You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
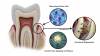
The goal of periodontal regeneration is to restore the cementum, a functionally oriented periodontal ligament, and any alveolar bone that was damaged or lost due to inflammatory destructive periodontal disease (Figure 1).1 Periodontal regeneration is most predictable in vertical, three-walled intrabony defects that have a narrow defect angle and an intrabony component that is equal to or greater than 5 mm in depth.2 The principles of periodontal regeneration require the exclusion of epithelial cells from the defect and the repopulation of the defect with periodontal ligament-derived mesenchymal stem cells. To facilitate this epithelial exclusion, clinicians have used several treatment modalities, including guided tissue regeneration with resorbable or nonresorbable membranes, bone replacement using bone graft materials (eg, demineralized freeze-dried bone allograft, freeze-dried bone allograft, anorganic bovine bone matrix), the use of osteopromotive growth factors, and combination therapies.2-4
Although many of these treatments have been shown to be effective in defects with ideal morphology,2,3,4 when challenging clinical scenarios present, clinicians should choose the most optimal grafting materials for each individual situation. Because each patient and site is unique, it is important for clinicians to understand the specific applications for adjunctive growth factors in periodontal regeneration, as well as their individual risks and benefits, and be able to provide evidence-based recommendations to deliver patient-centered care. Several available growth factors have been purported to be beneficial for periodontal regeneration.
Recombinant Human Platelet-Derived Growth Factor
During normal healing, a physiologic level of platelet-derived growth factor is derived from the platelets and serves as a nonspecific mitogen. Recombinant human platelet-derived growth factor BB (rhPDGF-BB), which is a laboratory-generated copy of the naturally occurring protein, has been shown to increase the migration of fibroblasts, cementoblasts, and osteoblasts to sites and to upregulate their activity.5,6 When used for periodontal regeneration, rhPDGF-BB acts as a chemotactic and mitogenic growth factor.5,6 It is often used in combination with xenografts and allografts in the treatment of intrabony defects. Studies in both animals and humans have demonstrated its potential for regeneration around teeth as well as dental implants.4-7 Overall, the use of rhPDGF-BB results in greater bone formation, decreased healing times, and improved periodontal clinical parameters when compared with the use of grafting technologies alone. 4-7
Platelet Concentrates
Platelet concentrates, such as platelet-rich plasma (PRP) and platelet-rich fibrin (PRF), are popular for intraoperative use. These autologous materials are derived from the patient's own blood and processed in-office with a centrifuge protocol specific to the product desired for use. Platelet concentrates contain an array of growth factors that are typically present during healing after injury.4,8 These growth factors are present in physiologic ratios, but at higher concentrations.4,8 In this manner, they can be osteopromotive and angiogenic. However, platelet concentrates generally require the use of bone grafting materials and a barrier membrane because they are neither cell-occlusive nor volumetrically stable.4 When used as an adjunct to traditional periodontal regeneration techniques, platelet concentrates deliver growth factor cascades and osteoblast precursors directly into the grafted site, which can increase bone turnover and decrease healing time.4,8
Vascular Endothelial Growth Factor
Vascular endothelial growth factor (VEGF) is the most potent known inducer of angiogenesis, and for this reason, it has been proposed as potentially useful for periodontal regeneration.9Animal studies have demonstrated that VEGF plays an important role in the formation of new bone by upregulating the chemotaxis of mesenchymal stem cells and enhancing the differentiation and proliferation of osteoblasts through its effects on osteoprogenitor cells.10 Further research regarding the isolation of VEGF and its direct use in periodontal defects is necessary prior to its approval by the US Food and Drug Administration (FDA) for clinical use.
Recombinant Human Fibroblast Growth Factor
Another adjunctive growth factor that has been used to enhance periodontal regeneration is recombinant human fibroblast growth factor-2 (rhFGF-2).11 The presence of rhFGF-2 increases the proliferation, migration, and differentiation of periodontal ligament cells as well as extracellular matrix production.11,12 It possesses a potent angiogenic and mitogenic capacity across a number of cell types.11,12 Because in vivo studies have demonstrated its ability to promote the proliferation and activation of osteoblasts, accelerating bone formation,12 it has been recommended for use in combination with allografts, xenografts, or alloplasts in the treatment of intrabony defects and peri-implant defects.11,12 The adjunctive use of rhFGF-2 has also demonstrated improved bone regeneration and faster soft-tissue healing postoperatively when compared with guided tissue regeneration alone.11 Currently, rhFGF-2 is not approved for use by the FDA, and further research to assess its safety and efficacy is warranted.
