You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
During the course of function, teeth may experience gingival recession to various degrees, which can lead to root exposure. Noncarious cervical lesions (NCCLs) may also be present alongside gingival recession defects, and the proper course of treatment for NCCLs or whether to treat these lesions at all is often debated. Similar debates arise when both the subjacent root structure and gingival recession is involved. In the United States, gingival recession has been reported in as many as 78% to 100% of middle-aged individuals and in as many as 22% to 53% of the teeth.1 In one study, the prevalence of 1 mm or more of recession on one or more teeth in the US population aged 30 years and older was 58%.2 Similarly, another study estimated that more than 50% of the US population has one or more teeth with at least 1 mm of recession.3 The prevalence of gingival recession is generally considered to increase with age.
Regarding NCCLs, one study reported their prevalence among older populations to be 46.7%.4 According to a study by Ceruti and colleagues, the overall prevalence of NCCLs is approximately 85%, and NCCLs affect approximately 18% of permanent teeth.5 The data indicated that the number of NCCLs increased with age and that posterior teeth were more frequently affected when compared with anterior teeth. NCCLs are characterized by a wedge- or V-shaped loss of tooth structure that commonly occurs on the facial surfaces of the teeth. This breakdown of tooth structure is not believed to be related to bacteria.6
Common surgical solutions to address gingival recession and NCCLs involve soft-tissue grafting using a variety of materials, including palatal tissue autografts and soft-tissue allografts, and incorporate various flap designs, such as envelope flaps, tunnel flaps, and vestibular and lateral approaches. Generally, each flap design presents unique advantages and disadvantages regarding root access, surgical trauma, and esthetics. The "frenectomy anterior tunnel sulcular access channel" flap design presented in this article is a novel approach that incorporates various flap designs to maximize esthetics, root access, and predictability in cases involving gingival recession and NCCLs in the maxillary arch.
Gingival Recession and NCCLs
According to the American Academy of Periodontology's Glossary of Periodontal Terms, gingival recession is defined as "the migration of the gingiva to a point apical to the cementoenamel junction (CEJ)," which exposes the root surface. Gingival recession is often associated with an underlying bony dehiscence and is more common in individuals with a thin periodontal phenotype.7
Etiology and Contributing Factors
The root causes of gingival recession, as well as NCCLs, are commonly debated, often without reaching a satisfactory conclusion. Recession is most commonly attributed to either a pathosis, such as periodontal disease; mechanical or chemical trauma; or parafunctional occlusion.6
There are several contributing factors often associated with root exposure, including deficiency in the alveolar bone, tooth shape, and the malposition of teeth, such as with crowding. In addition, mechanical trauma such as toothbrush abrasion can induce inflammation, which impacts the loss of gingival attachment. Other sources of trauma and inflammation that contribute to recession include forces from parafunctional behaviors, such as bruxism. And of course, plaque-induced periodontal disease can leave roots exposed as marginal inflammation and subsequent bone loss occurs.3
Classification Systems
When discussing root exposure, classification systems are helpful not only to facilitate consistent discussion but also to aid in determining the prognosis of teeth and in treatment planning. There have been many classification systems for gingival recession proposed in the literature, including those by Sullivan and Atkins, Miller, Cairo and colleagues, and others. In the Cairo classification system, the types of recession include the following8:
• Recession Type 1 (RT1). Gingival recession with no loss of interproximal attachment. The interproximal CEJ is not detectable clinically at both mesial and distal aspects of the tooth.
• Recession Type 2 (RT2). Gingival recession associated with loss of interproximal attachment. The amount of interproximal attachment loss (measured from the interproximal CEJ to the depth of the interproximal pocket/sulcus) is less than or equal to the buccal attachment loss (measured from the buccal CEJ to the depth of the buccal pocket/sulcus)
• Recession Type 3 (RT3). Gingival recession associated with loss of interproximal attachment. The amount of interproximal attachment loss is higher than the buccal attachment loss.
The classification of gingival recession is descriptive, so it is helpful in determining the proper course of treatment as well as in establishing expectations for treatment goals. Being able to accurately assess defects and anticipate the results of therapy are crucial in periodontal-restorative situations, where the sequence of treatment is important because it may be provided by various clinicians.
Typically, a thin periodontal phenotype is associated with a highly scalloped gingival architecture. The surrounding band of keratinized and attached gingiva may be narrow, and the marginal gingiva is often thin and delicate. The underlying bone is also thin and commonly associated with dehiscences or fenestrations in the labial plate. In contrast, a thick periodontal phenotype is typically characterized by a wide, flat gingival architecture with minimal scalloping. Here, a wider band of keratinized and attached gingiva is often found, and the marginal gingiva is thick and resilient. A thicker periodontal phenotype is also generally associated with thicker underlying bone. Clinically, the thin periodontal phenotype typically responds to insult or injury with recession of the gingiva, whereas the thicker phenotype is typically much more resistant to gingival recession.9
Regarding NCCLs, Winter and Allen describe them using the following four classifications10:
• NCL1. A less than 0.5-mm defect.
