You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Acquired environmental loss of tooth structure is often multifactorial.1 Traditionally, the terms erosion, abrasion, and attrition have been used to describe the noncarious, pathological loss of tooth tissue. The differential diagnosis of tooth wear2 is crucial and governs the spectrum of options that can be offered to restore the worn teeth to correct form and function. This article emphasizes the pathophysiology of tooth surface loss (TSL) due to gastroesophageal reflux and a modified minimalistic treatment approach.
Tooth Erosion
Erosion is a physical mechanism causing wear by friction from the movement of liquids. Tooth erosion is described as TSL produced by chemical or electrolytic processes of nonbacterial origin, which usually involves acids. In recent literature, the term biocorrosion has been substituted for the term erosion because it encompasses the chemical, biochemical, or electrochemical action that causes the molecular degradation of the essential properties in a living tissue.1
The source of acids may be endogenous—that is, they arrive in the oral cavity due to refluxed gastric juices either invited voluntarily (eg, self-induced vomiting from bulimia) or as a result of gastroesophageal reflux disease (GERD)—and/or exogenous—those whose sources are dietary, medicinal, occupational, or recreational.
GERD
Gastroesophageal reflux disorder is a chronic condition—often called heartburn—which is caused by stomach acid regurgitating into the esophagus or oral cavity. The American Gastroenterological Association has published the Montreal consensus,3 which defined GERD as “a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications;” its manifestations have been subclassified into esophageal and extraesophageal syndromes. The prevalence of dental erosion in adult GERD patients has been documented to be around 25%.4 Various factors—including consumption of alcohol and caffeine; the existence of medical conditions such as obesity, pregnancy, and sleep apnea; and the use of drugs like NSAIDs—are risk factors for GERD.5
Dental Manifestations of GERD
The oral manifestations may include tooth erosion, sensitivity, sour taste, halitosis, and mucositis.5 Dissolution of enamel begins when the pH drops below 5.2. The pH value of gastric acid is found to be around 2.0.6
Dental healthcare professionals are in a position to be the first to diagnose GERD or biocorrosion due to acids. For this reason, they need to look for the signs because most patients are “silent refluxers.” The typical dental manifestations of erosion from intrinsic causes are listed in Table 1.
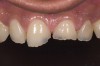
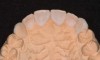
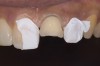
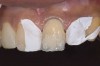
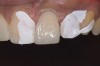
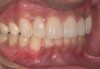
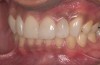
Acid dissolves the palatal enamel of upper anteriors, thus exposing the underlying dentin. This makes teeth appear higher in chroma and leads to hypersensitivity as well as supraeruption of opposing incisors. Clinically, this restricts the space needed to restore lost palatal tooth structure (Figure 1 and Figure 2).
Restorative options that help regain the lost space and lost palatal form without compromising the vitality of the anterior tooth are a priority. Methods of gaining space to restore lost palatal form may include the following options—each of which has advantages and disadvantages depending on the severity of TSL and number of teeth affected.
Excessive tooth preparations including elective endodontics.
Orthodontic repositioning of anterior teeth followed by palatal veneers.
Enameloplasty of opposing teeth.
Opening the occlusal vertical dimension (OVD) and restoring posterior occlusal surfaces and palatal surfaces of anteriors.
Harmonizing maximum intercuspation (MIP) with centric relation (CR).8
Palatal veneers using a modification of Dahl’s9 principle (Figure 3).
The traditional approach would require the clinician to sacrifice the vitality of the upper anterior teeth and consider intraradicular support to make full-coverage restorations. This treatment leads to excessive thinning and weakening of the anterior tooth, leading to increased flexibility,10 thereby putting the tooth at a high biomechanical risk and compromising its longevity. There is also an imminent danger of recurrent decay due to continued dissolution of tooth structure at the margins of the full-coverage restorations. It is important to emphasize that even conservative adhesive restorations would be susceptible to the risk of secondary decay to the same extent as full-coverage restorations; however, when it happens in the full-coverage restoration, it may be the end of the road for these teeth. With conservative adhesive restorations, there may still remain a chance of converting to full-coverage restorations at a later time. Orthodontic repositioning is ideal and conservative, but time constraints and economic considerations may negate their use in all cases. Enameloplasty of opposing teeth with patients’ consent can provide some additional space, but it may lead to hypersentivity.
