You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In restorative dentistry, there are defined clinical criteria for the evaluation of direct and indirect restorations.1 When evaluating restorations, one significant challenge that a clinician faces is the assessment of the acceptability of a restoration. If a restoration is unacceptable, then a decision must be made to either replace or repair that restoration. Considering that the hard-tissue examination must also include diagnosing primary, pit-and-fissure, and interproximal caries, the task for treatment planning restorative interventions can be very daunting.
There has been an increase in occlusal pit-and-fissure caries with a concomitant change in its pattern and progression.2-4 The diagnosis of pit-and-fissure occlusal lesions has become more difficult. This difficulty has led to an increase in research and development for better diagnostic tools for pit-and-fissure caries detection.5-7 In these articles there has been a consensus that optimal technique should have good diagnostic performance, be non-invasive, allow for a quantification of disease progression and objective monitoring, and be easy to carry out at reasonable costs.8 While the correct recognition of sound and cavitated surfaces is typically not a problem, non-cavitated lesions create a significant challenge. In recent years digital devices have been introduced as an adjunct to the clinical examination to diagnose pit-and-fissure caries.9
The diagnosis of smooth-surface interproximal carious lesions is also a clinical challenge. In the anterior region, the diagnosis can be made with a combination of visual assessment and radiography. In the posterior region, in most cases, a diagnosis of caries lesions can only be made using radiography. With radiographs, it is important that the images are of higher density (darker). Also, radiographs are better at providing diagnostic information for dentin lesions, not enamel lesions.10-12 With digital radiography, many manufacturers provide software enhancements to change the contrast and density of the image, and these changes allow for improved diagnostic decisions.13,14
When deciding to replace or repair existing restorations, there is difficulty in achieving consensus among practitioners. Bader and Shugars analyzed the extent of agreement to recommended treatment among dentists for 1,187 teeth in 43 patients.15 For at least six general practitioners examining, the "inter-dentist" reliability in recommending individual teeth for treatment was moderate. Reliability for treatment recommendations for unrestored teeth with no clinically evident caries was only fair. Surprisingly, reliability was lowest among these general practitioners when there was an existing restoration in a tooth. A detailed analysis revealed that for all teeth receiving at least one recommendation for treatment, only 22% received a unanimous recommendation. These and other significant variations in decision-making trends for treatment have been well described in the dental literature.16-18
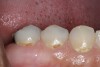
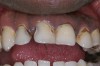
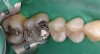
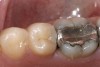
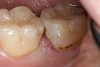
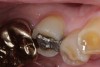
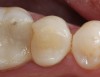
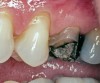
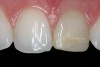
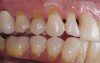
Replacement of existing restorations is responsible for 75% of all operative dentistry.15,19 The reasons for placement and replacement of restorations of direct restorative materials include: primary caries (Figure 1 and Figure 2); recurrent caries (Figure 3); poor margins (Figure 4 and Figure 5); restoration fracture (Figure 6 and Figure 7); tooth fracture (Figure 8); esthetics (Figure 9); non-carious tooth structure lost (attrition, abrasion, abfraction, erosion) (Figure 10); and pain/sensitivity.
Early evaluations of the need for replacement of direct restorative materials surveyed clinicians in private practice for the reasons for replacement of existing restorations.19 In 1981, Mjor reported on a survey of 87 private practitioners. Of the 5,487 restorations these clinicians placed, 74% were amalgam and 26% were composite resin, with 71% of the amalgam and 79% of the composite resin being replacement restorations. The reasons for amalgam replacement were secondary caries (61%); poor marginal adaptation (9%); isthmus fracture (12%); fracture of the tooth (7%); and other reasons (7%). For the composite resin group, replacements were due to secondary caries (20%); restoration discoloration (12%); poor anatomic form (40%); discolored margins (8%); and other reasons (20%). At the time of this survey, the routine use of adhesive composite resin restorations was still in its infancy, having been introduced in the early- to mid- 1970s.