Enamel Matrix Derivative
Enamel matrix derivative (EMD) is composed of porcine-derived proteins, primarily amelogenin (ie, up to 90% by volume), that are isolated from the Hertwig's epithelial root sheath of developing tooth buds.13-15 Although EMD's mechanism of action is not well understood, it has been established that it stimulates osteoblast proliferation.15,16 Histological analyses have revealed that the use of EMD can result in true periodontal regeneration with the formation of new bone, cementum, and periodontal ligament on previously diseased root surfaces.17 In well contained intrabony defects, EMD can be used with or without a bone graft or a membrane because it is osteopromotive and also has cytostatic properties that impede epithelial downgrowth.15 It can also be used in defects in combination with a bone graft or a membrane, depending on the size of the defect and its morphology.2
Bone Morphogenic Protein
Bone morphogenic protein (BMP), or sialoprotein, was first described by Urist in 1965.18 BMP-2 and BMP-7 are the two most commonly utilized types of BMP in oral bone regeneration.19 Although the use of BMP in periodontal intrabony defects is not well studied due to the cost and potential complications associated with its use for periodontal regeneration, the use of BMP at sites adjacent to those proposed for guided bone regeneration may allow for additional bone deposition in the periodontal defect. Both BMP-2 and BMP-7 are processed by recombinant means utilizing mammalian cells.4 BMP increases the proliferation of osteoclasts and, subsequently, osteoblasts, the mineralization of osteoid, and the expression of alkaline phosphatase and osteocalcin.20,21 The use of BMP may be indicated in large bony defects in combination with a titanium membrane or in patients with systemic or anatomic limitations that can impair healing for whom successful bone regeneration would otherwise be difficult using normal guided bone regeneration techniques.20,21 It is used with bioactive carriers such as hydroxyapatite or allograft bone replacement graft materials.20,21 The use of BMP may not be indicated for intrabony defects due to the localized manner and size of the defects as well as its specificity to only form bone, which may lead to ankylosis. BMP is often used in horizontal and vertical guided bone regeneration and in sinus grafting; however, it can lead to a significant degree of extraoral swelling during the initial phase of healing, which may create postoperative discomfort and impact patient-centered outcomes.21
Teriparatide
Teriparatide is a systemic anabolic agent that is commercially available as a form of parathyroid hormone. It relies on low, intermittent doses delivered over an extended period of time to stimulate pre-osteoblasts and increase osteoblast proliferation. In addition, teriparatide indirectly acts on osteoblasts to decrease the rate of apoptosis.22 It has the potential to offer promising new technologies to aid in healing on a systemic level and may be appropriate for individuals who have a decreased capacity for osseous healing due to age or systemic disease.23,24 Additional research to determine the ideal patient characteristics and clinically related variables for the applicable adjunctive use of such emerging technologies may lead to FDA approval specifically for dentistry.
Summary
The adjunctive use of growth factors and biologic materials in guided tissue regeneration procedures for intrabony defects may facilitate enhanced outcomes and/or periodontal regeneration at sites with less than ideal healing potentials. To deliver personalized care and optimize periodontal regenerative potential, practitioners should assess the predictability of periodontal regeneration for each patient and site based upon clinical, radiographic, and patient-specific findings. Furthermore, the adjunctive use of biologic materials and growth factors to enhance healing may result in improved patient-centered outcomes, such as reduced discomfort and healing times and improved postoperative esthetics. In addition, their use may be especially beneficial in patients with systemic morbidities that impact healing capacity. A critical evaluation of all findings and a robust understanding of the underlying mechanisms of each adjunctive biologic factor will allow dental healthcare providers to choose a material that is best suited to each individual patient's specific circumstances.
Queries regarding this course may be submitted to authorqueries@aegiscomm.com
About the Authors
Jamie Howard, DMD, MS
Private Practice Limited to Periodontics and Implants
Hoover, Alabama
Amanda Piche, DDS
PGY2 Resident
University of Alabama at Birmingham
School of Dentistry
Birmingham, Alabama
Maria L. Geisinger,
DDS, MS
Diplomate
American Board of Periodontology
Professor and Director
Advanced Education Program in Periodontology
University of Alabama at Birmingham
School of Dentistry
Birmingham, Alabama
References
1. American Academy of Periodontology. Glossary of Periodontal Terms. AAP website. https://members.perio.org/libraries/glossary?_ga=2. 69735257.851429052.1591021245-217819958. 1589986601 &ssopc=1. Accessed October 13, 2020.
2. Kao RT, Nares S, Reynolds MA. Periodontal regeneration - intrabony defects: a systematic review from the AAP regeneration workshop. J Periodontol. 2015;86(2 Suppl):S77-S104.
