You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Due to the large and growing percentage of patients with some type of edentulism, implant dentistry has seen accelerated progress in recent years. Data indicate that the adult population in need of one or two complete dentures will be close to 38 million in 2020.1,2 Under the right circumstances, implants are the method of choice to replace missing teeth, and should thus be considered for the treatment of partial and complete edentulism. However, implant surgery must satisfy prosthodontic needs and indications.3 Implant restorations can be fixated via a screw or an abutment with a screwed or overlaying cemented restoration, depending upon the type of retention desired or available. The choice between screw retention or cement retention often depends on the clinician’s preference.4,5 The proper diagnosis and correct execution of both the prosthetic and surgical phase of treatment planning is paramount to achieving optimal results.
The following are some of the issues to be considered.
Esthetics
Available residual bone and the resulting anatomy can hinder ideal implant position. In these cases, a cement-retained restoration with a custom or pre-angled abutment can be used to overcome this limitation.6
The access screw hole has been condemned as unesthetic in mandibular posterior areas or when the trajectory of the implant is facial in anterior areas. Cement-retained restorations offer a solution for this type of problem and permit greater freedom in implant positioning.
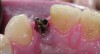
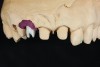
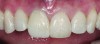
However, screw-retained restorations can still be placed when the trajectory and implant position are interfering with esthetic areas without compromising the final results (Figure 1). What is needed for this is excellent laboratory support and highly trained technicians who understand and can deliver this type of restoration.
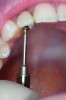
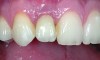
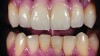
In this case, a prefabricated stock abutment was used. The abutment was milled to the desired height and width based on a diagnostic full-contour wax-up of the desired final restoration. Proper space for the crown materials and a desirable path of draw was achieved during the milling process. Then, the screw access hole was tapped on the palatal aspect of the restoration (Figure 2 through Figure 4). This achieves both the desired esthetics as well as retrievability and elimination of any subgingival cement that may affect the soft tissue.
This technique, which offers the advantage of being retrievable and avoids the biologic complications of cement-retained restorations, can also be used successfully for multiple restorations (Figure 5 and Figure 6).
Occlusion
Screw access holes on occlusal surfaces can cause disruption in the occlusal contacts during maximum intercuspation, and it has been suggested that they create offset loading forces. It has been stated that the access channel occupies a significant portion of the occlusal table.1,7,8 This occurrence may have a significant effect only when the implant system uses a larger screw for larger-diameter implants.1,3,6,7 Use in small dimension premolars may lead to the screw access hole occupying the majority of the occlusal surface, which can create both esthetic issues as well as difficulties in occlusion development.
Stable occlusal contacts can be established with cement restorations because there is no disruption of the occlusal surfaces.8,9
For anterior teeth, it is preferable for the crown that the access screw hole of the implant abutment be at the cingulum area and away from the incisal edge to properly support the metal or ceramic substructure.
In cases where the implant trajectory allows for proper screw retention, the access screw hole is not an important factor.6
The use of a surgical guide is paramount for single or multiple implant placements to ensure an ideally designed restoration. This is especially important in the maxillary anterior, where the trajectory of bone does not allow vertical placement of the implant body and does require some angulation.
A posterior implant is routinely placed at the center of the edentulous ridge, as the desired location and the access screw hole for the restoration should be at the center of the occlusal table. This is more important for screw-retained than cement-retained restorations, which allow for more latitude; without this, in some instances, periodontal-peri-implant health, esthetics, or maintenance may be compromised.
Screw-retained restorations require a minimum of 4 mm of inter-arch space from the implant platform to the occlusal surface of the opposing dentition. Cement-retained crowns need more interocclusal space to account for the multiple components used for their fabrication. For adequate retention of a cemented crown on an abutment, the abutment requires, at a minimum, 4 mm of height in the posterior. Anterior abutments will require greater heights, as the axial walls are more tapered than with posterior abutments, decreasing the retention available. There also has to be adequate space for the restorative material to be utilized in the crown, which typically requires approximately 2 mm. Thus, a minimum of 6 mm is required in the posterior, which will result in a fairly flat occlusal anatomy, and additional space is needed to develop anatomy that is lifelike.
