You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Many types of ceramic materials and processing techniques have been introduced throughout the years. As early as 1903, Charles Land patented all-ceramic restorations, using fired porcelains for inlays, onlays, and crowns.1 Insufficient understanding about material requirements for survival in the oral environment, poor ceramic processing techniques, and the inability for adhesive cementation led to early catastrophic failure. Since then, all imaginable varieties of materials and techniques from very conservative ceramic restorations to very complex porcelain veneered of either metal or high-strength crystalline ceramics have been introduced and tried with varying levels of success.2 The authors have previously published two detailed descriptions, or classification systems, for ceramics used in dentistry—one based on the microstructure of the material and the second on how the material is processed.3 There is considerable misinformation and a general lack of rational treatment planning guidelines published regarding the use of different ceramics in dentistry. The literature is replete with various accounts of clinical success and failures of all types of dental treatments. Sadowsky4 published a review of the literature covering treatment considerations using esthetic materials, eg, whether to use amalgam or composite and the success rates of different treatments. No recent literature could be found presenting a thorough discussion of when to use the various ceramics, eg, when feldspathic porcelains should be used, when either pressed or machined glass-ceramics are appropriate, when different types of glass-ceramics should be employed, when a high-strength all-ceramic crown system of either alumina or zirconia is ideal, and when metal-ceramics are suitable. This article provides a systematic stepwise process in treatment planning ceramic materials and presents specific guidelines for the appropriate clinical conditions for applications of the various systems.
Treatment Philosophy
Before making any decision regarding the use of a material or technique, a dental practitioner must have a treatment philosophy based on current standards of care that consider the patient's esthetic requirements. More importantly, this philosophy should be aimed at maintaining the long-term biologic and structural health of the patient in the least destructive way. Restorative or esthetic dentistry should be practiced as conservatively as possible. The use of adhesive technologies makes it possible to preserve as much tooth structure as feasible while satisfying the patient's restorative needs and esthetic desires.5 The philosophy today is not to remove any healthy tooth structure unless absolutely necessary. Our goal would be to not remove excessive amounts of enamel and expose the dentin when orthodontics would have been the ideal treatment. With restorations, clinicians should choose a material and technique that allows the most conservative treatment in order to satisfy the patient's esthetic, structural, and biologic requirements and has the mechanical requirements to provide clinical durability. Each of these requirements could be the topics of individual articles.
There are four broad categories, or types of ceramic systems, from which to choose: Category 1: powder/liquid feldspathic porcelains; Category 2: pressed or machined glass-ceramics; Category 3: high-strength crystalline ceramics; and Category 4: metal-ceramics. Category 1 (porcelains)—are the most esthetic, especially in thin sections and thus can be used the most conservatively, but are the weakest.3,6 Category 2 (glass-ceramics) also can be very translucent but requires slightly thicker dimensions for workability and esthetics than Category 1. Although demonstrating progressively higher fracture resistance, Categories 3 and 4 are more opaque and, therefore, require additional tooth reduction that produces a less conservative alternative. Based on the treatment goal of being as conservative as possible, the first choice will always be porcelains, then glass-ceramics, followed by high-strength ceramics or metal-ceramics. The decision will be based on satisfying all the treatment requirements, ie, if the more conservative material can meet all the treatment requirements, then that is the ideal choice. This article will identify the clinical conditions in which treatment requirements dictate the use of a specific category.
Five Clinical Parameters to Evaluate for Choosing a Material
The evaluation of individual teeth for specific material selection involves first determining the final 3-D posttreatment position of the tooth. After determining that, the clinician must have an understanding of the space requirements for using a specific material, the amount of color change required from the original situation, the condition of the substrate, the amount and type of stresses the restoration will undergo, the amount of potential flexure, and the potential for bond failure.
