You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Over the past few years, one article by the author that both garnered feedback and generated requests for further information was “The Role of Efficiency in Endodontic Care.”1 This is a follow-up to that original article that hopes to address some of the specific questions posed by readers. Therefore, this article will not only review some of the key points of the first article, but will additionally address some of the more specific questions of general dentists.
Efficiency: Key Concepts
We must begin with a review of some key concepts regarding efficiency and what exactly it is in the clinical sense. “Efficiency is defined as the ratio of useful energy delivered by a system to the total energy supplied to it. Essentially, analysis of the efficiency of a system measures the waste of effort by the system and compares how much effort will comparatively get the same results. Systems that produce less effort to produce the same output more quickly are considered to be more efficient.” 1 (Figure 1)
Although this explanation appears to be more applicable to mechanical engineering than endodontics, we must understand that an endodontic procedure, much like an engine, is a system composed of a collection of parts. Each part has a specific function. It is the relative functionality of each part and its congruent relationship with its counterparts that make the system synergistic and efficient, or inefficient, as a whole. If time and energy is lost during the process, we become less efficient at performing the procedure. But why is this even important?
The importance of efficiency in endodontics, much like all other healthcare fields, is related to the fact that most healthcare services are neither optional nor really desired by the patient. Much like a visit by the plumber, we may welcome it because of a need but would have preferred not to have the need to begin with. Understanding this helps motivate clinicians to invest in becoming more efficient.
Focusing on Quality Care
There is a false belief that efficiency in healthcare is associated with a lower quality of care. In fact, there is a distinct difference between performing a procedure quickly and performing the same procedure efficiently. The term efficiency assumes the same quality of care required to perform the procedure optimally, and therefore, higher efficiency should not mean a lower quality of patient care. This is why attaining an optimal outcome with less effort is generally more efficient than the same outcome achieved by more steps or unnecessary methods.
For example, if overnight delivery of packages by a company results into a higher rate of damaged packages than the normal delivery method, overnight delivery would only be a faster mode of delivery but not a more efficient one. Being fast is utterly useless if it means a diminution in quality. Consequently, to understand what efficiency truly means, we must comprehend the notion of skill.
“Skill may be defined as the conscious confluence of knowledge, desire, and practice. Gaining any skill is a function of having the desire to gain the necessary knowledge and further developing it through practice.”1 Therefore, one becomes skillful when one practices and hones a technique over time. Mastery in any field of practice, whether it is carpentry, poetry, gymnastics, or dentistry, seems to follow the same pattern. In endodontics, these principles, along with effective clinical skills, lead to optimal results.
Using Time and Energy Wisely
Efficiency of endodontic care (as with all other dental procedures) can be divided into two basic areas of service. The first is the efficiency in clinical procedures and the second aspect is efficiency associated with management of people. Basically, we’re trying to improve efficiency in managing techniques related to performing the clinical procedures and improving efficiency in managing people seeking those procedures.
The amount of mental energy to perform a procedure by any given operator is finite. The distribution of this energy to the procedure versus the patient is often a neglected point of discussion. Procedures are more efficient when the operator is allowed to focus more energy on the procedure than on the patient and his/her office staff. Therefore, establishing optimal guidelines to improve patient comfort throughout the appointment and having trained office staff that caters to the patient’s needs promptly frees the operator to focus more of his/her energy on the technical aspect of the procedure and less on psychological management of the patient. This helps improve technical efficiency.
This article will concentrate on the clinical aspects of endodontic efficiency as it relates to procedures, but truly efficient procedures combine efficiency of the clinical technique with management of the people seeking those procedures (patients) and those helping in delivering it (office auxiliary). These aspects of care are often inseparable. Efficient communication skills geared towards improving a patient’s understanding of the procedure and enhancing trust helps improve care acceptance and allows the operator to focus more of his/her energy on the procedure itself. A systematic approach to improving patient communication is always associated with patient-based practices exhibiting a higher rate of patient satisfaction with their overall experience.
Several clinical aspects of endodontic care can benefit from improvements in efficiency, including anesthesia, isolation, access, instrumentation, irrigation, obturation, and post placement in the tooth. Because an exhaustive review is beyond the scope of this article, the author will focus on those technique used in his clinical practice that help him with more efficient patient care. These are not the only techniques available to the profession but those that, in the author’s experience, work best in his hands and for his type of practice.