Retreivability
The main advantage of the screw-retained restoration is the ease of delivery and retrievability without damaging the fixture or the restoration.1,3 Retrieval of a cement-retained crown, even when a provisional cement was used, may be difficult due to the lower degree of axial wall convergence than observed with natural teeth.
It was previously believed that for their long-term success, implant restorations had to be retrievable, but this concept has its historical origins in the dependence of the screw-retained components of the early implant systems.3 In the past, it was routine to remove the implant fixed prosthetics annually to clean the prosthesis. This concept has been abandoned due to lack of clinical evidence that this had positive effects on long-term success compared to not removing the prosthetics at recall appointments.
With the new advances in technology during the past three decades, implant systems have evolved, introducing new components with more prosthetic versatility.
For screw-retained implant-supported restorations, screw loosening was an issue in the past. However, better-designed implants, improved mechanical properties of the screws, improved internal connections, and tighter interfaces—with abutments functioning with a conical seal and practically no micro movement—are now setting the standard for optimal prosthetic connection.10 Routine use of torque wrenches has also assured that the fixation screw has achieved the manufacturers recommended torque, which has greatly decreased the incidence of screw loosening.
The lack of micro movement on the abutment during function prevents bacteria from pumping in and out of the implant abutment interface, thus helping preserve bone at the highest possible level, in addition to other factors such as the platform-switching design.11,12
Single-implant cemented crowns with a zirconia abutment in esthetics cases with thin biotype can provide excellent esthetic results (Figure 7 and Figure 8). Cement-retained restorations are indicated for single-unit and short-span fixed dental prostheses where retrieval is likely not to be necessary.3 Implant survival rates were similar for single units using screw-retained and cement-retained methods of fixation, respectively.13
Screw-retained restorations for single- and multiple-unit reconstructions have been reported to have lower prosthesis survival rates.11 This might be related to the occlusal design, leading to fracture of the veneering porcelain and screw loosening caused by a non-axial load that promotes bending moments, stress concentration, and micro movement.8,13,14
The advantage of retrievability seems to improve the implant survival rate for screw-retained restorations for full-arch fixed prostheses. Lower implant survival rates are reported when large-span restorations are fabricated with cement-retained components.14
The biologic complications reported in the literature for cemented implant components are higher when compare to screw-retained restorations. The cement component, when it is not properly removed, causes bone loss around the implant, and this complication increases with the span of the prostheses.14
The problem with the cemented restorations with subgingival margins is the lack of a good verification system that indicates the cement has been removed. Radiographic x-rays can only provide a mesial and distal picture, not a bucco-lingual one. Additionally, some cements are visible on radiographs, whereas others are radiolucent, making detection of any residual cement subgingivally very difficult. It is advantageous to use cement that is radiopaque to aid detection of extravasated cement in the peri-implant region to help reduce the incidence of cement-induced peri-implantitis.16
Cement restorations with a loose abutment screw are not always predictably removed; they need to be cut off to gain access to the underlying abutment screw, which can damage the restoration and require the fabrication of a new implant crown. The cost of time and fabrication are factors that need to be considered during the planning phase.
That screw-retained crowns offer direct access to the abutment screw or implant is an advantage over cement-retained restorations. When both techniques are compared, the amount of chair time and cost favor screw-retained over cement-retained restorations.
If there is a prosthetic complication, the amount of clinical and laboratory time involved and needed to repair cement versus screw-retained cannot be easily overlooked.
Passivity of Framework
Cement retention has been proven to be more passive than screw retention. This is attributed to the space created to account for the cement material.3,6
Regardless of the method of fixation, the fabrication of implant-supported restorations requires very precise techniques. Every step in the fabrication process can induce a small error that will affect the position of the implant prosthesis.2
Some authors have suggested that the accuracy of an implant impression can be affected by the divergence of multiple implants, and to a greater extent if these are internal connections versus an external hex connection. The type of impression material and the technique used can also lead to inaccuracies.7 This is only the first step of the process, which is followed by fabricating the master cast and wax pattern, investing, casting or milling, and firing porcelain, any of which could add even more distortion of the superstructure.7 Substructure fabrication has in recent years moved away from casting due to its inherent inaccuracies and potential weakness towards CAD/CAM-milled substructures. Computer designed and milled structures provide higher accuracy with regard to fit but also strength, as they are created from single blocks of material, eliminating solder joints or laser welds.