Mjor updated this survey in 1997,20 with reports from 22 clinicians surveying 2,379 restorations to include amalgam (45%), composite resin (37%), and glass ionomer (18%). The data summarized the numbers of restorations placed due to primary caries, non-carious tooth structure loss, tooth fracture, or replacement restorations. For amalgam, restoration placement was due to primary caries (33%); non-carious tooth structure loss (2%); and replacement of failed restorations (65%). For composite resin, the reasons for placement were due to primary caries (18%); non-carious tooth structure loss (22%); and replacement of failed restorations (60%). For glass ionomer, restoration placement was due to primary caries (22%); non-carious tooth structure loss (12%); and restoration replacement (66%). The ratio of initial restorations placed due to primary caries to restoration replacement was 1:1.4, meaning that approximately 60% of restorations placed were replacement restorations. For amalgam restorations, the reasons for replacement included secondary caries (43%); poor margins (15%); isthmus/bulk fracture (19%); tooth fracture (11%); pain/sensitivity (5%); unsightliness (1%); and other reasons (6%). For composite resin, the reasons for replacement were due to secondary caries (26%); poor margins (19%); bulk fracture (4%); tooth fracture (14%); pain/sensitivity (4%); unsightliness (26%); and other reasons (6%). For glass ionomer, reasons for replacement included secondary caries (26%); poor margins (16%); bulk fracture (9%); tooth fracture (15%); pain/sensitivity (10%); unsightliness (8%); and other reasons (16%). Of interest in this data set is that even though glass ionomer has fluoride release, secondary caries does occur at restoration margins but may take a longer period of time when compared to composite resin. In both surveys, the most frequent reason for restoration replacement was secondary caries.
In evaluating the reasons for replacement of amalgam, composite resin, and glass ionomer and then deciding on what restorative material should be used to replace the existing restoration or place an initial restoration, the longevity of the restoration being placed is important when determining appropriate treatment. As new technologies and materials evolve, predicting the longevity of restorations may be impossible. In a survey of dentists' estimates of longevity in 1986, clinicians reported that small amalgam restorations lasted 11 years, large amalgam restorations lasted 6 years, and cast restorations lasted 13 years.21 When asked why restorations failed, responsibility was placed upon the patient (37%); the dentist (30%); and the restorative material (23%). A more recent survey evaluated Class I and Class II amalgam and composite resin restorations by two practitioners,22 and found that survival rates for posterior composite at 5 years was 91.7% and at 10 years was 82.2%. For amalgam, the survival was 89.6% at 5 years and 79.2% at 10 years. Other reports provide similar results.23,24
Diagnosis for Restoration Replacement
Among the criteria for restoration replacement are those diagnoses that are obvious from clinical examination and patient history, but there are criteria that are not as clearly defined, such as: restoration replacement due to frank caries visible at restoration margins (secondary caries); a fractured restoration; a fractured tooth adjacent to an existing restoration; restoration discoloration that is esthetically unacceptable to the patient; pain/sensitivity; and significant noncarious loss of tooth structure that changes the contour and function of the tooth. Secondary caries can be more difficult to diagnose.
Secondary caries is the most prevalent diagnosis for replacing restorations.19,20,25-29,30 Secondary caries is difficult to diagnose, and clinicians are often inaccurate and inconsistent in this diagnosis resulting in the unnecessary replacement of satisfactory restorations.31,32 Practitioners, when surveyed, indicated that defective margins are a frequent criteria for restoration replacement.19,33,34 The presence of ditched amalgam margins as a predictor for recurrent caries has been controversial.35-38 This controversy revolves around the challenges of making a visual assessment of an amalgam restoration's decline.39-41 There has been concern that marginal defects and replacement of restorations due to these defects do not correlate well with the actual presence of secondary caries, and that clinical treatment be deferred until caries is present clinically or radiographically.36,37,42 Hewlett and coworkers investigated radiographic secondary caries prevalence in teeth with clinically defective restorations.43 They found that the likelihood of radiographic secondary caries was three times higher for defective restorations than for intact restorations. The large number of defective restorations (86%) with no radiographic evidence of secondary caries suggests that using current, diagnostic radiographs combined with restoration status can reduce the risk of overtreatment.