1. Space Required and Color Change for Esthetics
The first consideration is the final 3-D position of the teeth, ie, smile design. The reader has several resources for smile design.7,8 Second, the color change desired from the substrate (tooth) must be determined because this will dictate the restoration thickness. In general with porcelains, the dentist needs a porcelain thickness of 0.2 mm to 0.3 mm for each shade change (A2 to A1 or 2M1 to 1M1). For example, A3 to A0 would require a veneer 0.6-mm to 0.9-mm thick. Glass-ceramics need the same space requirements as porcelain for effective shade change; however, the authors find it difficult to work with this category and to produce the best esthetic results if the material is less than 0.8 mm. High-strength all-ceramic crowns require a thickness of 1.2 mm to 1.5 mm, depending on the substrate color; metal-ceramics need a thickness of at least 1.5 mm to create lifelike esthetics. With that in mind, a diagnosis based on tooth position and color change will direct treatment planning as well as the final decision regarding tooth preparation design (ie, total tooth structure reduction) and whether a combination of orthodontic treatment is required to facilitate a more conservative, esthetic outcome.
2. Substrate
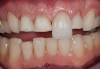
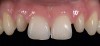
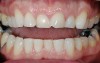
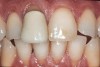
The second consideration is evaluating the substrate to which the material will be attached (Figure 1). Is it enamel? How much of the bonded surface will be enamel? How much enamel is on the tooth? Is it dentin? How much of the bonded surface will be dentin? What type of dentin will the restoration be bonded to (ie, tertiary or sclerotic dentin exhibits very poor bond strength, and bonding to this type of dentin should be avoided when possible)? Is it a restorative material (eg, composite, alloy)? These questions should be addressed for each tooth to be restored because this will be one major parameter for material selection. It is generally understood and accepted that predictable and high bond strengths are achieved when restorations are bonded to enamel, given the fact that the stiffness of enamel supports and resists the stresses placed on the materials in function. It is equally understood that bonding to dentin surfaces—as well as to composite substrates—is less predictable given the variability and flexibility of these substrates. The more stress placed on the bonds between dentin and composite substrates and the restoration, the more damage is likely to occur to the restoration and underlying tooth structure. Therefore, because enamel is significantly stiffer than either dentin or composite and much more predictable for bonding, it is the ideal substrate for bonded porcelain restorations.
3. Flexure Risk Assessment
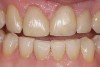
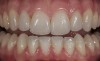
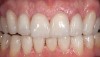
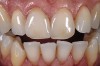
Next is the flexure risk assessment. Each tooth and existing restoration is evaluated for signs of past overt tooth flexure. Signs of excessive tooth flexure can be excessive enamel crazing (Figure 2), tooth and restoration wear, tooth and restoration fracture, microleakage at restoration margins, recession, and abfraction lesions. Often, the etiology is multifactorial and controversial. However, if several of these conditions exist, there is an increased risk of flexure on the restorations that are placed, which may overload weaker materials. Evaluation of this possibility is also based on the amount of remaining tooth structure. The more intact the enamel is, the less potential for flexure. The amount of tooth preparation can directly affect tooth flexure and stress concentration. There is much potential subjectivity in any observational assessment of clinical conditions; however, an assessment of flexure potential for each tooth to be restored is needed. A subjective assignment of Low, Medium, or High Risk for flexure is based on the evaluated parameters, as outlined below. Low Risk: There is low wear, minimal-to-no fractures or lesions in the mouth, and a reasonably healthy oral condition. Medium Risk: Signs of occlusal trauma are present; mild-to-moderate gingival recession exists, along with inflammation; bonding mostly to enamel is still possible; and there are no excessive fractures. High Risk: Occlusal trauma from parafunction is evident, more than 50% dentin exposure exists, there is significant loss of enamel due to wear of 50% or more, and porcelain must be built up more than 2 mm.