In severe generalized TSL due to erosion involving anterior and posterior teeth, it may be prudent to restore the lost vertical dimension by opening the bite to employ additive restorative modalities. This, combined with harmonizing the MIP with CR, provides the crucial few millimeters required to restore lost form without aggressive tooth preparation.10
The greatest challenge exists in management of localized TSL on the palatal surfaces of the upper anteriors with little or no TSL on posteriors. The option of palatal veneers using a modified Dahl’s9 principle is conservative and advocated in such cases when possible.
Case Presentation
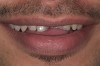
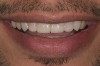
A 20-year-old male patient presented with irregular upper anterior teeth and was unhappy with his smile (Figure 4). He complained of occasional generalized mild sensitivity. Dental treatment history revealed that he had occasional dental work done in the past. Two weeks previously, he had severe pain in tooth No. 10, which was treated endodontically, and he was then referred to the author’s practice for management of anterior wear. Tooth No. 3 had a broken amalgam restoration.
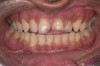
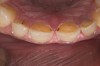
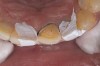
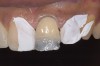
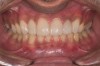
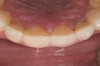
Examination revealed that palatal surfaces of teeth Nos. 6 through 11 showed severe loss of tooth structure, with mild wear on the lower incisors and loss of anterior guidance (Figure 5 through Figure 7). The palatal TSL was consistent with the clinical picture presented by patients with gastric reflux. A detailed medical history was taken, and the patient complained of having heartburn and acidity at least 4 out of 7 days a week. He had never sought treatment for it and used over-the-counter medication when needed. He was a nonsmoker, with occasional intake of alcohol. He had a high-stress job with irregular meal times. A thorough smile and dental analysis11 was carried out; the findings appear in Table 2.
Treatment Plan
The primary challenge here was to regain the lost palatal anatomy with no interocclusal space for any restorative material. Orthodontics was suggested, but refused by the patient. Performing endodontics with radicular posts, opening the VDO, and enameloplasty were not considered for reasons already mentioned above. Some of these options would biomechanically weaken the teeth.12
For this patient, a modification of the Dahl’s principle was employed whereby direct resin was used to build up the palatal anatomy of the upper anteriors and restore the lost incisal edges and labial anatomy at the same time.
Based on the patient’s age a conservative treatment plan was devised. This could be summarized as follows:
- Restoration of palatal and labial anatomy of upper anteriors with composite resin allowing disclusion of all posteriors during eccentric movements.
- Harmonizing anterior guidance.
- Restoration of all non-carious cervical lesions on cuspids and bicuspids.
- Occlusal equilibration after re-establishment of posterior occlusion by passive eruption.
Treatment Steps
Stone models were fabricated. The upper model was used to do a wax-up on the palatal/labial surfaces of anteriors (Figure 8), which established the lost form of the teeth and had a stop designed for lower incisors so that non-axial forces would be minimized.
A putty index of this wax-up was fabricated. The patient was scheduled for 3-D mock-up preview of the anterior teeth. Self-cured bis-acryl temporary resin (shade A2) was loaded in the putty index and placed on the incisors, the labial surfaces of which were spot-etched and bonded. The intraoral mock-up was finished and polished. The anterior occlusion was adjusted to have uniform contacts on all upper anteriors by restoring the palatal tooth form. The patient was allowed to evaluate the mock-up for 48 hours, after which he was scheduled for the direct resin build-up.