Endo–Restorative Continuum
Before discussing the clinical steps, it’s important to keep some concepts in mind. First, we must emphasize that the goal of endodontic therapy is not to save roots, but to reestablish a patient’s loss of health, function, and esthetics as a result of pulpal disease. Therefore, it’s important to consider the restorative aspects of any tooth requiring root canal therapy prior to considering the technical requirements of efficient root canal therapy.
A tooth with considerable biomechanical challenge due to loss of an extensive amount of coronal tooth structure or one with an unsound periodontal foundation due to persistent periodontal disease may not be a candidate for root canal therapy in the long run. Therefore, the most efficient procedure for a patient is one that considers the ultimate aim of saving a tooth in the context of the patient’s needs, requirements, and ideal vision of the desired outcome. An efficient root canal procedure that fails biomechanically in a short period of time due to a lack of consideration about the restorative requirement of the tooth reflects poor treatment planning. Focusing on the long-term outcome beyond the actual procedure is the first way you can improve efficiency of care, and outcome, for any given patient. In this treatment-planning phase, the employment of experienced specialists is important. Outcome assessment is often a result of years of experience. If a tooth’s salvageability is deemed questionable, consultation with an experienced endodontist prior to extraction is advisable. The same is true about the restorability of the tooth prior to endodontic treatment. A consultation with an experienced restorative dentist is always recommended. Experience is key, as true outcome assessment is a function of experiencing failures. The more failures a practitioner has seen, the more accurately he or she will be able to prognosticate the potential for failure of a given case.
The relationship between endodontic therapy and restorative dentistry can be described as the endo–restorative continuum.2 This relationship, like links in a chain, is only as strong as its weakest link. Unless potential challenges along this continuum are recognized and their implication communicated with the patient, postoperative management problems can arise.
Once the restorative aspects of care have been completely understood and its limitations have been clearly communicated with the patient, the next clinical area of challenge is anesthesia.
Anesthesia
Anesthesia appears to be an area where time is wasted without any gains in efficiency, but obtaining profound, definitive anesthesia is a considerable time saver throughout the procedure.3 Cutting corners and obtaining less than complete anesthesia will not only waste valuable time mid-operatively by attempting to reestablish effective anesthesia after a painful incidence, it also creates a loss of confidence by the patient regarding the surgeon’s skills and the quality of care rendered.
Patients are skeptical about the level of comfort they would be expecting during an endodontic procedure. Any confirmation of such feelings will adversely create a patient management challenge and halt the procedure. Remember that all efforts to reduce the flow of energy into the patient management aspect of the procedure will enhance the flow of the energy into the procedure itself. Therefore, profound, definitive, and verifiable anesthesia is required prior to beginning the procedure to reduce such crisis and allow for uninterrupted flow of energy into the procedure.
The simplest way to ensure this is testing the tooth prior to beginning the access opening. This test can easily be done with a cold cotton pellet or a cotton swab sprayed with a refrigerant. Alternatively, an electric pulp tester can be used to determine that the tooth is anesthetized. Asking the patient whether the tooth or the lip are numb are very poor indicators of pulpal anesthesia.
Waiting long enough for effective anesthesia and being ready to move quickly to additional anesthetic techniques such as intra-ligamentary or intra-osseous—if conventional anesthesia fails testing—will save time in the long run. The author does not recommend counting on intra-pulpal anesthesia as a quick way to numb patients after anesthesia failure is recognized during access preparation as it is an extremely painful technique. Furthermore, the use of techniques that have poor duration of pulpal anesthesia, such as non-vasoconstrictor containing anesthetics or relying on the use of intra-ligamental or intra-osseous injections as the sole mode of anesthesia, are also not recommended. These techniques will not yield pulpal anesthesia durations long enough for full pulpectomy in multirooted roots, and are therefore not reliable. The time one “wastes” by administering a reliable, predictable, long-acting pulpal anesthesic is worthwhile, considering the exponential gain in efficiency when you have a comfortable patient throughout the procedure. The dramatic increase in patient satisfaction with the experience is a welcome bonus.
Isolation
Isolation is an additional area that has generated multiple questions, with a common one being: “Does applying a rubber dam slow down the procedure, and how important is it?” Good isolation is absolutely critical to a smooth flowing procedure for both the clinician and the patient. It also addresses the essence of clinical endodontics—namely, the removal of infected dentin and the prevention of bacterial ingress into the pulp.