4. Excessive Shear and Tensile Stress Risk Assessment
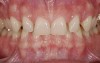
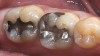
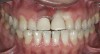
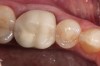
The fourth parameter is the risk (or amount) of ongoing shear and tensile stresses that the restoration will undergo, because the prognosis is more guarded for specific materials. All types of ceramics (especially porcelains) are weak in tensile and shear stresses.9 Ceramic materials perform best under compressive stress. If the stresses can be controlled, then weaker ceramics can be used, eg, bonded porcelain to the tooth. The same parameters are evaluated, similar to flexure risk, eg, deep overbites and potentially large areas where the ceramic would be cantilevered (Figure 3). If a high-stress field is anticipated, stronger and tougher ceramics are needed; if porcelain is used as the esthetic material, the restoration design should be engineered with such support (usually a high-strength core system) that it will redirect shear and tensile stress patterns to compression. To achieve that, the substructure should reinforce the veneering porcelain by using the reinforced porcelain system, which is generally accepted in the literature as a metal-ceramic concept.10 The practitioner can assess and categorize Low, Medium, or High Risk for tensile and shear stress based on the parameters and symptoms mentioned above.
5. Risk of Bond Failure
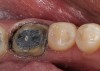
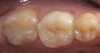
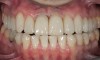
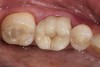
The fifth parameter is the risk of losing the bond or seal of the restoration to the tooth over time. Glass matrix materials, which are the weaker powder/liquid porcelains, and the tougher pressed or machined glass-ceramics absolutely require maintenance of the bond and seal for clinical durability.11,12 Due to the nature of the glass matrix materials and absence of a core material, the veneering porcelains are much more susceptible to fracture under mechanical stresses. Therefore, a good bond in combination with a stiffer tooth substructure (eg, enamel) is essential to reinforce the restoration. If the bond and seal cannot be maintained, then high-strength ceramics or metal-ceramics are the most suitable because these materials can be placed using conventional cementation techniques. Clinical situations in which the risk is higher for bond failure are: 1) moisture control problems; 2) higher shear and tensile stresses on bonded interfaces; 3) variable bonding interfaces (eg, different types of dentin); 4) material and technique selection of bonding agents (ie, as dictated by such clinical situations as the inability to achieve proper isolation for moisture control to enable the use of adhesive technology); and 5) the experience of the operator (Figure 4). An assignment of Low, Medium, or High Risk for bond and seal failure is based on the evaluated parameters.
Category 1: Powder/Liquid Porcelains
Bonded pure porcelain restorations are ideal as the most conservative choice but are the weakest materials and require specific clinical parameters to be successful.13 Many good materials and techniques are available for bonded porcelain (eg, Creation, Jensen Dental, www.jensendental.com; Cermaco® 3, DENTSPLY, www.dentsply.com; EX-3, Noritake, www.noritake-dental.co.
jp). The authors use Vita® VM 13 (Vita Zahnfabrik, www.vita-zahnfabrik.com) when 3-D master shades are taken and Halo (Shofu, www.shofu.com) when classic shades are taken. When following clinical parameters and guidelines at the UCLA Center for Esthetic Dentistry, the authors have observed similar success rates with these materials when compared with porcelain-fused-to-metal (PFM) materials (ie, less than a 1% fracture rate if all parameters are followed) (Figure 5 and Figure 6).
Esthetic Factors
Space requirements for shade change: 0.2 mm to 0.3 mm for each shade change.
Environmental Factors
1. Substrate condition: A rate of 50% or more remaining enamel is on the tooth, 50% or more of the bonded substrate is enamel, and 70% or more of the margin is in enamel. These percentages are subjective assessments based on an overall evaluation of all parameters affecting the teeth to be restored and may influence material selection. If bonding to some dentin substrate, the dentin should be mostly unaffected and superficial because sclerotic dentin exhibits very poor bond strength.