3. Reynolds MA, Kao RT, Nares S, et al. Periodontal regeneration - intrabony defects: practical applications from the AAP regeneration workshop. Clinical Advances in Periodontics. 2015;5(1):21-29.
4. Suárez-López del Amo F, Monje A, Padial-Molina M, et al. Biologic agents for periodontal regeneration and implant site development. BioMed Research International. 2015;2015. doi: 10.1155/2015/957518.
5. Lynch SE, Williams RC, Polson AM, et al. A combination of platelet-derived and insulin-like growth factors enhances periodontal regeneration. J Clin Periodontol. 1989;16(8):545-548.
6. Nevins M, Kao RT, McGuire MK, et al. Platelet-derived growth factor promotes periodontal regeneration in localized osseous defects: 36-month extension results from a randomized, controlled, double-masked clinical trial. J Periodontol. 2013;84(4):456-464.
7. Lynch SE, Buser D, Hernandez RA, et al. Effects of the platelet-derived growth factor/insulin-like growth factor-1 combination on bone regeneration around titanium dental implants. Results of a pilot study in beagle dogs. J Periodontol. 1991;62(11):710-716.
8. Boyapati L, Wang H-L. The role of platelet-rich plasma in sinus augmentation: a critical review. Implant Dent. 2006;15(2):160-170.
9. Leung DW, Cachianes G, Kuang WJ, et al. Vascular endothelial growth factor is a secreted angiogenic mitogen. Science. 1989;246(4935):1306-1309.
10. Keramaris NC, Calori GM, Nikolaou VS, et al. Fracture vascularity and bone healing: a systematic review of the role of VEGF. Injury. 2008;39(Suppl):45-57.
11. Cochran DL, Oh T-J, Mills MP, et al. A Randomized controlled trial evaluating rh-FGF-2/B-TCP in periodontal defects. Journal of Dental Research. 2016;95(5):523-530.
12. Murakami S. Periodontal tissue regeneration by signaling molecule(s): what role does basic fibroblast growth factor (FGF- 2) have in periodontal therapy? Periodontology 2000. 2011;56(1):188-208.
13. Kao RT, Murakami S, and Beirne OR. The use of biologic mediators and tissue engineering in dentistry. Periodontology 2000. 2009;50(1):127-153.
14. Simmer JP, Fincham AG. Molecular mechanisms of dental enamel formation. Crit Rev Oral Biol Med.1995;6(2):84-108.
15. Esposito M, Grusovin MG, Papanikolaou N, et al. Enamel matrix derivative (Emdogain(R)) for periodontal tissue regeneration in intrabony defects. Cochrane Database Syst Rev. 2009;(4):CD003875.
16. Schwartz Z, Carnes DL, Pulliam R, et al. Porcine fetal enamel matrix derivative stimulates proliferation but not differentiation of pre-osteoblastic 2T9 cells, inhibits proliferation and stimulates differentiation of osteoblast-like MG63 cells, and increases proliferation and differentiation of normal human osteoblast NHOst cells. J Periodontol. 2000;71(8):1287-1296.
17. Mellonig JT. Enamel matrix derivative for periodontal reconstructive surgery: technique and clinical and histologic case report. Int J Periodontics Restorative Dent. 1999;19(1):8-19.
18. Urist MR. Bone: formation by autoinduction. Science. 1965;150(3698):893-899.
19. Chenard KE, Teven CM, He T-C, Reid R. Bone morphogenetic proteins in craniofacial surgery: current techniques, clinical experiences, and the future of personalized stem cell therapy. J Biomed Biotechnol. 2012;2012:601549. doi: 10.1155/2012/601549.
20. Kobayashi M, Takiguchi T, Suzuki R, et al. Recombinant human bone morphogenetic protein-2 stimulates osteoblastic differentiation in cells isolated from human periodontal ligament. J Dent Res. 1999;78(10):1624-1633.
21. Ripamonti U, Renton L. Bone morphogenetic proteins and the induction of periodontal tissue regeneration. Periodontol 2000. 2006;41(1):73-87.
22. Bashutski JD, Eber RM, Kinney JS, et al. Teriparatide and osseous regeneration in the oral cavity. New England Journal of Medicine. 2010;363:2396-2405.
23. Lin Z, Rios HF, Cochran DL. Emerging regenerative approaches for periodontal reconstruction: a systematic review from the AAP regeneration workshop. J Periodontol. 2015;86(Suppl 2):S134-S152.
24. Rios H, Bashutski JD, McAllister BS, et al. Emerging regenerative approaches for periodontal reconstruction: practical applications from the AAP regeneration workshop. Clinic Adv Periodontics. 2015;5(1):40-46.