During the next appointment, a palatal index of the approved provisional was fabricated with putty silicone. This enabled the clinician to precisely build the lingual surfaces and incisal edges of teeth Nos. 6 through 11. The provisional mock-up resin on No. 9 was removed, and the underlying labial tooth was roughened with an abrasive diamond bur. No tooth structure was removed from the palatal surface, and unsupported enamel was rounded off from the labial. An ultrathin dry cord was placed in the gingival sulcus on No. 9 (Figure 9 and Figure 10). Teflon tape was used to isolate No. 9 from adjacent teeth. Then 37% phosphoric acid was used to totally etch the labial surface for 10 seconds and the palatal surfaces on No. 9 for 5 seconds. Single bond was applied and spread uniformly across the tooth and light-cured for 20 seconds.
White enamel shade was placed on the putty index and carried to the palatal surface of No. 9. This layer was spread uniformly and thinned out and spread along the entire width of the tooth (Figure 11). After curing this layer, A2 dentin was layered to simulate the lobular pattern seen in dentin of the natural teeth (Figure 12). After curing, a layer of transparent resin was placed in the incisal areas between the dentinal lobes. The final layer of A2 enamel was built and shaped to full contour (Figure 13). A similar build-up was done for all the remaining anterior teeth. The bite in MIP was adjusted such that there was uniform contact on all anterior teeth. The anterior guidance was harmonized to maintain uniformity in the contact of the incisors during protrusion and the canines and incisors during lateral excursions. Finishing and polishing was done per protocol (Figure 14 through Figure 18).13
The cervical erosive lesions on the cuspids and bicuspids were restored with resin-modified glass-ionomer cement. The lesions on these teeth could be due to extrinsic acids consumed in the diet combined with other factors.
The patient was recalled at frequent intervals, and after 8 months, occlusal equilibration was done to harmonize the discrepancy between MIP and CR and to have uniform, stable holding contacts on all posterior teeth and re-confirm that the anterior guidance was adequate to disclude posteriors.
Adjunctive Medical Treatment
The patient was counseled to avoid food habits that precipitate reflux. He was advised not to lie down immediately after heavy meals. To minimize gastric reflux during sleep time, patients are asked to keep their head higher than the rest of their body.
Discussion
Systematic analysis of anterior wear to fulfill patients’ esthetic and functional objectives is mandatory.14 Recent advances in composite resin technology allow the clinician to use these materials in stress-bearing areas for such cases of TSL due to acid reflux. While it may seem tempting to proceed with full-coverage restorations, it must be stressed that such restorations would require endodontic intervention and possibly intraradicular posts and weaken the tooth, thereby reducing its longevity. In cases such as these, the risk of secondary caries is high with most restorative modalities due to continued erosion of tooth structure at the margins. Clinicians need to bear in mind that usually such patients will undergo several episodes of dental treatment in their lifetime, and the most conservative approach that can meet the desired goals should be employed in each instance. Ideally, invasive treatments such as full-coverage restorations should be used after conservative options are tried and exhausted. However, in certain cases where there is severe loss on posterior tooth surfaces and resultant loss of vertical dimension of occlusion, full-coverage restorations may be the only option to restore the form, function, and beauty of the entire dentition. In 1975, Dahl9 proposed a concept of creating space in the treatment of localized anterior wear. It involved a chrome cobalt appliance with anterior bite plane, discluding the posteriors. In due course, the posteriors would erupt and the anteriors would intrude, allowing the posterior occlusion to be re-established. Over the years, various modifications of Dahl’s principle have been reported in literature.10
A simple, additive option using direct resin as presented in this case for management of localized palatal wear using the modified Dahl’s principle allowed the patient to retain his residual anterior tooth structure. Nanofilled formulations of light-cured resin were used because they have better strength, wear resistance, and optical properties as compared to hybrid composites and have shown good survival rates in high-stress situations. It needs to be emphasized that these newer formulations of composite resins, when used in such cases of significant function—even with excellent adjustment and guidance—will have surface loss at greater rates than metal or ceramic surfaces. However, in young patients, additive resin techniques allow the clinician to buy time and save crucial tooth structure so that future definitive restorative options may be exercised.