2. Flexure risk assessment: A higher-risk and more guarded prognosis is presented when bonding to dentin. Due to dentin's flexible nature, avoiding the use of low-fracture resistance restorative materials is recommended; therefore, the presence of a higher percentage of enamel (ie, at least 70% in high-stress areas such as the margins) is recommended when restoring using powder/liquid materials (Category 1). By increasing the presence of enamel, the prognosis is improved. Depending on the dentin/enamel ratio, the risk can be assessed between low to moderate.
3. Tensile and shear stress risk assessment: Low-to-low/moderate risk. Large areas of unsupported porcelain, deep overbite or overlap of teeth, bonding to more flexible substrates (eg, dentin and composite), bruxing, and more distally placed restorations increase the risk of exposure to shear and tensile stresses.
4. Bond/seal maintenance risk assessment: Absolute low risk of bond/seal failure.
Summary: 1) Generally indicated for anterior teeth; 2) Occasional bicuspid use and rare molar use would be acceptable only with all parameters at the least-risk level. Category 1 materials are ideal in cases with significant enamel on the tooth and generally with low flexure and stress risk assessment. These materials absolutely require long-term bond maintenance for success.
Category 2: Glass-Based Pressed or Machinable Materials
Glass-ceramic pressable materials, such as IPS Empress® (Ivoclar Vivadent, www.ivoclarvivadent.us) and Authentic® (Jensen Dental), and the higher-strength IPS e.max® (Ivoclar Vivadent) materials can be used in any of the clinical situations as Category 1 materials. Machinable versions of glass-ceramic material, such as Vitablocs Mark II® (Vident, www.vident.com), IPS Empress CAD, and IPS e.max CAD, can be used interchangeably with the pressed versions. Monolithic IPS e.max, due to its high strength and fracture toughness, has shown promise as a full-contour, full-crown alternative, even on molars.14 Glass-ceramics can also be used in clinical situations when higher risk factors are involved. Other than certain risk factors (see below) that would limit their use, these materials can be difficult to use when there is less than 0.8 mm in thickness, except at marginal areas. They can gradually thin to a margin of approximately 0.3 mm. All things being equal, if the restoration is still a Category 1 clinical situation and there is more than 0.8 mm of working space, glass-ceramics should be considered due to their increased strength and toughness, as well as the presence of sufficient room to achieve the desired esthetics.
Esthetic Factors
Space requirements for workability and shade change: 0.8 mm of minimum working thickness and 0.2 mm to 0.3 mm for each shade change.
Environmental Factors
1. Substrate condition: Less than 50% of the enamel is on the tooth, less than 50% of the bonded substrate is in the enamel, and 30% or more of the margin is in the dentin.
2. Flexure risk assessment: Medium for Empress, Vitablocs Mark II, and Authentic-type glass-ceramics or layered IPS e.max. In cases in which flexure risk assessment is medium to high (and full-crown preparation is not desirable), the authors have found in their clinical trials that monolithic IPS e.max has been 100% successful for as long as 30 months in service. All glass-ceramic restorations, including IPS e.max, were adhesively bonded in their samples.
3. Tensile and shear stress risk assessment: Medium for Empress, Vitablocs Mark II, and Authentic-type glass ceramics or layered IPS e.max. Medium to medium/high for bonded monolithic IPS e.max.
4. Bond/seal maintenance risk assessment: Low risk of bond/seal failure for Empress, Vitablocs Mark II, and Authentic type glass-ceramics or layered IPS e.max. Medium for monolithic IPS e.max.
Summary: Pressed or machined glass-ceramic material such as Empress, Vitablocs Mark II, and Authentic are indicated for thicker veneers, anterior crowns, and posterior inlays and onlays (Figure 7 and Figure 8) in which medium or lower flexure risks and shear and tensile stress risks are documented (Figure 9 and Figure 10). Also, they are indicated only in clinical situations in which long-term bond seal can be maintained. IPS e.max (Figure 11 and Figure 12), which is a different type of glass-ceramic that has higher toughness, is also indicated for the same clinical situations as the other glass-ceramics but can be extended for single-tooth use in higher-stress situations (as in molar crowns). This is provided it is used in a full-contour monolithic form and cemented with a resin cement.