• NCL2. A 0.5-mm to 2-mm defect that does not involve the CEJ.
• NCL3. A 0.5-mm to 2-mm defect with loss of the CEJ and enamel contour.
• NCL4. A 2-mm or larger defect in the root with loss of cervical enamel.
Periodontal Treatment Planning
When considering periodontal treatment for gingival recession or cervical lesions, several factors may be considered. Ultimately, the long-term health of the periodontium is the primary goal. Therefore, examining the mucogingival complex should be a priority to ensure that there is an adequate amount of keratinized and attached gingiva for optimal health. Generally speaking, 2 mm of keratinized gingiva with 1 mm of attached gingiva is considered adequate.11 However, a recent study found that in a compliant patient group, the presence of 1.5 mm of keratinized gingiva was associated with a stable gingival margin after 10 years.12 The importance of adequate keratinized gingiva/attached gingiva is magnified when the tooth will be restored with a subgingival margin.13
Regardless of whether or not a tooth will be restored, there are several reasons why gingival recession and NCCLs may be treated with periodontal surgery. The benefits of periodontal plastic surgery procedures include improving access for oral hygiene procedures, decreasing the risk of root surface caries, and correcting gingival deformities. However, because these benefits can also be achieved through restorative therapies, it can sometimes be challenging to decide between periodontal surgery, restorative treatment, or a combination of the disciplines. Excellent communication between the dentist, specialist, and patient is vital to developing the appropriate treatment plan for each case.
Selecting a Flap Design
For root coverage surgery, a common debate in graft material selection is whether to use the patient's own tissue (ie, autograft) or tissue from another source, commonly a cadaver (ie, allograft). Clinical studies have shown both materials to be effective at reducing gingival recession.14 Other graft materials are commercially available as well, but because this decision largely comes down to the preferences of the surgeon and the patient, selecting the most appropriate flap design to treat multiple recessions may be more relevant to the success of the outcome, particularly in the maxillary anterior region where esthetics are critical.
When selecting a flap design for root coverage, clinicians should consider factors such as the presence of vital anatomic structures, the adequacy of the blood supply, root access, space maintenance for the incoming graft material, passive closure over the graft, esthetics, and more. There are several flap designs that can be used to address these challenges.
Envelope flaps,15 which are one of the most common flap designs, have the advantage of simplicity, blood supply, sulcular access to the roots to address NCCLs or for root preparation, and predictable root coverage (Figure 1). Because this flap design involves reflection of the papillae, it may affect papillary height upon healing. Envelope flaps may be utilized with vertical releasing incisions as a variation.
Another flap design, tunnel flaps,16 are very popular in esthetically demanding areas such as the upper anterior teeth due to their lack of papillae reflection, which preserves both the blood supply as well as the papillary height (Figure 2). Only sulcular incisions are utilized, and the graft is introduced over the root surfaces via a sulcular access. The disadvantages of tunnel flaps include increased technique sensitivity and the potential for complications, such as flap perforation, inadequate flap release to allow enough room for the graft materials, and passive closure over the gingival recessions. In addition, access to root surfaces may be a challenge because no flap is reflected to permit visualization.
Vestibular approaches (eg, vestibular incision subperiosteal tunnel access)17 are variations on tunnel flaps that address many of the challenges presented by the basic design (Figure 3). By making an incision in the vestibule, instruments may be passed beneath the mucoperiosteum to create space and passivity of the flap while minimizing the chances of creating perforations or tears in critical areas, such as the facial gingival margin. Depending on the size of the vestibular incision, either a sulcular access or vestibular access can be used for placement of the graft material. Unfortunately, because vestibular approaches are essentially still tunnel flaps, lack of root access remains an issue.
In order to take advantage of the benefits of the above-mentioned flap designs while minimizing the limitations, the frenectomy anterior tunnel sulcular access channel approach combines envelope flaps with a vestibular access tunnel by incorporating the maxillary midline frenum (Figure 4). This technique, which can be especially helpful for treating generalized recession affecting the upper anterior teeth, is demonstrated in the following case report.
