int J Oral Maxillofac Surg. 2001;30(6):518-521.
14. Blinder D, Manor Y, Marinowitz U, et al. Dental extractions in patients maintained on continued oral anticoagulant: comparison of local hemostatic modalities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(2):137-140.
15. Wahl MJ. Dental surgery in anticoagulated patients. Arch Intern Med. 1998;158(15):1610-1616.
16. van Diermen DE, Aartman IH, Baart JA, et al. Dental management of patients using antithrombotic drugs: critical appraisal of existing guidelines. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107(5):616-624.
17. Greer JP, Foerster J, Rodgers GM, et al. Wintrobe’s Clinical Hematology. 12th ed. Philadelphia, PA: Lippincott, Williams & Wilkins; 2008.
18. Grines CL, Bonow RO, Casey DE Jr, et al. Prevention of premature discontinuation of dual antiplatelet therapy in patients with coronary artery stents: a science advisory from the American Heart Association, American College of Cardiology, Society for Cardiovascular Angiography and Interventions, American College of Surgeons, and American Dental Association, with representation from the American College of Physicians. Circulation. 2007;115(6):813-818.
19. Napeñas JJ, Hong CH, Brennan MT, et al. The frequency of bleeding complications after invasive dental treatment in patients receiving single and dual antiplatelet therapy. J Am Dent Assoc. 2009;140(6):690-695.
20. Glick M. Medical considerations for dental care of patients with alcohol-related liver disease. J Am Dent Assoc. 1997;128(1):61-70.
21. Firriolo FJ. Drug use in hepatic dysfunction. In: Hupp JR, Williams TP, Firriolo FJ, eds. Dental Clinical Advisor. 1st ed. St. Louis, MO: Mosby; 2006:476.
22. Little JW, Falace DA, Miller CS, et al.
23. Golla K, Epstein JB, Cabay RJ. Liver disease: current perspectives on medical and dental management. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;98(5):516-521.
24. Douglas LR, Douglass JB, Sieck JO, et al. Oral management of the patient with end-stage liver disease and the liver transplant patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;86(1):55-64.
25. Thomson PD, Melmon KL, Richardson JA, et al. Lidocaine pharmacokinetics in advanced heart failure, liver disease, and renal failure in humans. Ann Intern Med. 1973;78(4):499-508.
26. Mehra P, Caiazzo A. Maloney P. Lidocaine toxicity. Anesth Prog. 1998;45(1):38-41.
27. Leitner JM, Graninger W, Thalhammer F. Hepatotoxicity of antibacterials: pathomechanisms and clinical data. Infection. 2010;38(1):3-11.
About the Authors
Wendy S. Hupp, DMD
Assistant Professor of Oral Medicine
Department of General Dentistry and Oral Medicine
University of Louisville, School of Dentistry
Louisville, Kentucky
F. John Firriolo, DDS, PhD
Professor and Director
Division of Oral Medicine
Department of General Dentistry and Oral Medicine
University of Louisville, School of Dentistry
Louisville, Kentucky
Scott S. De Rossi, DMD
Associate Professor of Oral Medicine
Chairman, Department of Oral Health and Diagnostic Sciences
Medical College of Georgia
Augusta, Georgia