Category 3: High-Strength Crystalline Ceramics
Mostly all-crystalline materials (eg, In-Ceram®, Vita) are used for core systems to replace metal that would then be veneered with porcelain. Alumina-based systems, eg, In-Ceram, Procera® (Nobel Biocare, www.nobelbiocare.com), were first on the market but are now generally being replaced with zirconia systems. Alumina systems have been shown to be very clinically successful for single units, with a slightly increased risk in the molar region.15,16 They can be recommended for any single-unit anterior or bicuspid crown (Figure 13 and Figure 14). The authors have observed a slight increase in failure with conventional cements. For example, after using alumina restorations for many years at the UCLA Center for Esthetic Dentistry, the authors observed that at between 8 and 10 years, the failure rate doubled to approximately 2%, with those failures being core fractures necessitating replacement. Their suggestion for alumina core restorations is either a resin-modified, glass-ionomer luting cement (eg, Fuji PLUS™, GC America, www.gcamerica.com; RelyX™ Luting Cement, 3M ESPE, www.3mespe.com) or a resin cement. For zirconia core systems (eg, Vita YZ, Vident, www.vident.com; Procera® Zirconia, Nobel Biocare, www.nobelbiocare.com; Lava™, 3M ESPE), the authors have not experienced core fracture but have seen problems with chipping of porcelain. White and McLaren17 found that a special slow-cool thermal cycle minimizes the stress in the porcelain and porcelain/zirconia interface. Clinically, because the authors of this current article have been using the altered firing schedules, their replacement rate for chipping has been reduced by less than 1%.
Esthetic Factors
Space requirements for workability and maximum esthetics: 1.2-mm minimum working thickness and 1.5 mm ideal if masking.
Environmental Factors
1. Substrate condition: Substrate is not critical because the high-strength core supports the veneering material.
2. Flexure risk assessment: High or below. For high-risk situations, the core design and structural support for porcelain become more critical.
3. Tensile and shear stress risk assessment: High or below. Note: For high-risk situations, the core design and structural support for porcelain become more critical. Preparations should allow for a 0.5-mm core plus 1 mm of porcelain to ensure the best esthetic results. There should not be more than 2 mm of unsupported occlusal or incisal porcelain; the restoration core should be built out to support marginal ridges. For higher-risk molar regions, it is more ideal to use zirconia cores vs. alumina cores, provided the current firing parameters are followed. Full-contour zirconia restorations (eg, Prettau Zirconia, Zirkozahn, www.zirkonzahn.com; BruxZir®, Glidewell Laboratories, www.glidewelldental.com) have been recommended for high-risk molar situations. Failure would not be an issue; some preliminary concern involves wear of the opposing dentition with full-contour zirconia.18 No clinical data could be found to confirm or refute this. Clinically, only full-contour zirconia against full-contour zirconia in the molar region should be considered when no other clinical option is viable.
4. Bond/seal maintenance risk assessment: If the risk of obtaining or losing the bond or seal is high, then zirconia is the ideal all-ceramic to use.
Summary: High-strength ceramics (specifically zirconia) is indicated when significant tooth structure is missing, an unfavorable risk for flexure and stress distribution is present, and it is impossible to obtain and maintain the bond and seal (eg, most posterior full-crown situations with subgingival margins) (Figure 15 and Figure 16).
Category 4: Metal-Ceramics
For almost half a century, metal-ceramics have been the standard for esthetic full-crown restorations. Generally, they have the same indications as Category 3 zirconia-based restorations. With metal-ceramics, manufacturers have eliminated the complications throughout the years; these materials do not have the same thermal firing sensitivity as zirconia does. However, anterior teeth metal-ceramics need to be approximately 0.3 mm thicker to have the same esthetics as properly designed zirconia/porcelain crowns.