What is the relationship between marginal ditching and staining as a predictor of secondary caries for amalgam restorations? Kidd and coworkers investigated the relationship between marginal ditching and secondary caries as a predictor for secondary caries adjacent to amalgam restorations by microbiologic assessment.44 Their findings were very clear. For amalgam restorations there were no significant differences of clinical caries beneath intact restorations and restorations with narrow ditches (less than 0.4 mm). The color of the enamel was irrelevant to the level of infection of the dentin beneath the margins of the restoration as long as a frankly carious lesion was not present. The results suggest that amalgam restorations with ditched margins greater than 0.4 mm or frank carious lesions need to be replaced. The presence of narrow ditched margins and color change should not trigger restoration replacement.
Prediction of secondary caries with composite resin and glass ionomer can also be a challenge. When the marginal staining and discoloration of tooth-colored restorations create an unsightly appearance that is bothersome to the patient, the rationale for replacement of that restoration is obvious. The diagnosis of secondary caries for tooth-colored restorations in the presence of marginal staining and ditching is not conclusive.45,46 When frank caries is present at a restoration margin the restoration should be replaced or repaired, but does a line of stain or discoloration seen through the translucent restoration or enamel clearly define secondary caries? In a laboratory study using 112 extracted teeth that had previously placed amalgam and composite restorations in 331 sites that had either intact margins, ditched margins, or stained margins, radiographic and clinical evidence of secondary caries was evaluated.46 There was no difference in the data between amalgam and composite resin, so the data was combined. The restorations were removed and the dentin at the dentin–enamel junction (DEF) was evaluated for its consistency (hard/soft) and color (stained/stain-free). The results demonstrated that staining around a restoration is not a reliable predictor of softening or discoloration on the dentin. Ditched margins were also not a clear indication. The only triggers for restoration replacement due to secondary caries were the presence of frank caries or radiographic evidence of caries. Kidd and Beighton investigated the prediction of secondary caries adjacent to tooth-colored restorations with a clinical and microbiologic assessment.47 An evaluation of 113 teeth with 197 visible sites were clinically examined and the plaque and dentin cultured. Only 38 of the 167 sites without frank carious dentin had soft dentin at the DEJ. The conclusion of this study was that there are no good clinical criteria to predict the presence of soft dentin other than the presence of frank caries at the restoration margin.
Repair or Replacement of Defective Restorations
There is a limited longevity for restorations. A significant part of dental practice is the replacement of defective restorations.48,49 When a restoration is defective, the recommendation has traditionally been to replace the entire restoration.48,50 In recent years, the concept of minimally invasive restorative dentistry has generated investigations of the sealing, repair, and refurbishing of existing restorations instead of entire restoration replacement.50-56 The rationale for restoration repair is that minimal intervention with a repair conserves existing tooth structure and places the dental pulp at less risk through less traumatic tooth preparations.57-59 Also, repairing a restoration has the potential of needing less treatment time, can sometimes be performed without the need for local anesthesia, and as a result can be less stressful to the patient.50 Whenever an existing restoration is replaced, the removal of the restoration also includes the removal of additional tooth structure, enlarging the preparation.
Research studies investigating the sealing, repair, and refurbishing of defective restorations have been very promising at improving the longevity of existing restorations. A 7-year study of 113 defective amalgam restorations where localized defects were sealed, repaired, refinished, replaced, or not treated evaluated the outcomes of treatment decisions.54 Sealing a defective "ditched" margin was accomplished using an etch-and-rinse light-cured resin sealant. Repairs of defective sites were done using a carbide bur removing the amalgam from the defective site, evaluating the defect to remove caries or defective tooth structure, and restoring with amalgam. Refinishing with a finishing bur treated defective marginal areas that contained amalgam excesses. The margin was then polished with a rubber point. For the replacement and no treatment groups, treatment was randomly assigned for defective restorations that could not be markedly improved with any of the other treatment options. For replacement restorations, the clinicians removed the defective restoration, finalized the cavity preparation, and restored with amalgam using no bonding agent or liner. At each recall period restorations were evaluated using the modified USPHS criteria60: occlusal margin adaptation; proximal marginal adaptation; anatomic form (occlusal); anatomic form (proximal); occlusal contact; proximal contact; secondary caries; and postoperative sensitivity. At the 7-year recall, the conclusion of this study was that repair rather than replacement of amalgam restorations with localized defects was an acceptable treatment option.