The posteriors will initially get discluded, and most patients need a couple of days to become accustomed to that. There may be transient problems with speech because of the increased VDO in some cases. The resulting interocclusal space in posterior teeth is progressively eliminated through passive eruption of the posterior teeth and slight intrusion of the anterior teeth.10 Frequent monitoring of posterior occlusion is required in these cases. Lack of posterior occlusal support may lead to the breakdown of anterior palatal composites and mobility of the anterior teeth in the long term. Wear of palatal composites may be a possibility. Even if there is severe loss of palatal composites in years to come, there is no harm done to the tooth structure, and touch-up repair treatments can be easily performed.
The medical management of these cases has to be instituted simultaneously while addressing the dental conditions. For patients who cannot get their GERD or bulimia under control, intracrevicular margins of full-coverage restorations will provide more protection against recurrent caries. However, in these cases, too, it is prudent to use this conservative approach as the first line of treatment and monitor the patient over time before committing to more aggressive restorations that require tooth preparations to meet space requirements of restorative materials.
Conclusion
GERD is an increasingly common and potentially serious condition with several predisposing factors and dental manifestations of which clinicians should be aware. An astute clinician can pick up the signs of these “silent refluxers,” thereby initiating treatment and referral to a specialist. Severe loss of palatal enamel due to acid reflux leads to increased flexibility and weakening of anterior teeth, which leads to compromised form, function, and esthetics. Full-coverage restorations in these cases can prove to be detrimental. In actuality, sometimes the most elegant solutions are those that are simple and minimalistic in approach.
References
1. Grippo JO, Simring M, Coleman TA. Abfraction, abrasion, biocorrosion, and the enigma of noncarious cervical lesions: a 20-year perspective. J Esthet Restor Dent. 2012;24(1):10-23.
2. Spear F. A patient with severe wear on anterior teeth and minimal wear on posterior teeth. J Am Dent Assoc. 2008;139(10):1399-1403.
3. Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101(8):1900-1920.
4. Pace F, Pallotta S, Tonini M et al. Systematic review: gastro-esophageal reflux disease and dental lesions. Aliment Pharmacol Ther. 2008;27(12):1179-1186.
5. Ranjitkar S, Smales R, Kaidonis J. Oral manifestations of gastoesophageal reflux disease. J Gastroenterol Hepatol. 2012;27(1):21-27.
6. Larsen MJ. Chemical events during tooth dissolution. J Dent Res. 1990;69(Spec issue):575-580.
7. Spear F. A patient with severe wear on the posterior teeth and minimal wear on the anterior teeth. J Am Dent Assoc. 2009;140(1):99-104.
8. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby, 2007.
9. Dahl BL, Krogstad O, Karlsen K. An alternative treatment in cases with advanced localized attrition. J Oral Rehabil. 1975;2(3):209-214.
10. Magne P, Magne M, Belser UC. Adhesive restorations, centric relation and the Dahl principle: minimally invasive approaches to localized anterior tooth erosion. Eur J Esthet Dent. 2007;2(3):260-273.
11. Fradeani M. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Vol. 1. Chicago, IL: Quintessence Publishing Co. Inc.; 2004.
12. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing Co. Inc.; 2002.
13. LeSage B, Milnar F, Wohlberg J. Achieving the epitome of composite art: creating natural tooth esthetics, texture and anatomy using appropriate preparation and layering techniques. J Cosmet Dent. 2008;24(3):132.
14. Sesemann MR. Systematic analysis of an anterior wear case to fulfill esthetic and functional objectives. Compend Contin Educ Dent. 2012;33(2):124-129.
About the Author
Aliasger Tunkiwala, MDS
Private Practice
Mumbai, India