According to Karl and colleagues,17 there is evidence that both screw- and cement-retained frameworks always produce a measurable strain; therefore, passive fit cannot be achieved. It has been suggested that a strain of 3,000 or more is destructive and could result in bone resorption.15
The most common complications of non-passive–fitting frameworks are screw loosening, screw fracture, framework fracture, and implant fracture.7 Some authors also suggest the misfit of the prosthesis can lead to cupping bone loss around osseointegrated implants, but there is no conclusive evidence of this.3,8,18
Provisionalization and Immediate Loading
Screw-retained provisional restorations are preferred over those that are cement retained. Sculpting the peri-implant tissue is very important prior to delivering the final implant restoration. This helps to create a lifelike restoration.6 Additionally, screw-retained provisionals lock the prosthesis to the implants, eliminating the potential for a loosening of the prosthesis with the implants when a cemented provisional is used, which may go unnoticed until the immediate-loaded implant shows signs of failure.
Healing caps placed at the time of implant placement or during second-stage surgery often have a narrow diameter and lack the correct contours and emergence profile of the missing tooth.
The screw-retained provisional restoration can gradually mold the tissue around the implant with gently applied pressure (Figure 9). The blanching created at the time of provisional insertion should dissipate in less than 5 to 10 minutes. If the blanching is not monitored and the provisional restoration is left as is, exerting too much pressure could create recession and undesirable esthetic results.
For cement-retained provisional restorations, a polyether ketone (PEEK) prefabricated provisional abutment or a titanium implant cylinder modified with composite material at the gingival level should be prepped and customized for each tooth and specific situation. The provisional crown can then be cemented in. To avoid the biologic compromise caused by the cement, a finish line on the abutment must be prepared supragingivally, which could negatively impact esthetics results if the tooth to be restored is anterior.
From a surgical perspective, the authors recommend placing implants in extraction sockets with as much preservation of the buccal plate as possible to prevent tissue recession. They should be placed at least 3 mm apical to the free gingival margin of the adjacent teeth and 2 mm of the buccal plate to develop an adequate emergence profile. If cement is deposited in the gap around the body of the implant and the surrounding tissues, it could compromise the osseointegration.6
If the soft tissue around the implant needs modifications via second-stage surgery—such as a connective tissue graft or free gingival graft to improve the soft-tissue biotype—a screw-retained provisional restoration is preferred over a cement-retained provisional to avoid cement around the surgical site.6 It is recommended that these soft tissue needs be identified prior to implant placement and addressed at the time the implant is placed and screw-retained provisional used, when possible.
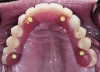
For a large-span or full-arch provisional prosthesis on immediate-load cases, a cement-retained prosthesis must be cemented with a definitive cement; if temporary cement is used, it can wash out, inducing micro movement during the early stages of osseointegration and cause implant failure. If definitive cement is used, the retrieval of the interim restoration is compromised, and no further adjustment can be made. Screw-retained provisionals for full-arch cases with immediate load or delayed load are preferred (Figure 10).
Screw retention provides the most rigid splint, preventing micro movement when multiple implants are immediately loaded.6 In addition, the interface of machined components is superior to any cement margin that can be developed.19
Ease of Fabrication and Costs
Cement-retained restorations are easier to fabricate than screw-retained restorations, because they follow traditional prosthetics techniques similar to those used for conventional crown and bridge prostheses.1,6-8 Components for these types of restorations are less expensive thanks to the advances in CAD/CAM technologies that allow for milled components with a more precise fit and lower costs.
Screw-retained restorations are more expensive because of the extra components needed. Machined components—such as uniabutments, angled abutments, fixation screws, and UCLA abutments—are needed for screw-retained restorations. These restorations are more demanding and technique sensitive from the laboratory perspective, but they offer multiple short- and long-term advantages.
Conclusion
Implant restorations require careful prosthodontic planning, even before the implant has been placed in the patient’s mouth. After placement, patients should be monitored during regular maintenance visits, during which the practitioner should check for bone loss, bleeding, and suppuration regardless of implant fixation type. Cement-retained restorations should be carefully assessed at each recall appointment due to their higher incidence of cement-induced peri-implantitis.