Esthetic Factors
1. Work space requirements: 1.5 mm to 1.7 mm for maximum esthetics.
2. Substrate condition: The substrate is not as critical because a metal core supports the veneering material.
3. Flexure risk assessment: High or below. For high-risk situations, the core design and structural support for porcelain become more critical.
4. Tensile and shear stress risk assessment: High or below. For high-risk situations, the core design and structural support for porcelain become more critical.
5. Bond/seal maintenance risk assessment: If the risk of obtaining or losing the bond or seal is high, then metal ceramics are an ideal choice for a full-crown restoration.
Summary: Metal-ceramics are indicated in all full-crown situations, especially when all risk factors are high (Figure 17).
Conclusion
This article presented a systematic process of clinical evaluation and rationale for material selection. The most important point is the most conservative restoration should be done if the clinical criteria are met, eg, a full-coverage crown or deep-cut glass-ceramic restoration should not be performed when a more conservative Category 1 porcelain restoration is indicated.
References
1. Land CH. Porcelain dental art. Dent Cosmos. 1903;65:615-620.
2. Della Bona, Kelly JR. The clinical success of all-ceramic restorations. J Am Dent Assoc. 2008;139(suppl);8S-13S.
3. McLaren EA, Cao PT. Ceramics in dentistry—part I: classes of materials. Inside Dentistry. 2009:5(9)94-103.
4. Sadowsky SJ. An overview of treatment considerations for esthetic restorations: a review of the literature. J Prosthet Dent. 2006;96(6):433-442.
5. Strassler HE. Minimally invasive porcelain veneers: indications for a conservative esthetic dentistry treatment modality. Gen Dent. 2007;55(7):686-712.
6. Giordano R. A comparison of all-ceramic systems. J Mass Dent Soc. 2002;50(4):16-20.
7. McLaren EA, Cao PT. Smile analysis and esthetic design: "in the zone." Inside Dentistry. 2009;5(7):44-48.
8. Chiche G, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Publishing. 1994:13-32.
9. Hondrum SO. A review of the strength properties of dental ceramics. J Prosthet Dent. 1992;67(6):859-865.
10. Shoher I, Whiteman A. Reinforced porcelain system: a new concept in ceramometal restorations. J Prosthet Dent. 1983;50(4):489-496.
11. Malament KA. Considerations in posterior glass-ceramic restorations. Int J Periodontics Restorative Dent. 1988;8(4):32-49.
12. Malament KA, Socransky SS, Thompson V, et al. Survival of glass-ceramic materials and involved clinical risk: variables affecting long-term survival. Pract Proced Aesthet Dent. 2003(suppl):5-11.
13. Friedman MJ. A 15-year review of porcelain veneer failure—a clinician's observations. Compend Contin Educ Dent. 1998;19(6):625-638.
14. Fasbinder DJ, Dennison JB, Heys D, et al. A clinical evaluation of chairside lithium disilicate CAD/CAM crowns: a two-year report. J Am Dent Assoc. 2010;141(suppl 2):10S-14S.
15. Odman P, Andersson B. Procera All-Ceram crowns followed for 5 to 10.5 years: a prospective clinical study. Int J Prosthodont. 2001;14(6):504-509.
16. McLaren EA, White SN. Survival of In-Ceram crowns in a private practice: a prospective clinical trial. J Prosthet Dent. 2000;83(2):216-222.
17. White SN, McLaren EA. 3M Expertise Scientific Facts. June 2009. Data on file with 3M.
18. Ghuman T, Beck P, Ramp LC, et al. Wear of enamel antagonist to ceramic surfaces. J Dent Res. 2010;89(spec iss B):1394.
About the Authors
Edward A. McLaren, DDS, MDC
Professor, Founder, and Director
UCLA Post Graduate Esthetics
Director
UCLA Center for Esthetic Dentistry
Los Angeles, California
Yair Y. Whiteman, DMD
Faculty Member
UCLA Post Graduate Esthetics
UCLA Center for Esthetic Dentistry
Los Angeles, California