For a procedure to be efficient, it also helps if it is easy to accomplish. A fine-gauge or, at most, a medium-gauge rubber dam with a frame already attached is an efficient way to isolate the tooth. In endodontics, isolating a single tooth is all that is needed, and therefore the additional 30 seconds it takes to isolate a tooth will save you minutes in fighting the tongue and saliva in the area. Leaving a saliva ejector under the dam or asking the patient to swallow by pressing their tongue against the roof of their mouth is often helpful.
Furthermore, the use of a rubber dam is the standard of care in the United States and its omission is an automatic instance of negligence. The use of more universal rubber dam clamps is helpful in keeping your armamentarium small. Most endodontists use three or four clamps for 90% of their procedures.
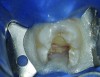
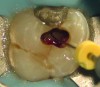
A key factor in efficiency is to be definitive in procedures. Much like anesthesia, isolation should also accomplish its goal definitively. When leakage occurs around the rubber dam, it potentially allows both contaminated crevicular fluid in the operating field as well as disinfectants into the patient’s mouth. The former can decrease the efficacy of care through contamination, and the latter will result into work stoppage to rinse the patient’s mouth, and therefore decreases efficiency. The use of rubber dam sealants around the clamp or open areas can helps prevent leakage (Figure 2). Furthermore, in severely angulated teeth or in some calcified teeth, accessing the tooth without the rubber dam helps decrease the chance of procedural errors such as perforation by improving alignment with adjacent teeth as well as visualization of coronal relationships. Following access and discovery of the canals in such teeth, the rubber dam should then be applied prior to instrumentation.
Access
General practitioners sometimes ask, “How can I make my access as small as the one my endodontist makes?” Not only do specialists have more experience, but also very often they are using a microscope when creating access. In fact, the most common mistake is to make the access prep too small, which will only make the entire procedure more challenging. The clinical outcome will be less than desired and the process will surely be inefficient. The following tips may help ensure appropriate and efficient preparation.
“Spend 5 more minutes on access preparation and you will save 25 minutes overall.” This saying describes the correct mentality when it comes to access preparation. Creating access is not just about getting a file to the canal orifice. Good straight-line access is directed towards the apex versus the orifice of the canal and aims to facilitate apical preparation and negotiation of curvatures in the most difficult part of the anatomy. Furthermore, good straight-line access allows the proper placement of the master cone without hanging up in the coronal third of the canal or in the pulp chamber. Thinking of access preparation as merely making a hole in the tooth should be avoided at all cost. The operator should think of good access as removing those coronal restrictions that ultimately makes possible the sliding down of a dead piece of gutta-percha all the way down to the apex and around its capricious curvatures. Otherwise stated, begin with the end in mind.
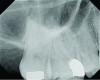
Micro-access preparations appear to be the trend right now. These significantly smaller access openings make the preservation of 1 mm of coronal dentin a higher priority than improving efficiency and increase the incidence of missed canals and separated files due to lack of visibility and lack of relief for coronal curvatures (Figure 4 through Figure 12). Basically, for preserving an additional millimeter of tooth structure on the access outline form, the procedure becomes more complicated and less predictable while increasing the overall chair time. Furthermore, scientific evidence does not exist to demonstrate what, if any, clinically significant benefit we gain for the additional millimeter of dentin we preserve. We do know that it will make exploration, instrumentation, and irrigation more difficult, however. Micro-access preparations complicate the root canal procedure unnecessarily, and for the complexity they introduce, the proponents do not validate any improvement in case outcome at the present time.
Micro-access preparations are a great example of a loss of efficiency based on increasing the complexity of a procedure without any assignable evidence of improved case outcome. This example seems to stand as a microcosm for many aspects of care recommended today. This is why the author believes that efficiency is always maximized when it is combined with the principle of economy.
To avoid missed canals in molars, a good rule of thumb to follow is to assume that all molars have four canals until proven otherwise. Please remember that mandibular molars are rectangular and maxillary molars are rhomboidal in shape, not triangular. The most commonly missed canal in a maxillary molar is the MB2 canal and in a mandibular molar is a second distal canal. Understanding the anatomy by sectioning numerous extracted teeth and familiarizing oneself with pulpal anatomy is a great step towards being more efficient at access preparation.
Instrumentation
The past two decades have seen an explosion in endodontic technology, mostly geared towards an improvement in the efficiency of care in the most challenging aspect of root canal therapy procedure: root canal instrumentation.