When either a prosthetic or surgical problem arises with a screw-retained restoration, which offers improved access, its correction requires less time chairside.
Certainly there is no right or wrong when selecting one type of connection over another, but clinicians need to be aware of the advantages and disadvantages of each type of prosthesis and make the appropriate decision based on the specific clinical situation.
References
1. Rola S, Nasrin S. A comparison between screw and cement retained implant prosthesis. A literature review. J Oral Implantol. 2012;38(3):298-307.
2. Douglas CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosthet Dent. 2002;87(1):5-8.
3. Taylor TD, Belser U, Mericske-Stern R. Prosthodontic considerations. Clin Oral Implants Res. 2000;11(Suppl 1):101-107.
4. Cutrim ES, Peruzzo DC, Benatti B. Evaluation of soft tissues around single tooth implants in the anterior maxilla restored with cemented and screw retained crowns. J Oral Implantol. 2012;38(6):700-705.
5. Vigolo P, Givani A, Majzoub Z, Cordioli G. Cemented versus screw-retained implant-supported single-tooth crowns: a 4-year prospective clinical study. Int J Oral Maxillofac Implants. 2004;19(2):260-265.
6. Chee W, Jivraj S. Screw versus cemented implant supported restorations. Br Dent J. 2006;201(8):501-507.
7. Michalakis KX, Hirayama H, Garefis PD. Cement-retained versus screw-retained implant restorations: a critical review. Int J Oral Maxillofac Implants. 2003;18(5):719-728.
8. Hebel KS, Gajjar RC. Cement-retained versus screw-retained implant restorations: achieving optimal occlusion and esthetics in implant dentistry. J Prosthet Dent. 1997;77(1):28-35.
9. Sherif S, Susaria SM, Hwang JW, et al. Clinician and patient reported long term evaluation of screw and cement retained implant restorations: a 5-year prospective study. Clin Oral Investig. 2011;15(6):993-999.
10. Zipprich H. Micromovements at the implant-abutment interface: measurement, causes and consequences. Implantologie. 2007;15(1):31-46.
11. Hansson S. Implant abutment interface: biomechanical study of flat top vs. conical. Clin Implant Dent Relat Res. 2000;2(1):33-41.
12. Baumgarten H, Cocchetto R, Testori T, et al. A new implant design for crestal bone preservation: initial observations and case report. Pract Proced Aesthet Dent. 2005;17(10):735-740.
13. Vigolo P, Mutinelli S, Givani A, Stellini E. Cemented versus screw retained implant supported single tooth crowns: a 10-year randomized controlled trial. Euro J Oral Implantol. 2012;5(4):355-364.
14. Gotfredsen K, Wiskott A. Consensus report – reconstructions on implants. The Third Consensus Conference 2012. Clin Oral Implants Res. 2012;23(Suppl. 6):238-241.
15. Nissan J, Narobai D, Gross O, et al. Long-term outcome of cemented versus screw-retained implant-supported partial restorations. Int J Oral Maxillofac Implants. 2011;26(5):1102-1107.
16. Pette G, Ganeles J, Norkin FJ. Radiographic appearance of commonly used cements in implant dentistry. Int J Periodontics Restorative Dent. 2013;33(1):61-68.
17. Karl M, Taylor TD, Wichmann MG, Heckmann SM. In vivo stress behavior in cemented and screw-retained five-unit implants FPDs. J Prosthodont. 2006;15(1):20-24.
18. Greenstein G, Cavallaro J Jr. Cantilevers extending from unilateral implant-supported fixed prostheses: a review of the literature and presentation of practical guidelines. J Am Dent Assoc. 2010;141(10):1221-1230.
19. Keith SE, Miller BH, Woody RD, Higginbottom FL. Marginal discrepancy of screw-retained and cemented metal-ceramic crowns on implant abutments. Int J Oral Maxillofac Implants. 1999;14(3):369-378.
About The Authors
Fernando J. Padron, DDS, FICOI
Prosthodontist
Oral Rehabilitation Center, P.C.
Skokie, Illinois
Sergio Rubinstein, DDS
Prosthodontist
Oral Rehabilitation Center, P.C.
Skokie, Illinois
Toshiyuki Fujiki, RTD
Laboratory Master Ceramist
Oral Rehabilitation Center, P.C.
Skokie, Illinois