Evaluation of defective composite resin restorations provide different challenges for decision making to repair or replace.45-47 Gordan and coworkers investigated repair versus replacement of composite-resin restorations over a 7-year clinical evaluation.56 Composite-resin restorations that were defective were assigned groups for no treatment, marginal sealing, resurfacing, replacement, or repair. The repair, sealant, and replacement groups showed the best results when compared to the no-treatment group for marginal adaptation. For restorations that had marginal staining, repair and replacement demonstrated superior results. Over the 7 years of evaluation, restorations demonstrated degradation in all of the evaluated criteria and restoration survival differed among treatment approaches. Non-replacement treatment strategies for composite restorations can be successful. Other studies evaluating repair versus replacement for localized defects of amalgam and composite-resin restorations have shown similar conclusions.51,53,55
Conclusion
The diagnostic decision to repair or replace defective restorations is controversial for many practitioners. To make this decision, the clinician must have a clear understanding of the objective criteria that determines a defective restoration. Restorations are replaced due to primary and recurrent caries; poor margins; bulk fracture; tooth fracture; poor esthetics; tooth structure loss due to attrition, abrasion, abfraction, and/or erosion; and tooth pain/sensitivity.
When the decision is made to intervene restoratively, the evidence supports consideration for localized marginal defects to repair rather than replace the entire restoration. Restoration repair conserves tooth structure, puts the pulp at less risk, and will provide a treatment outcome that can be as successful as total restoration replacement.
References
1. Hickel R, Peschke A, Tyas M, et al. FDI World Dental Federation clinical criteria for the evaluation of direct and indirect restorations. Update and clinical examples. J Adhes Dent. 2010;12(4):259-274.
2. Weerheijm KL, Gruythuysen RJM, can Amerongen WE. Prevalence of hidden caries. ASDC J Dent Child. 1992;59(6):408-412.
3. Haugejorden O, Tveit AB. The effect of fluoridation on the occurrence of hidden caries in clinically sound occlusal surfaces. Caries Res. 1998;32(4):266.
4. Ricketts D, Kidd E, Weerheijm K, de Soet H. Hidden caries: what is it? Does it exist? Does it matter? Int Dent J. 1997;47(5):259-265.
5. Wenzel A, Larsen MJ, Ferjerskov O. Detection of occlusal caries without cavitation by visual inspection, film radiographs, xeroradiographs, and digitized radiographs. Caries Res. 1991;25(5):365-371.
6. Verdonschot EH, Wenzel A, Bronkhorst EM. Assessment of diagnostic accuracy in caries detection: an analysis of two methods. Community Dent Oral Epidemiol. 1993;21(4):
203-208.
7. Pitts NB. Clinical diagnosis of dental caries: a European perspective. J Dent Educ. 2001;65(10):972-978.
8. Kühnisch J, Heinrick-Weltzien R, Tabatabaie M, et al. An in vitro comparison between two methods of electrical resistance measurement for occlusal caries detection. Caries Res. 2006;40(2):104-111.
9. Strassler HE, Sensi LG. Technology-enhanced caries detection and diagnosis. Compend Contin Educ Dent. 2008;29(8):464-470.
10. Rocha RO, Ardenghi TM, Oliveira LB, et al. In vivo effectiveness of laser fluorescence compared to visual inspection and radiology for detection of occlusal caries in primary teeth. Caries Res. 2003;37(6):437-441.
11. Lussi A. Comparison of different methods for the diagnosis of fissure caries without cavitation. Caries Res. 1993;27(5):409-416.
12. Ricketts DN, Kidd EA, Beighton D. Operative and microbiological validation of visual, radiographic and electronic diagnosis of occlusal caries in non-cavitated teeth judged to be in need of operative care. Br Dent J. 1995;179(6):214-220.
13. Wenzel A, Fejerskov O, Kidd E, et al. Depth of occlusal caries assessed clinically by conventional film radiographs and by digitized processed radiographs. Caries Res. 1990;24(5):327-333.
14. Li G, Yahuira K, Welander U, et al. Detection of approximal caries in digital radiographs before and after correction for attenuation and visual response: an in vitro study. Dentomaxillofacial Radiol. 2002;31(2):113-116.