Clinicians face an increasing array of options when it comes to instrumentation. Although outcome assessment studies comparing various file systems are desperately needed, this area suffers from a paucity of scientific research. Although the shift from hand instrumentation to rotary nickel-titanium (NiTi) instrumentation has dramatically improved the efficiency of care, a measurable improvement in efficacy of care has not yet been demonstrated scientifically.4
As a result, the instrumentation options are based on bench top studies regarding each file’s material science rather than its actual contribution to case outcome. Therefore, clinicians are left to decide among an ever-increasing collection of instruments without much scientific support.
Most of the file systems out there achieve the same objective of shaping canals for obturation in relatively similar fashion. The differences are based on specific aspects of efficiency, versatility, safety, complexity, and price that each file system offers. Furthermore, the synchronicity of instrumentation with obturation is one of the primary motivators of this system and how it streamlines the process of canal instrumentation and obturation all the way to its restoration with a post and core. No matter what instrumentation system is used, its integration into a robust obturation system is necessary to improve efficiency.
The author’s own time–motion studies have shown that most of the time during root canal instrumentation is lost between changing files in the handpiece. Therefore, having multiple handpieces can help forego this necessity. This way, changing files would take no longer than changing hand instruments. This requires a greater upfront cost, but this cost is recaptured very quickly by the time saved not changing files and efficiently instrumenting the canal.
Furthermore, the author has noticed that when clinicians face the option of changing the file to a smaller size or pushing harder on the current file in the handpiece, most operator opt out of changing the file and push a little harder to move the file to length. This poor practice may work 75% of the time; but the 25% of the time when it results in a file fracture will drastically reduce efficiency and efficacy of the procedure. Therefore, creating an environment that facilitates the use of additional files when needed, such as having multiple handpieces loaded with different size files, will dramatically increase both your efficiency and the predictabilty of your outcomes.
Irrigation
Historically, root canal irrigation has been assigned the task of disinfecting the root canal during the shaping process prior to its obturation. However, irrigation should really be assigned two specific functions: removal of the gross debris and disinfection of shaped root surfaces.
The author recommends the use of ultrasonics with water throughout the procedure as the most efficient way to achieve the first objective. The ultrasonic energy delivered to water quickly removes debris generated by cutting dentin during the early phase of instrumentation.
Disinfection is needed once the gross debris has already been removed. At this time, the use of an effective disinfectant such as sodium hypochlorite is recommended. Because delivery of a high volume of disinfectant is a critical component of irrigation, and since sodium hypochlorite is toxic if inadvertently expressed beyond the root end, safe administration of this irrigant is critical. Although positive pressure systems (ie, injecting slowly from a side vented syringe tip that is loosely placed inside the root canal) have traditionally worked, newer negative pressure irrigation systems can help improve efficiency dramatically while improving safety.5 Negative pressure irrigation systems allow clinicians to express a high volume of disinfectant safely deep inside the canal.
Chelating agents such as EDTA, demineralizing acid such as citric acid, or lubricants approved for intracanal use may also help facilitate instrumentation by reducing drag on instruments and decreasing torque. Their excessive use should be avoided, however, as they can potentially soften dentin too much and facilitate ledging or perforations.
Obturation
Root canal obturation has been given excessive attention in the past few decades. This is primarily a function of the final radiograph being the only legally documentable evidence of an adequate or inadequately performed procedure. It is the last forensic evidence that allows for others attribute quality of care rendered by a clinician. Although the radiographic appearance of an obturation material is not a guarantee for successful outcomes, for better or worse, this procedural phase bears the clinician’s signature and is therefore an important part of the procedure.
All clinicians must recognize that cleaning and shaping are far greater determinants of success than obturation. Provided an equally good coronal seal, an inadequately cleaned and shaped case with the radiographic appearance of a dense fill will likely have a poorer long-term prognosis than one that is completely cleaned and shaped but inadequately obturated. This is because the radiodensity of a material has no bearing on its seal.