Case Report
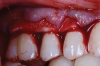
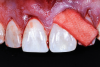
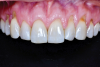
A female patient presented to the practice with generalized gingival recession in the maxilla that extended from tooth No. 4 to tooth No. 13 (her maxillary first premolars were missing). The recession was classified as Cairo RT1 for all affected teeth, and the root exposure ranged from 1 mm to 4 mm. As part of the examination, radiographs were acquired; however, no remarkable interproximal bone loss was observed (Figure 5). Teeth Nos. 4, 6, 10, 11, and 13 were the most severely affected, and NCCLs were present on the canines and premolars (Figure 6). More specifically, tooth No. 4 presented with 3 mm of recession and an NCCL; tooth No. 6 presented with 3 mm of recession and an NCCL; teeth Nos. 7 through 9 presented with 1 mm of recession and no NCCLs; tooth No. 10 presented with 4 mm of recession and an NCCL; tooth No. 11 presented with 4 mm of recession and an NCCL; and finally, tooth No. 13 presented with 3 mm of recession and an NCCL. All of the NCCLs demonstrated a Winter and Allen classification of NCL3. The patient's keratinized tissue was greater than 2 mm for all teeth, her periodontal phenotype was thick, and her midline frenum was prominent and inserted 5 mm apical to the tip of the papilla between teeth Nos. 8 and 9.
Development and Execution of the Flap Design
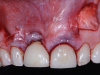
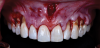
Given the importance of anterior esthetics as well as the clinical need for root access to address the NCCLs, no single flap design would suffice to solve the dilemma of esthetics versus root access in this case. And the presence of the patient's prominent midline frenum only added to the challenge of managing flap tension. Therefore, the proposed solution was a frenectomy anterior tunnel sulcular access channel approach. In this approach, a frenectomy procedure was performed to create a vestibular access point, followed by the creation of envelope flaps over the posterior teeth with gingival recession. This approach accomplished three goals: safe tunneling of the mucoperiosteal flap over the incisors without the need for papillae reflection, simple flap release over the teeth with gingival recession to provide space for the soft-tissue graft, and establishment of an easy access point to position the graft over the roots (Figure 7). Keeping the papillae between the incisors intact solved the esthetic concerns of the case, and the envelope flaps over the posterior teeth would permit the NCCLs to be reduced and smoothed with rotary instruments to provide a flat or concave surface for the graft material,10 which is very difficult or impossible with a tunnel flap. It is convenient that most NCCLs occur on posterior teeth5 because that allows an envelope flap for sulcular access and visualization to be incorporated with minimal effect on the esthetics. By combining a frenectomy with posterior envelope flaps for sulcular access, the frenectomy anterior tunnel sulcular access channel approach indeed creates a "channel" so that the soft-tissue graft can be placed over the roots from either direction and direct visual confirmation is possible to ensure proper placement (eg, no folding of the material, proper root coverage). If this approach was not used, one could imagine the challenges of properly placing the graft within a tunnel flap or through a single vestibular incision (Figure 8).
Placement of the Soft-Tissue Allograft and Closure
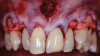
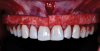
Mobility of the anterior tunnel portion of the flap was achieved by scoring the periosteum through the frenectomy incision. The flap release in the posterior envelope sections of the flap was achieved through the coronal (ie, sulcular) area. These steps were important to both create space for the graft material and ensure complete passive closure over the graft without excess flap tension. After this, the NCCLs were smoothed with rotary instruments to provide smooth, flat (or concave) surfaces. A soft-tissue allograft was then introduced through the frenectomy incision, passed through the "channel" over the incisors, and then retrieved through the envelope portion of the flap on both the left and right sides. After the graft was sutured to the CEJs with independent sling sutures using 4-0 chromic gut sutures (as can be seen in Figure 4), the overlying flap was coronally advanced over the allograft and sutured with independent sling sutures using 4-0 polypropylene sutures, and the frenum was closed with interrupted sutures also using 4-0 polypropylene sutures (Figure 9). To confirm passive closure of the flap, the patient's lips and cheeks were then manipulated in various directions. Care was taken to be sure that no allograft material was exposed.
Postoperative Care and Results
Postoperative care included dispensing an over-the-counter antimicrobial mouth rinse and a prescription for hydrocodone (5.0/325 mg) for pain. In addition, the patient was prescribed a 10-day course of amoxicillin (500 mg t.i.d.). It should be noted that this is outside the current antibiotic stewardship recommendations for postoperative antibiotic use, which indicate limiting the course to 5 days. The patient was instructed to avoid brushing or flossing near the gingival margin. Although the polypropylene sutures were removed at 2 weeks, the instructions to avoid brushing or flossing near the gingival margin remained in effect until 12 weeks. The patient was allowed to brush normally on the occlusal and lingual surfaces.
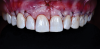
The patient's postoperative healing was uneventful. She reported light bruising; however, no bruising was observed at the suture removal appointment. She also indicated experiencing moderate pain but only during the first three days after surgery. By 12 weeks, nearly 100% root coverage was observed, and the quality of the tissue, which was thick, keratinized, pink, firm, and dense, remained stable. Inflammation was minimal, and the patient's oral hygiene was good. At the 1-year follow-up appointment, the observed results had been maintained and still demonstrated excellent esthetics (Figure 10).