15. Bader JD, Shugars DA. Agreement among dentists' recommendations for restorative treatment. J Dent Res. 1993;72(5):891-896.
16. Bailit HL, Clive J. The development of dental practice profiles. Med Care. 1981;19(1):30-46.
17. Bailit H, Chiriboga D, Grasso J, et al. A new intermediate dental outcome measure. Med Care. 1979;17:780-786.
18. Grembowski D, Milfrom P, Fiset L. Clinical decision making among dental students and general practitioners. J Dent Educ. 1989;53:189-192.
19. Mjör I. Placement and replacement of restorations. Oper Dent. 1981;6:49-54.
20. Wilson JHF, Burke FJT, Mjör IA. Reasons for placement and replacement of restorations of direct restorative materials by a selected group of practitioners in the United Kingdom. Quintessence Int. 1997;28:245-248.
21. Maryniuk GA, Kaplan SH. Longevity of restorations: survey results of dentists' estimates and attitudes. J Am Dent Assoc. 1986;112:39-45.
22. Opdam NJ, Bronkhorst EM, Roeters JM, Loomans BA. A retrospective clinical study on longevity of posterior composite and amalgam restorations. Dent Mater. 2007;23:2-8.
23. De Rosa Rodolpho PA, Cenci MS, Donassollo TA, et al. A clinical evaluation of posterior composite restorations: 17 year findings. J Dent. 2006;34:427-435.
24. Osborne JW, Norman RD, Gale EN. A 14-year clinical assessment of 12 amalgam alloys. Quintessence Int. 1991;22:857-864.
25. Allander L, Birkhed D, Bratthall D. Reasons for replacement of Class II amalgam restoration in private practice. Swed Dent J. 1990;14:179-184.
26. Kidd EAM, Toffenetti F, Mjör IA. Secondary caries. Int Dent J. 1992;42:127-138.
27. Deligeorgi V, Mjör IA, Wilson NH. An overview of reasons for the placement and replacement of restorations. Prim Dent Care. 2001;8(1):5-11.
28. Burke FJ, Cheung SW, Mjör IA, Wilson NH. Restoration longevity and analysis of reasons for the placement and replacement of restorations provided by vocational dental practitioners and their trainers in the United Kingdom. Quintessence Int. 1999;30:234-242.
29. Nascimento MM, Gordan VV, Qvist V, et al. Reasons for placement of restorations on previously unrestored tooth surfaces by dentists in the Dental Practice Based Research Network. J Am Dent Assoc. 2010;141:441-448.
30. Mjör IA, Moorhead JE, Dahl JE. Reasons for replacement of restorations in permanent teeth in general dental practice. Int Dent J. 2000;50:361-366.
31. Merrett MCW, Elderton RJ. An in vitro study of restorative dental treatment decisions and dental caries. Br Dent J. 1984;157:128-133.
32. Mjör IA. Clinical diagnosis of recurrent caries. J Am Dent Assoc. 2005;136:1426-1433.
33. Qvist V, Thylstrup A, Mjör IA. Restorative treatment pattern and longevity of amalgam restorations in Denmark. Acta Odontol Scand. 1986;44:343-349.
34. Boyd MA, Richardson AS. Frequency of amalgam replacement in a general dental practice. J Can Dent Assoc. 1985;51:763-766.
35. Jorgensen KD, Wakumoto S. Occlusal amalgam fillings: marginal defects and secondary caries. Odontol Tidskr. 1968;76(1):43-54.
36. Kidd EAM, O'Hara JW. The caries status of occlusal restoration amalgam restorations with marginal defects. J Dent Res. 1990;69(6):1275-1277.
37. Letzel H, van't Hof MA, Vrijhoef MMA, et al. Failure, survival, and reasons for replacement of amalgam restorations. In: Anusavice KJ, ed. Quality Evaluation of Dental Restorations. Chicago, IL: Quintessence Publishing Co. 1989;83-92.
38. Ermis RB, Aydin U. Examiner agreement in the replacement decision of Class I amalgam restorations. J Contemp Dent Pract. 2004;5(2):81-92.