As a result, biocompatible and dimensionally stable obturation cements that bond chemically to dentin should be the logical choice over non-bonding cements with higher levels of radioopacifying agents for the purposes of creating the illusion of a better seal. Currently, the only chemically bonding root canal sealers that are biocompatible and dimensionally stable are the glass ionomer and bioceramic family of molecules.6 The problem with glass ionomers is their fast setting time and difficulty in obtaining a consistent mix. As a result, bioceramic cements are the modern cements with universal application in endodontics.7
The combination of bioceramic technology and coated bioceramic cones has simplified obturation through hydraulic condensation7 and has made the process significantly more efficient. When adequate cleaning and shaping has been performed, more complicated, time-consuming, vertical/lateral condensation, or various thermoplastic-based techniques can safely be replaced with hydraulic condensation to improve efficiency. This leap in obturation efficiency is now possible only as a result of improvements in sealer technology and introduction of true bioceramics sealers/fillers to the field.6,7
Restoration
Whenever possible, placement of the post and core should be done as soon as possible after the completion of the endodontic therapy. Provided that an adequate amount of confidence is justified following completion of the case, placement of a definitive restoration immediately after the root canal procedure may even be ideal. Placing a post and providing a bond for the post and core is better achieved under rubber dam isolation and immediately after the disinfection of the chamber, such as occurs during root canal therapy. Most often, the tooth is not isolated as effectively during the placement of a post and core as it is during the root canal. Therefore, bonding the post and core immediately will save time later with anesthesia, isolation, and another trip by the patient to the office. However, this step is primarily reserved for endodontists placing cores or highly experienced general dentists who have the ability to assess potential case outcome accurately immediately postoperatively.
Because placement of a post using almost all the post systems requires a post drill, a second visit is often required, as the sealer has to set prior to using a post drill. This is why the author uses a drill-less post system with fiber posts that match corresponding size endodontic files. This system foregoes the use of a post drill and allows for immediate placement of the fiber post.8 The post space can be prepared immediately by segmenting the gutta-percha using a previously described technique by the author.3 The synchronicity offered by this system of matching files, gutta-percha, paper points, and posts has efficiency built into the instrumentation, obturation, and restorative phases of the clinical procedure.
Conclusion
Efficiency is achieving the same outcome with less effort or in less time. It is not a shortcut that sacrifices quality for speed. Highly efficient systems are composed of a set of robust, predictable, and reliable functions that work synergistically to increase output for a given amount of energy. Time is not distributed equally in efficient systems. Spending additional time in certain steps can save more time in future steps. This is evident during delivery of a reliable anesthesia, deployment of a well-sealed isolation, and creating an ideal access.
Specific steps of care during the procedure should be definitive. Tentative decisions and unreliable steps severely reduce efficiency through increasing the rate of errors that require correction. Furthermore, iatrogenic errors such as perforations, ledging, file fractures, and inadequate fills may equally affect the efficacy of care.
Simplicity is the quintessential component of all robust and efficient systems. Today’s improvements in technology and material science have allowed for de novo synthesis of some of the old clinical concepts in endodontics. This modern science allows critical inquiry about the origin of ad hoc obturation concepts with hope of improving efficiency of care in this area. Further investigation validating the effect of added complexity for improving case outcome is desperately needed in the profession as a whole. Improvements in efficiency ultimately benefit both healthcare providers and patients alike.
References
1. Nasseh, AA. The role of efficiency in endodontic Care. Inside Dentistry. 2007;3(9):30-40.
2. Koch K, Brave D, Nasseh A. Bioceramic technology: closing the endo-restorative circle, part 2. Dent. Today. 2010;29(3):98-105.
3. Nasseh, AA. Considerations for ensuring complete anesthesia during endodontic care. Inside Dentistry. 2005;1(1):60-64.
4. Nasseh AA. Endodontic instrumentation options. Inside Dentistry. 2013;9(6):78-83.
5. Nielsen BA, Craig Baumgartner J. Comparison of the EndoVac system to needle irrigation of root canals. J Endod. 2007;33(5):611-615.
6. Koch K, Brave D. A new day has dawned: the increased use of bioceramics in endodontics. Dentaltown. April 2009:39-43.
7. Nasseh A. The rise of bioceramics in endodontics. Endodontic Practice. 2009;2:17-22.
8. Trushkowsky R. Fiber post selection and placement criteria: a review. Inside Dentistry. 2008;4:86-94.
About the Author
Allen Ali Nasseh, DDS, MMSc
President
RealWorldEndo™
Clinical Instructor
Department of Restorative Dentistry and Biomaterial Sciences
Harvard University School of Dental Medicine
Boston, Massachusetts
Private Practice
Boston, Massachusetts