Conclusion
Generalized gingival recession in the maxilla poses many challenges for clinicians. Although soft-tissue grafting is commonly the surgical treatment of choice, there are a number of possibilities regarding flap design. In the case report included in this article, selection of the frenectomy anterior tunnel sulcular access channel approach took into account the dental/oral anatomy, goals of treatment, and the skill/experience of the clinician to achieve an excellent result that was practical, efficient, and predictable. This flap design is best used in cases involving Cairo RT1 recession and NCCLs of any class.10 It may also be used with any amount of existing gingival thickness or width of keratinized tissue or even in the presence of frenum attachments; however, these anatomical considerations may affect the clinician's choice of graft materials.18 This novel flap design offers many benefits, but research is needed to evaluate the clinical results of its use in root coverage procedures, as well as changes to the periodontal phenotype, and compare it with the other established flap designs discussed in this paper and elsewhere in the literature. Furthermore, in this case report, a soft-tissue allograft was the material of choice. Research evaluating the results of various graft materials with this flap design is needed to assess if the results are comparable or perhaps even superior.
Queries regarding this course may be submitted to authorqueries@broadcastmed.com
About the Author
David H. Wong, DDS
Diplomate
American Board of Periodontology
Private Practice
Tulsa, Oklahoma
References
1. Gorman WJ. Prevalence and etiology of gingival recession. J Periodontol. 1967;38(4):316-322.
2. Albandar JM, Kingman A. Gingival recession, gingival bleeding, and dental calculus in adults 30 years of age and older in the United States, 1988-1994. J Periodontol. 1999;70(1):30-43.
3. Kassab MM, Cohen RE. The etiology and prevalence of gingival recession. J Am Dent Assoc. 2003;134(2):220-225.
4. Teixeira DNR, Thomas RT, Soares PV, et al. Prevalence of noncarious cervical lesions among adults: a systematic review. J Dent. 2020;95:103285.
5. Ceruti P, Menicucci G, Mariani GD, et al. Non carious cervical lesions. A review. Minerva Stomatol. 2006;55(1-2):43-57.
6. Bartlett DW, Shah P. A critical review of non-carious cervical (wear) lesions and the role of abfraction, erosion, and abrasion. J Dent Res. 2006;85(4):306-312.
7. Younes F, Eghbali A, Raes M, et al. Relationship between buccal bone and gingival thickness revisited using non-invasive registration methods. Clin Oral Implants Res. 2016;27(5):523-528.
8. Cairo F, Nieri M, Cincinelli S, et al. The interproximal clinical attachment level to classify gingival recessions and predict root coverage outcomes: an explorative and reliability study. J Clin Periodontol. 2011;38(7):661-666.
9. Jung RE, Sailer I, Hämmerle CH, et al. In vitro color changes of soft tissues caused by restorative materials. Int J Periodontics Restorative Dent. 2007;27(3):251-257.
10. Winter RR, Allen EP. Restorative and periodontal considerations for the treatment of noncarious cervical lesions. Adv Esthet Interdiscip Dent. 2005;1(4):24-28.
11. Lang NP, Löe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43(10):623-627.
12. Barootchi S, Tavelli L, Di Gianfilippo R, et al. Soft tissue phenotype modification predicts gingival margin long-term (10-year) stability: longitudinal analysis of six randomized clinical trials. J Clin Periodontol. 2022;49(7):672-683.
13. Stetler KJ, Bissada NF. Significance of the width of keratinized gingiva on the periodontal status of teeth with submarginal restorations. J Periodontol. 1987;58(10):696-700.
14. de Souza SLS, Novaes AB Jr, Grisi DC, et al. Comparative clinical study of a subepithelial connective tissue graft and acellular dermal matrix graft for the treatment of gingival recessions: six- to 12-month changes. J Int Acad Periodontol. 2008;10(3):87-94.
15. Zucchelli G, Mele M, Mazzotti C, et al. Coronally advanced flap with and without vertical releasing incisions for the treatment of multiple gingival recessions: a comparative controlled randomized clinical trial. J Periodontol. 2009;80(7):1083-1094.
16. Allen EP. Subpapillary continuous sling suturing method for soft tissue grafting with the tunneling technique. Int J Periodontics Restorative Dent. 2010;30(5):479-485.
17. Zadeh HH. Minimally invasive treatment of maxillary anterior gingival recession defects by vestibular incision subperiosteal tunnel access and platelet-derived growth factor BB. Int J Periodontics Restorative Dent. 2011;31(6):653-660.
18. Zadeh HH, Gil A. Coronally positioned flaps and tunneling. In: Nares S, ed. Advances in Periodontal Surgery. Springer; 2020:137-155.