39. Jokstad A, Mjör IA. Assessment of marginal degradation of restorations on impressions. Acta Odontol Scand. 1991;49(1):15-25.
40. Bryant RW, Mahler DB, Engel JH. A comparison of methods for evaluating marginal fracture of amalgam restorations. Dent Mater. 1985;1(6):235-237.
41. Woods PW, Marker VA, Mckinney TW, et al. Determining amalgam marginal quality: effect of occlusal surface condition. J Am Dent Assoc. 1993;124(5):60-65.
42. Espelid I, Twiet AB. Diagnosis of secondary caries and crevices adjacent to amalgam. Int Dent J. 1991;41(6):359-364.
43. Hewlett ER, Atchison KA, White SC, Flack V. Radiographic secondary caries prevalence in teeth with clinically defective restorations. J Dent Res. 1993;72:1604-1608.
44. Kidd EAM, Joyston-Bechal S, Beighton D. Marginal ditching and staining as a predictor of secondary caries around amalgam restorations: a clinical and microbiological study. J Dent Res. 1995;74:1206-1211.
45. Qvist V, Qvist J, Mjör IA. Placement and longevity of tooth-colored restorations in Denmark. Acta Odontol Scand. 1990;48:305-311.
46. Kidd EAM, Joyston-Bechal S, Beighton D. Diagnosis of secondary caries: a laboratory study. Br Dent J. 1994;176(4):135-139.
47. Kidd EAM, Beighton D. Prediction of secondary caries around tooth-colored restorations: a clinical and microbiology study. J Dent Res. 1996;75:1942-1946.
48. Going RE, Jendresen MD. Failures related to materials used in restorative dentistry. Dent Clin North Am. 1972;16(1):71-86.
49. Deligeorgi V, Mjör IA, Wilson NH. An overview of reasons for the placement and replacement of restorations. Prim Dent Care. 2001;8(1):5-11.
50. Sharif MO, Merry A, Catleugh M, et al. Replacement versus repair of defective restorations in adults: amalgam. Cochrane Database Syst Rev. Feb 17, 2010; DOI: 10.1002/14651858.CD005970.pub2.
51. Moncada G, Martin J, Fernandez E, et al. Sealing, refurbishing and repair of Class I and Class II defective restorations: a three-year clinical trial. J Am Dent Assoc. 2009;140(4):425-432.
52. Setcos JC, Khosravi R, Wilson NH, et al. Repair or replacement of amalgam restorations: decisions at a USA and a UK dental school. Oper Dent. 2004;29(4):392-397.
53. Fernandez EM, Martin JA, Angel PA, et al. Survival rate of sealed, refurbished and repaired defective restorations: 4-year follow-up. Braz Dent J. 2011;22(2):134-139.
54. Gordan VV, Riley JL 3rd, Blaser PK, et al. Alternative treatments to replacement of defective amalgam restorations: results of a seven-year clinical study. J Am Dent Assoc. 2011;142(7):842-849.
55. Moncada G, Fernandez E, Martin J, et al. Increasing longevity of restorations by minimal intervention: a two-year clinical trial. Oper Dent. 2008;33(3):258-264.
56. Gordan VV, Garvan CW, Blaser PK, et al. A long-term evaluation of alternative treatments to replacement of resin-based composite restorations: results of a seven-year study. J Am Dent Assoc. 2009;140:1476-1484.
57. Gordan VV. In vitro evaluation of margins of replaced resin-based composite restorations. J Esthet Dent. 2000;12(4):209-215.
58. Gordan VV. Clinical evaluation of Class V resin-based composite restorations. J Dent. 2001;29(7):495-498.
59. Brantley CR, Bader JD, Shugars DA, Newbit SP. Does the cycle of re-restoration lead to larger restorations. J Am Dent Assoc. 1995;126:1407-1413.
60. Cvar JF, Ryge G. Criteria for the clinical evaluation of dental restorative materials. San Francisco: U.S. Department of Health, Education, and Welfare, Public Health Service, National Institutes of Health, Bureau of Health Manpower Education, Division of Dental Health, Dental Health Center; 1971. U.S. Public Health Service Publication 790-244.
About the Author
Howard E. Strassler, DMD
Professor, Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland